Dysbiosis - Gut Feeling Gone Wrong
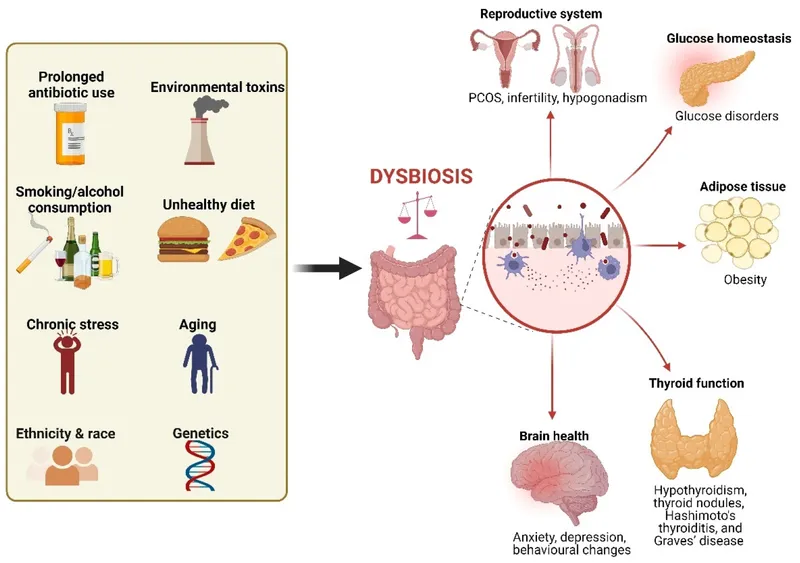
- Dysbiosis: A qualitative and quantitative imbalance in the normal gut microbial community, disrupting homeostasis.
- Common Triggers: Broad-spectrum antibiotics, proton pump inhibitors (PPIs), poor diet (↓fiber, ↑fat/sugar), psychological stress, and infections.
- Key Disease Associations:
- Gastrointestinal: Inflammatory Bowel Disease (Crohn's, UC), Irritable Bowel Syndrome (IBS), Clostridioides difficile infection, colorectal cancer.
- Metabolic: Obesity, Type 2 Diabetes, NAFLD.
- Systemic/Immune: Allergies, asthma, autoimmune disorders (e.g., rheumatoid arthritis), anxiety/depression (gut-brain axis).
⭐ Fecal Microbiota Transplant (FMT) is a highly effective therapy for recurrent C. difficile colitis, aiming to restore a healthy microbial community.
Disease Associations - The Gut-Body Axis Attack
- Metabolic Syndrome: ↑ Firmicutes/Bacteroidetes ratio linked to obesity & Type 2 Diabetes.
- Microbes affect energy harvest, fat storage, & insulin resistance.
- NAFLD/NASH: Dysbiosis drives liver inflammation.
- Cardiovascular Disease:
- Microbial Trimethylamine N-oxide (TMAO) from dietary choline/carnitine promotes atherosclerosis.
- Autoimmune/Inflammatory:
- IBD: ↓ diversity, ↑ pro-inflammatory bacteria.
- Rheumatoid Arthritis, Psoriasis: Systemic inflammation links.
- Neuropsychiatric (Gut-Brain Axis):
- Associated with anxiety, depression, ASD.
- Potential roles in Parkinson's, Alzheimer's.
- Cancer:
- Fusobacterium nucleatum linked to colorectal cancer.
⭐ Gut bacteria metabolize dietary choline and L-carnitine into Trimethylamine (TMA). The liver converts TMA to TMAO, a pro-atherogenic molecule that promotes foam cell formation and inhibits reverse cholesterol transport.
Clinical Sequelae - When Good Bugs Go Bad
Dysbiosis, an imbalance in normal flora, can precipitate disease by allowing pathogenic members to dominate or by compromising host defenses.
- Antibiotic-Associated Diarrhea: Broad-spectrum antibiotics (clindamycin, FQs, cephalosporins) deplete commensals, allowing Clostridioides difficile overgrowth.
- Pathogenesis: Toxin A (enterotoxin) and Toxin B (cytotoxin) disrupt the intestinal epithelium, causing pseudomembranous colitis.
- Bacterial Vaginosis (BV): Shift from protective Lactobacillus spp. to anaerobes (Gardnerella vaginalis). Presents with thin, gray discharge; fishy odor.
- Diagnosis: pH > 4.5, clue cells on microscopy, positive whiff test.
- Inflammatory Bowel Disease (IBD): Reduced microbial diversity is strongly linked to both Crohn's disease and Ulcerative Colitis.
- Opportunistic Infections: Flora breach their normal habitat.
- Bacteroides fragilis → Intra-abdominal abscess post-surgery.
- Viridans streptococci → Subacute bacterial endocarditis after dental procedures.
⭐ C. difficile toxins A and B inactivate Rho-family GTPases, leading to actin cytoskeleton disruption, cell death, and massive fluid secretion.

Diagnosis & Fixes - Restoring Gut Harmony
-
Diagnosis:
- Molecular analysis: 16S rRNA sequencing, metagenomics, and metabolomics to profile microbial composition and function.
- Culture-based methods are often insufficient for anaerobes.
-
Therapeutic Interventions:
- Probiotics: Introduce beneficial microbes (e.g., Lactobacillus, Bifidobacterium).
- Prebiotics: Fuel beneficial microbes (e.g., inulin, fiber).
- Dietary changes: ↑ Fiber and plant-based foods.
- Fecal Microbiota Transplant (FMT): Infusion of a healthy donor's microbiota.
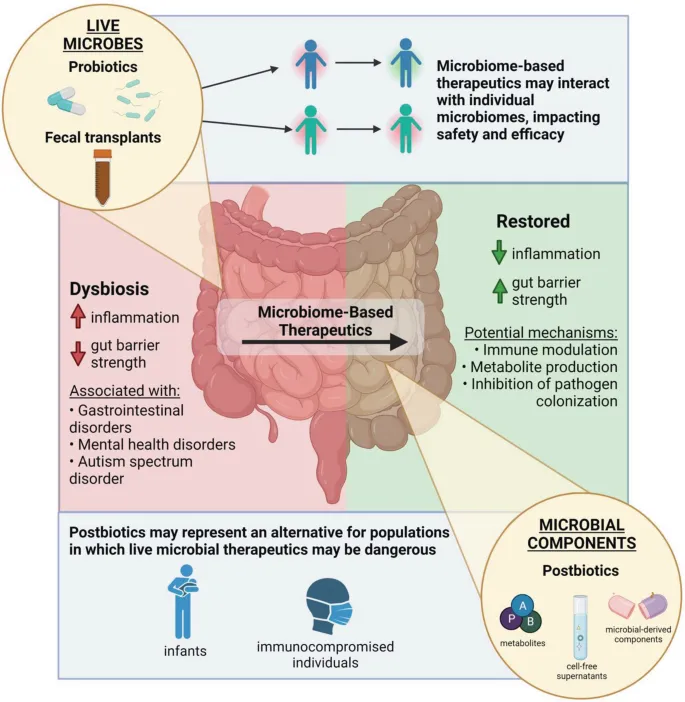
⭐ Fecal Microbiota Transplant (FMT) is a highly effective therapy for recurrent Clostridioides difficile infection, with cure rates often exceeding 90%.
High‑Yield Points - ⚡ Biggest Takeaways
- Dysbiosis is a pathogenic imbalance in the normal flora, often triggered by antibiotics, leading to disease.
- C. difficile overgrowth following antibiotic use (e.g., clindamycin) is the classic cause of pseudomembranous colitis.
- Bacterial vaginosis results from a shift from protective Lactobacillus to anaerobes like Gardnerella vaginalis.
- Gut dysbiosis is a key pathogenic factor in Inflammatory Bowel Disease (IBD).
- An altered Firmicutes/Bacteroidetes ratio in the gut is strongly associated with obesity and metabolic syndrome.
- Dental caries are driven by oral dysbiosis, primarily an overgrowth of Streptococcus mutans.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

