Inclusion Criteria - The Green Light
- Age ≥ 18 years
- Clinical diagnosis of ischemic stroke causing measurable neurological deficit.
- Time from symptom onset to treatment is within 3 hours (standard window).
- An extended window of up to 4.5 hours is available for a select patient group.
- Blood pressure is controlled to <185/110 mmHg prior to and during IV alteplase administration.
⭐ The extended 3 to 4.5-hour window has stricter exclusion criteria, including: age > 80 years, NIHSS score > 25, or a history of both diabetes and prior ischemic stroke.
Exclusion Criteria - Absolute No-Gos
- Hemorrhage:
- Any prior Intracranial Hemorrhage (ICH)
- Active internal bleeding
- Known intracranial aneurysm, AVM, or neoplasm
- Recent Major Events (Time-Sensitive):
- Intracranial/intraspinal surgery or serious head trauma within 3 months
- Major non-head surgery or serious trauma within 14 days
- Vitals & Labs:
- Persistent BP > 185/110 mmHg despite treatment
- Platelet count < 100,000/mm³
- INR > 1.7 or elevated aPTT
- Specific Conditions:
- Suspected aortic arch dissection
- Infective endocarditis
⭐ Even if a patient's blood pressure is initially >185/110 mmHg, thrombolysis can be considered if the BP can be safely lowered and maintained below this threshold with medication.
Time Windows - The Ticking Clock
- "Time is Brain": The single most critical factor. The clock starts from the patient's Last Known Normal (LKN).
- Efficacy of IV thrombolysis is strictly time-dependent.
- 0-3 Hours (Golden Window)
- Highest benefit from IV Alteplase.
- 3-4.5 Hours (Extended Window)
- Stricter exclusion criteria apply:
- Age > 80 years
- Severe stroke (NIHSS > 25)
- History of both diabetes and prior ischemic stroke
- On any oral anticoagulant (regardless of INR).
- Stricter exclusion criteria apply:
⭐ The DAWN and DEFUSE-3 trials proved the benefit of mechanical thrombectomy for Large Vessel Occlusion (LVO) up to 24 hours post-LKN, using perfusion imaging to identify salvageable brain tissue.
High‑Yield Points - ⚡ Biggest Takeaways
- Time is critical: Administer tPA within 3 hours of symptom onset; can extend to 4.5 hours in select patients.
- BP must be <185/110 mmHg before and during infusion.
- Absolute contraindications include any prior intracranial hemorrhage (ICH), active bleeding, or arteriovenous malformation.
- Exclude for recent (<3 months) major surgery, serious head trauma, or prior stroke.
- Bleeding diathesis is a key exclusion: Platelets <100,000, elevated INR, or recent anticoagulant use.
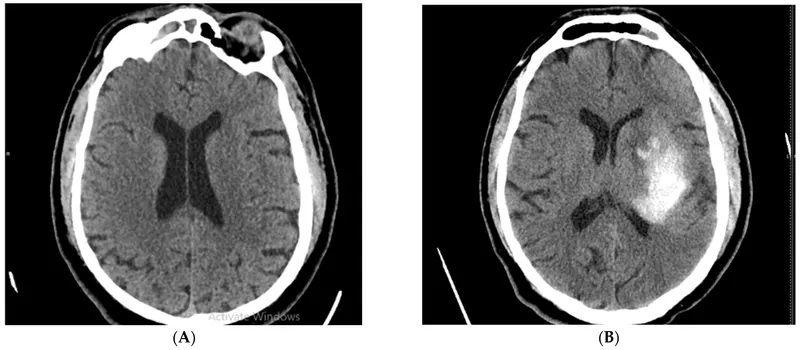
- CT findings: Exclude for signs of hemorrhage or a large established infarct (>1/3 hemisphere).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

