Leishmania 101 - Sandfly's Surprise
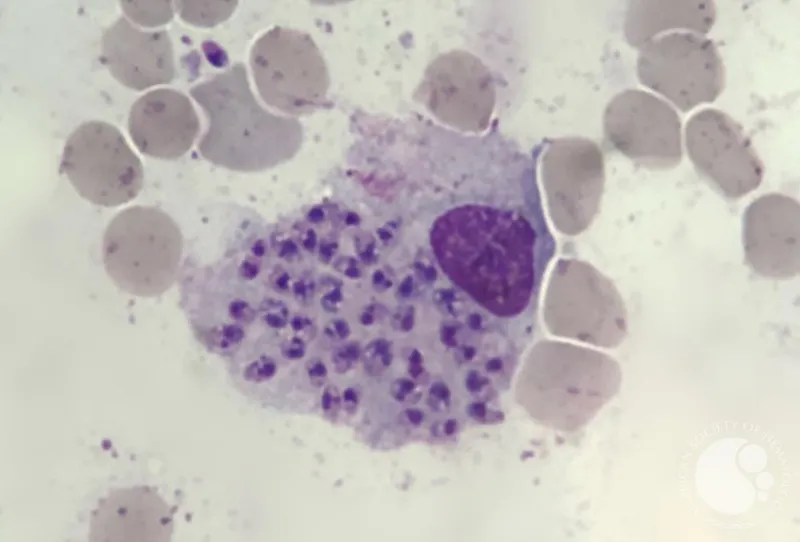
- Vector: Female sandfly; transmits infective, flagellated promastigotes.
- Lifecycle: Promastigotes are phagocytosed by macrophages and transform into non-motile, intracellular amastigotes.
- Syndromes:
- Cutaneous: Chronic, painless skin ulcers with indurated borders.
- Mucocutaneous: Destructive lesions of the nose and mouth.
- Visceral (Kala-azar): Spiking fevers, hepatosplenomegaly, pancytopenia, hypergammaglobulinemia.
- Treatment: Liposomal amphotericin B, sodium stibogluconate.
⭐ Diagnosis relies on identifying amastigotes within macrophages on a Giemsa-stained smear of bone marrow or spleen aspirate.
Lifecycle & Vector - A Bug's Journey
- Vector: Female sandfly (Phlebotomus or Lutzomyia species).
- Infective Form (to humans): Promastigote (motile, flagellated).
- Diagnostic Form (in humans): Amastigote (non-motile, intracellular) within macrophages.
- 📌 Mnemonic: Amastigotes are A-motile; Promastigotes are Pro-pelled.

⭐ Amastigotes, the intracellular form found within macrophages, are the key diagnostic finding on microscopic examination of tissue samples (e.g., skin biopsy, bone marrow).
Clinical Disease - The Three Faces
-
1. Cutaneous Leishmaniasis (CL):
- L. tropica, L. major, L. mexicana
- Presents as a painless, pink papule that enlarges into a nodule, then a well-demarcated ulcer with a raised, indurated border ("volcano sign").
- Usually heals spontaneously, leaving a depigmented scar.

-
2. Mucocutaneous Leishmaniasis (MCL):
- L. braziliensis
- Occurs months to years after a cutaneous lesion.
- Causes destructive, disfiguring lesions of the nasal septum, palate, and oropharyngeal mucosa (espundia).
-
3. Visceral Leishmaniasis (VL) / Kala-azar:
- L. donovani, L. infantum
- Systemic disease affecting the reticuloendothelial system.
- Classic triad: Spiking fevers, massive splenomegaly, pancytopenia.
- Associated with weight loss, weakness, and hyperpigmentation of the skin.
⭐ Diagnosis is confirmed by identifying amastigotes within macrophages in tissue specimens from bone marrow, spleen, or lymph node aspirates.
Diagnosis & Rx - Find and Fight
- Diagnosis:
- Microscopy: Key is identifying intracellular amastigotes (LD bodies) within macrophages on Giemsa/Wright-stained tissue smears (e.g., spleen, bone marrow).
- Culture: On Novy-MacNeal-Nicolle (NNN) medium.
- PCR: For definitive species identification.
- Treatment:
- Sodium stibogluconate: Traditional choice for cutaneous forms.
- Liposomal Amphotericin B: Drug of choice for severe/visceral leishmaniasis.
- Miltefosine: An effective oral agent.

⭐ Post-Kala-Azar Dermal Leishmaniasis (PKDL) can manifest as skin lesions months to years after successful visceral leishmaniasis treatment, acting as a disease reservoir.
High‑Yield Points - ⚡ Biggest Takeaways
- Leishmania is a protozoan transmitted by the sandfly; it exists as intracellular amastigotes in macrophages.
- Cutaneous leishmaniasis (L. tropica/mexicana) causes chronic, painless skin ulcers.
- Mucocutaneous leishmaniasis (L. braziliensis) leads to destructive lesions of the nose and mouth.
- Visceral leishmaniasis (L. donovani), or kala-azar, presents with fever, pancytopenia, and massive hepatosplenomegaly.
- Diagnosis relies on identifying amastigotes in tissue specimens.
- Key treatments include sodium stibogluconate and amphotericin B.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

