PrEP & PEP - Chemical Shields Up
-
PrEP (Pre-Exposure Prophylaxis): Ongoing ART for high-risk individuals to prevent HIV.
- Regimen: Daily oral tenofovir/emtricitabine (TDF/FTC or TAF/FTC).
- Indication: For individuals with ongoing, substantial risk of HIV exposure.
- Key: High adherence is critical for >99% efficacy in preventing sexual transmission.
-
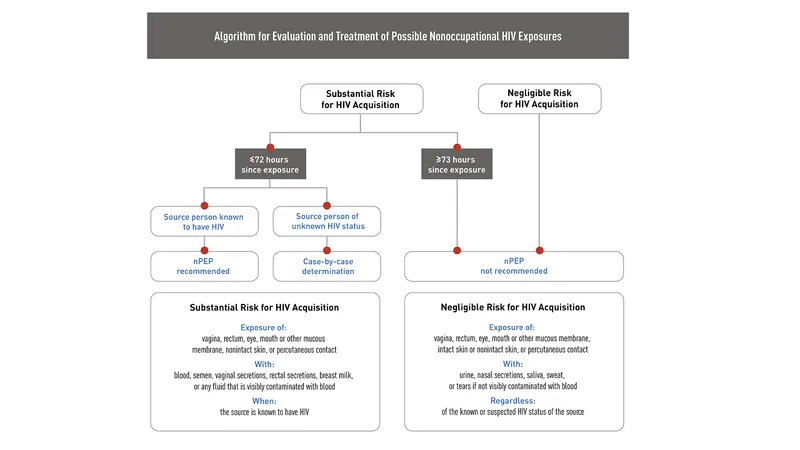
PEP (Post-Exposure Prophylaxis): Emergency ART initiated after a potential HIV exposure.
- Regimen: 3-drug ART course (e.g., TDF/FTC + dolutegravir/raltegravir).
- Duration: 28-day course.
- Crucial Timing: Must be started as soon as possible.
⭐ Initiate PEP urgently, ideally within hours of exposure, but no later than 72 hours. Efficacy declines significantly with delay.
Barriers & Behavior - Smart Choices Save
- Physical Barriers:
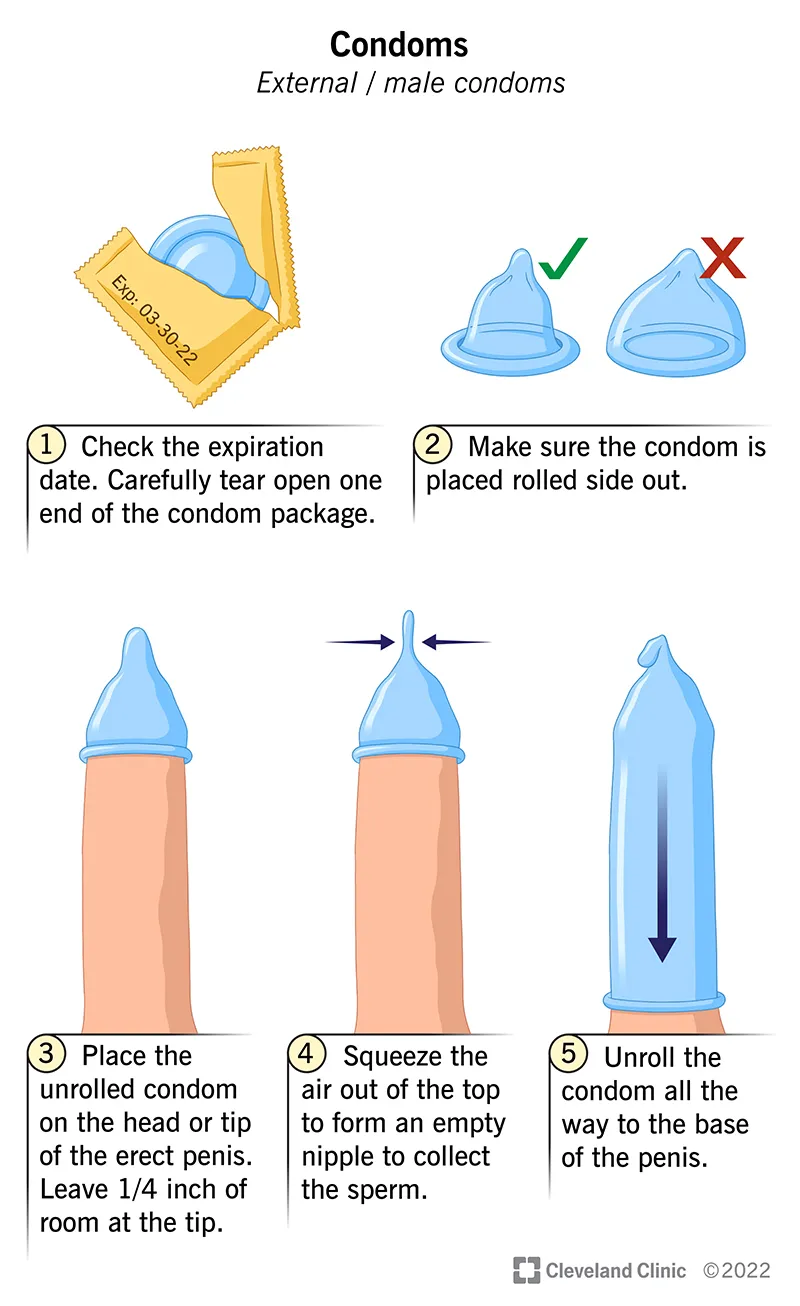
- Condoms (male/latex, female/polyurethane): Emphasize consistent & correct use for preventing sexual transmission.
- Harm Reduction (IVDU): Advise using sterile needles/syringes and avoiding equipment sharing.
- Behavioral & Procedural:
- Risk Reduction Counseling: Encourage limiting sexual partners and knowing their HIV status.
- STI Screening: Promptly diagnose and treat other STIs, as they can ↑ HIV transmission risk.
- Voluntary Medical Male Circumcision (VMMC): Reduces female-to-male transmission risk by ~60%.
⭐ Co-infection with other STIs (e.g., syphilis, herpes) significantly increases HIV transmission risk by disrupting mucosal barriers and causing inflammation.
Treatment as Prevention - Undetectable is Untransmittable
- Core Principle: Antiretroviral therapy (ART) suppresses HIV viral load to undetectable levels in the blood.
- Definition of Undetectable: Plasma HIV RNA level below the limit of detection of standard assays (typically <20-75 copies/mL).
- Clinical Implication: A person with a sustained undetectable viral load cannot sexually transmit HIV to others.
- Mnemonic: 📌 U=U (Undetectable = Untransmittable).
- This requires consistent ART adherence for at least 6 months to ensure stable viral suppression.
⭐ High-Yield Fact: The landmark HPTN 052 trial demonstrated that early initiation of ART by HIV-positive individuals reduced sexual transmission to their HIV-negative partners by 96%, cementing TasP as a cornerstone of HIV prevention.

Perinatal Prevention - Protecting the Newborn
- Universal HIV Screening: All pregnant women at the first prenatal visit.
- Maternal cART: Initiate combination antiretroviral therapy immediately for all HIV-positive mothers to reduce viral load.
- Goal: Achieve undetectable viral load (<50 copies/mL) before delivery.
- Intrapartum Care: Decision based on maternal viral load near delivery.
- Viral load >1,000 copies/mL: IV Zidovudine (ZDV) + scheduled C-section at 38 weeks.
- Viral load <1,000 copies/mL: Vaginal delivery is appropriate.
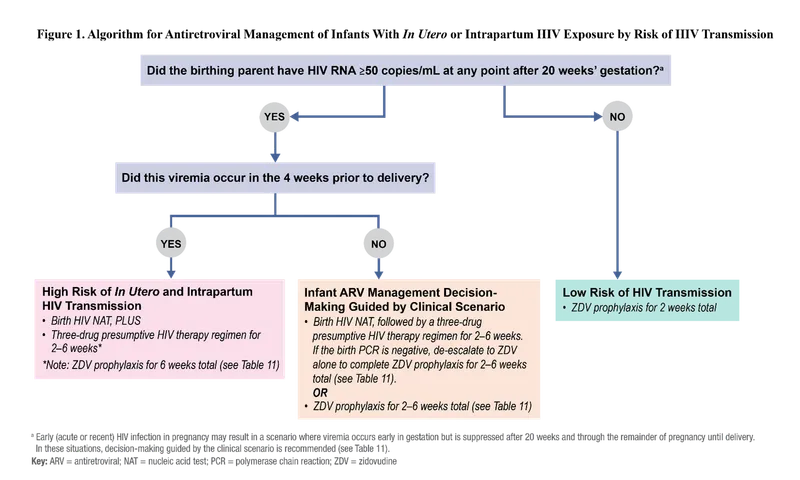
- Neonatal Prophylaxis:
- Low-risk infant: Zidovudine (ZDV) for 4 weeks.
- High-risk infant: Multi-drug ART.
- Infant Feeding: Avoid breastfeeding; recommend formula feeding.
⭐ With effective cART and appropriate management, the risk of mother-to-child HIV transmission is reduced from ~25% to <1%.
High‑Yield Points - ⚡ Biggest Takeaways
- Pre-exposure prophylaxis (PrEP) with tenofovir-emtricitabine is highly effective for preventing acquisition in high-risk individuals.
- Post-exposure prophylaxis (PEP), a multi-drug regimen, must be started within 72 hours of exposure.
- Treatment as Prevention (TasP): Antiretroviral therapy (ART) suppresses viral load to undetectable levels, preventing sexual transmission (U=U).
- Screening all pregnant women and providing maternal ART plus infant prophylaxis prevents vertical transmission.
- Harm reduction via condom use and sterile needle programs is critical.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

