Initial Screening - The Bedside Gulp Test
- Goal: Screen all stroke patients for dysphagia before any oral intake to prevent aspiration pneumonia. Maintain NPO status until the screen is passed.
- Method: The bedside swallow screen (BSS), often the 3-oz (90 mL) water swallow test.
- Observe for: Coughing, choking, wet/gurgly voice, or oxygen desaturation during or after swallowing.
⭐ A failed bedside screen mandates keeping the patient NPO (nothing by mouth) and ordering a formal swallowing evaluation to prevent aspiration.
Formal Evaluation - Scopes & Swallows
Following a failed bedside screen, definitive instrumental tests are used to visualize swallow anatomy and physiology, guiding diet modification and therapy.

| Feature | Videofluoroscopic Swallow Study (VFSS/MBS) | Fiberoptic Endoscopic Evaluation of Swallowing (FEES) |
|---|---|---|
| Mechanism | Lateral view X-ray with barium-coated foods. | Flexible nasendoscope visualizes the pharynx. |
| Indication | Comprehensive assessment of all swallow phases. | Patient is immobile or requires frequent re-assessment. |
| Pros | Gold standard; visualizes aspiration during swallow. | Portable (bedside); no radiation; direct anatomy view. |
| Cons | Radiation exposure; patient must be transported. | Invasive; brief "whiteout" during swallow; misses oral phase. |
Management - Safe-Swallow Strategies
-
Diet Modification: Crucial for preventing aspiration pneumonia.
- Altering food textures (e.g., pureed, minced) and liquid consistencies.
- National Dysphagia Diet (NDD): Standardizes textures. Liquids are often thickened (e.g., nectar-thick, honey-thick) to slow flow, allowing more time for airway closure.
-
Compensatory Strategies: Immediate techniques to improve swallowing safety.
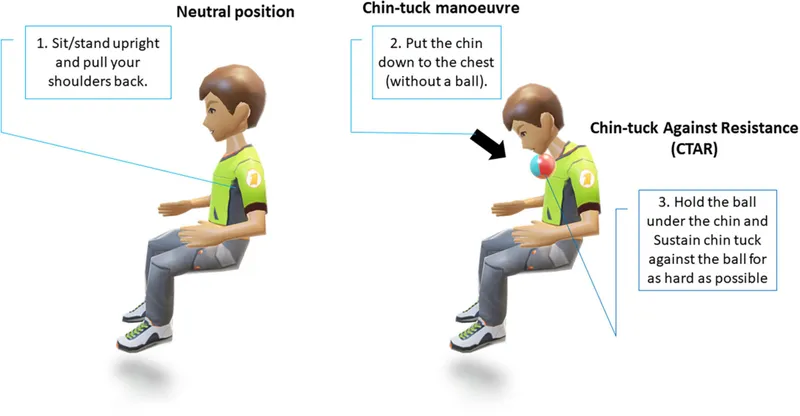
- Postural adjustments (e.g., head turn, chin-tuck).
- Altering bolus size and placement in the oral cavity.
⭐ The 'chin-tuck' maneuver is a simple but highly effective compensatory strategy that physically narrows the airway entrance, helping to protect against aspiration.
- Rehabilitation Exercises: Aim to restore long-term swallow function.
- Strengthening exercises for tongue, lips, and pharyngeal muscles (e.g., Masako maneuver, Shaker exercise).
Complications & Nutrition - The Danger Zone
- Aspiration Pneumonia: The most critical complication of dysphagia. Silent aspiration (no overt cough/choke) is common. Presents with fever, cough, and ↓O₂ saturation.
- Malnutrition & Dehydration: Result from inadequate oral intake, impairing recovery and increasing infection risk.
- Feeding Tube Management:
- Short-term (< 4-6 weeks): A nasogastric (NG) tube is used for initial nutritional support.
- Long-term (> 4-6 weeks): A percutaneous endoscopic gastrostomy (PEG) tube is indicated.
⭐ For long-term (> 4-6 weeks) dysphagia, a PEG tube is preferred over an NG tube to reduce the risk of sinusitis, esophagitis, and tube displacement.

- All stroke patients require a swallowing screen before any oral intake to prevent aspiration.
- Keep patients NPO (nothing by mouth) until this initial bedside assessment is passed.
- A failed bedside screen necessitates a videofluoroscopic swallowing study (VFSS), the gold standard for diagnosis.
- Aspiration pneumonia is a major complication of post-stroke dysphagia.
- Management includes dietary modifications (e.g., thickened liquids, pureed diet) and speech therapy.
- For severe dysphagia, consider enteral feeding via NG or PEG tube.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

