MRSA - The Staph Superbug
-
Mechanism: The mecA gene encodes Penicillin-Binding Protein 2a (PBP2a). This altered protein has a low affinity for β-lactam antibiotics, conferring resistance by preventing their binding.
-
Clinical Syndromes:
- Community-Associated (CA-MRSA): Presents as skin/soft tissue infections (abscesses, boils). Virulence is often driven by Panton-Valentine Leukocidin (PVL) toxin.
- Hospital-Associated (HA-MRSA): Causes more invasive disease (bacteremia, pneumonia, endocarditis) in patients with recent healthcare exposure.
-
Diagnosis:
- Rapid: NAAT for the mecA gene offers fast identification.
- Culture: Chromogenic agar for screening; Kirby-Bauer testing with a cefoxitin disk confirms resistance.
⭐ The PVL toxin in CA-MRSA is linked to severe, necrotizing pneumonia, classically seen in healthy patients following an influenza infection.
VRE - Vexing Vancomycin Villain
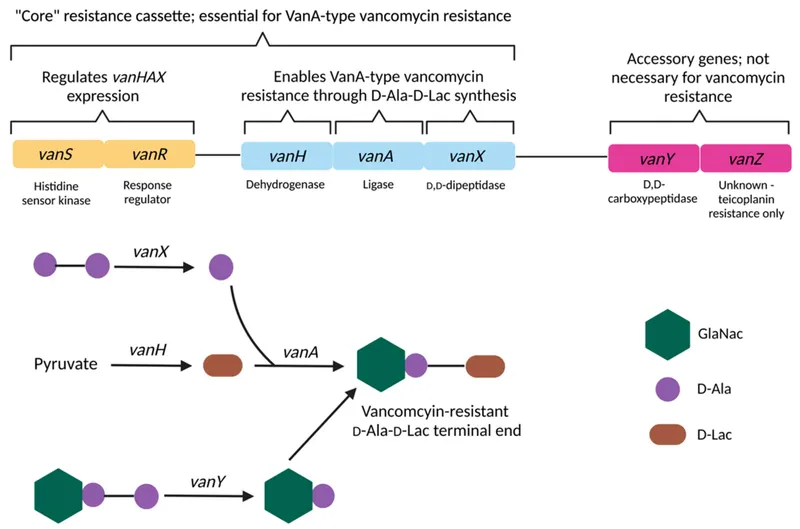
- Mechanism: Acquired vanA or vanB genes alter the peptidoglycan precursor target.
- Terminal $D-Ala-D-Ala$ is changed to $D-Ala-D-Lac$.
- This substitution prevents vancomycin from binding effectively.
- Predominant Species:
- Enterococcus faecium is more frequently vancomycin-resistant than E. faecalis.
- Key Risk Factors:
- Prolonged hospitalization or ICU stay.
- Long-term antibiotic therapy, especially with vancomycin.
- Clinical Syndromes:
- Nosocomial infections, including UTIs, bacteremia, and endocarditis.
⭐ VRE can transfer its resistance genes to other bacteria, such as S. aureus, leading to the emergence of Vancomycin-Resistant Staphylococcus aureus (VRSA).
Treatment - The Resistance Rumble
| Drug | Mechanism & Key Side Effect | MRSA | VRE |
|---|---|---|---|
| Vancomycin | Inhibits cell wall synthesis by binding D-Ala-D-Ala. → Red Man Syndrome, nephrotoxicity. | ✅ | ❌ |
| Daptomycin | Lipopeptide; depolarizes cell membrane. → Myopathy (monitor CPK). | ✅ | ✅ |
| Linezolid | Binds 50S subunit. → Thrombocytopenia, Serotonin Syndrome (risk with SSRIs). | ✅ | ✅ |
| Ceftaroline | 5th-gen cephalosporin; binds PBP2a. → Hemolytic anemia. | ✅ | ❌ |
| Tigecycline | Binds 30S subunit. → Severe nausea/vomiting; ↑ mortality warning. | ❌ | ✅ |
- MRSA resistance stems from the mecA gene, encoding an altered penicillin-binding protein (PBP2a), making it impervious to most beta-lactams.
- VRE resistance arises from the conversion of the peptidoglycan precursor from D-Ala-D-Ala to D-Ala-D-Lac.
- Key MRSA treatments include Vancomycin, Linezolid, and Daptomycin.
- For VRE, preferred agents are Linezolid and Daptomycin.
- Both are significant causes of nosocomial infections, particularly in immunocompromised patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

