MDR Gram-Negatives - The Usual Suspects
-
Key Pathogens (SPACE-E):
- Serratia
- Pseudomonas aeruginosa
- Acinetobacter baumannii
- Citrobacter
- Enterobacter spp.
- Escherichia coli (not traditionally SPACE, but a major MDR threat)
- Klebsiella pneumoniae
-
Primary Resistance Mechanisms:
- Enzymatic Degradation: Extended-spectrum β-lactamases (ESBLs) & Carbapenemases (KPC, NDM, OXA).
- Efflux Pumps: Multi-drug efflux systems (e.g., MexAB-OprM in Pseudomonas).
- Target Modification/Protection: e.g., Porin loss to block antibiotic entry.
⭐ Carbapenem-resistant Enterobacteriaceae (CRE) infections can have mortality rates approaching 50%. Resistance is often carried on mobile genetic elements (plasmids), facilitating rapid spread.
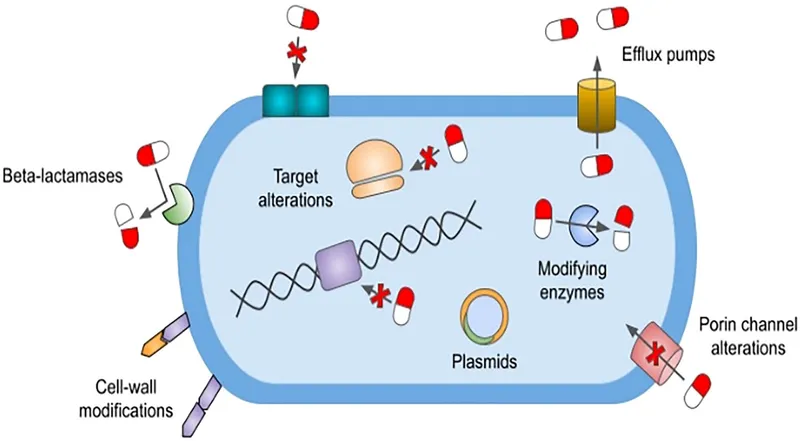
Resistance Mechanisms - Their Bag of Tricks
- Enzymatic Degradation: Bacteria produce enzymes that destroy the antibiotic.
- β-Lactamases: The most common mechanism against β-lactam antibiotics.
- ESBLs (Extended-Spectrum β-Lactamases): Inactivate most penicillins & cephalosporins.
- AmpC β-Lactamases: Chromosomally inducible or plasmid-mediated; resist cephamycins.
- Carbapenemases: Degrade carbapenems, the last-resort antibiotics (e.g., KPC, NDM-1, OXA).
- β-Lactamases: The most common mechanism against β-lactam antibiotics.
- Target Site Modification: Altering the drug's binding site reduces its efficacy.
- Examples: Changes in Penicillin-Binding Proteins (PBPs) → Methicillin resistance (MRSA).
- Reduced Permeability & Active Efflux:
- Porin Channel Loss: Decreased entry of antibiotics into the bacterial cell.
- Efflux Pumps: Actively pump the antibiotic out of the cell (e.g., TetA for tetracycline).
⭐ High-Yield: Carbapenemase genes are often located on plasmids, facilitating rapid horizontal transfer between different bacterial species and leading to widespread resistance.
📌 Mnemonic: Remember the core mechanisms with "E.A.T."
- Enzymatic degradation
- Altered target site
- Transport (reduced permeability/efflux)
Treatment Strategies - The Big Guns
- Core Principle: Use newer agents based on resistance mechanism, often requiring combination therapy.
-
Last-Resort Agents (High Toxicity):
- Polymyxins (Colistin, Polymyxin B): High rates of nephrotoxicity and neurotoxicity. Used when other options are exhausted.
- Tigecycline: Broad spectrum, but bacteriostatic. ⚠️ Increased mortality (black box warning); poor choice for bacteremia.
-
Other Key Agents:
- Cefiderocol: Siderophore cephalosporin; active against many CRE, including MBLs.
- Eravacycline, Omadacycline: Newer tetracyclines with activity against some resistant strains.
⭐ High-Yield: For severe CRE infections, especially those caused by metallo-β-lactamases (MBLs), combination therapy (e.g., ceftazidime-avibactam plus aztreonam) is often required as single agents may be ineffective.
High‑Yield Points - ⚡ Biggest Takeaways
- MDR gram-negatives are a major threat in healthcare settings, causing high-mortality infections like HAP/VAP and sepsis.
- Key pathogens: CRE (Carbapenem-resistant Enterobacteriaceae), MDR Pseudomonas, and Acinetobacter baumannii.
- Primary resistance mechanism: beta-lactamase enzymes (e.g., ESBLs, KPCs) that destroy most beta-lactam antibiotics.
- Resistance genes are typically on plasmids, allowing for rapid horizontal gene transfer between different bacterial species.
- Treatment often requires last-resort drugs like colistin, tigecycline, or newer beta-lactamase inhibitor combinations.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

