Filarial Nematodes - Thread-like Terrors
Filarial nematodes are tissue-dwelling roundworms transmitted by arthropod vectors like mosquitoes and flies. Adult worms mature over months in specific tissues (e.g., lymphatics, subcutaneous), releasing live offspring called microfilariae into the blood or skin. Pathology is primarily due to the host's inflammatory response to adult worms and the migrating microfilariae.
⭐ Diagnosis often requires timed blood smears due to the nocturnal or diurnal periodicity of microfilariae in peripheral blood, a key feature for species identification.

Lymphatic Filariasis - The Elephant in the Room
- Organisms: Wuchereria bancrofti, Brugia malayi.
- Vector: Mosquito.
- Clinical Presentation:
- Often asymptomatic.
- Acute: Adenolymphangitis (fever, painful lymph nodes).
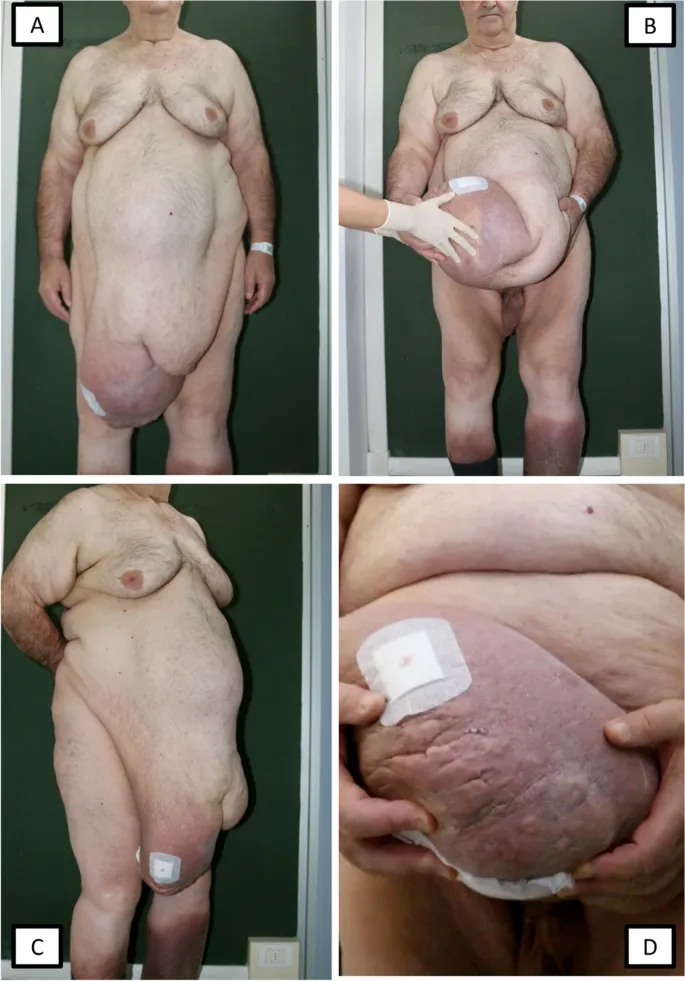
- Chronic: Lymphedema → Elephantiasis. Hydrocele in males.
- Diagnosis:
- Thick blood smear for microfilariae.
- 📌 Collect blood at night (nocturnal periodicity).
- Treatment: Diethylcarbamazine (DEC).
⭐ The diagnostic yield of blood smears is highest when collected between 10 PM and 2 AM due to the nocturnal periodicity of microfilariae in peripheral blood.
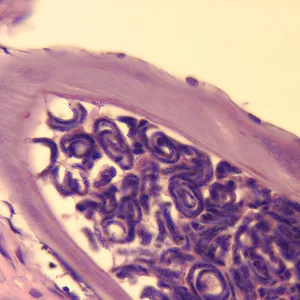
Onchocerca volvulus - Blinded by the Bite
- Organism: Onchocerca volvulus, a filarial nematode.
- Vector: Transmitted by the bite of a female blackfly, which breeds in fast-flowing rivers.
- Clinical Features:
- Onchodermatitis: Intense, pruritic papular dermatitis, leading to "lizard skin" or "leopard skin."
- Subcutaneous nodules (Onchocercomata): Palpable nodules containing adult worms.
- Ocular Lesions: Microfilariae in the cornea and anterior chamber lead to sclerosing keratitis, "river blindness."
- Diagnosis: Skin snip microscopy (bloodless) to visualize microfilariae.
- Treatment: Ivermectin.
- ⚠️ Avoid Diethylcarbamazine (DEC) due to the severe Mazzotti reaction (fever, hypotension, pruritus).
⭐ The intense itching is often more debilitating for patients than the blindness.
Loa loa & Dracunculus - The Wanderers
| Feature | Loa loa (African Eye Worm) | Dracunculus medinensis (Guinea Worm) |
|---|---|---|
| Vector/Transmission | Bite from Deerfly (Chrysops) | Drinking water with infected copepods |
| Clinical | Transient 'Calabar' swellings; worm migration across conjunctiva | Painful papule/blister on lower limb; emerging worm |
| Diagnosis | Microfilariae on daytime blood smear | Visualizing the emerging worm |
| Treatment | Diethylcarbamazine (DEC) | Slow, mechanical extraction |
⭐ Loa loa is associated with transient, localized angioedema known as 'Calabar swellings' due to host reactions to migrating adult worms or their metabolic products.
High‑Yield Points - ⚡ Biggest Takeaways
- Loa loa (eyeworm), transmitted by deer flies, causes transient Calabar swellings; treat with Diethylcarbamazine.
- Onchocerca volvulus, from blackfly bites, leads to river blindness and leopard skin; treat with Ivermectin.
- Wuchereria bancrofti & Brugia malayi are spread by mosquitoes and cause elephantiasis (lymphatic filariasis).
- Diagnosis relies on finding microfilariae on a thick blood smear (often at night) or skin snip (Onchocerca).
- Significant eosinophilia is a common lab finding.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

