Initial Triage - Scan, Don't Speculate
Core presentation: Sudden onset of a focal neurological deficit. The immediate priority is to differentiate between ischemic and hemorrhagic types, as treatments are diametrically opposed.
- Clinical Features (FAST mnemonic 📌):
- Face Drooping
- Arm Weakness
- Speech Difficulty
- Time to call 911
| Feature | Ischemic Stroke | Hemorrhagic Stroke |
|---|---|---|
| Pathophysiology | Vascular occlusion (thrombus/embolus) | Vessel rupture & bleeding |
| Initial CT | Often normal initially (hypodensity later) | Hyperdense (bright) blood |
| Acute Goal | Restore blood flow (e.g., tPA, thrombectomy) | Control bleeding, ↓ICP |
Ischemic Stroke - The Clot Thickens
- Pathophysiology: Brain tissue death from ↓ blood flow, creating a pale infarct. Surrounding salvageable tissue is the ischemic penumbra.
- Etiology:
- Thrombotic: Local clot on an atherosclerotic plaque (e.g., carotid bifurcation).
- Embolic: Clot from a distant source (e.g., atrial fibrillation).
| Vessel | Area Supplied | Clinical Deficit |
|---|---|---|
| MCA | Lateral cortex | Contralateral face/arm weakness, aphasia (dominant), neglect (non-dominant) |
| ACA | Medial cortex | Contralateral leg weakness, personality changes |
| PCA | Occipital lobe | Contralateral homonymous hemianopia w/ macular sparing |
- Acute Management: Thrombolysis with tPA if within <4.5 hours; BP must be <185/110 mmHg.
⭐ Lacunar Strokes: Small vessel strokes in deep brain structures (basal ganglia, thalamus) from hyaline arteriosclerosis, often due to hypertension or diabetes. They cause pure motor or pure sensory deficits.
Hemorrhagic Stroke - A Bloody Mess
Results from vessel rupture and bleeding into brain parenchyma or the subarachnoid space, creating a "red infarct." Management focuses on controlling bleeding and intracranial pressure (ICP).
- Primary Causes:
- Chronic hypertension (most common for ICH)
- Ruptured saccular (berry) aneurysm (most common for SAH)
- Arteriovenous malformation (AVM)
| Feature | Intracerebral (ICH) | Subarachnoid (SAH) |
|---|---|---|
| Location | Brain parenchyma | Subarachnoid space |
| Cause | Hypertension, AVM | Aneurysm rupture |
| Presentation | Focal deficits, headache | "Worst headache of my life" |
| LP | Contraindicated (risk of herniation) | Blood/xanthochromia |
⭐ Xanthochromia (yellow CSF) on lumbar puncture is a classic sign of SAH, appearing 6-12 hours after the bleed due to bilirubin from RBC breakdown.
- The first and most critical step for all suspected strokes is a non-contrast head CT.
- Ischemic stroke: CT is often normal in the first 6-24 hours, later showing a hypodense (dark) lesion.
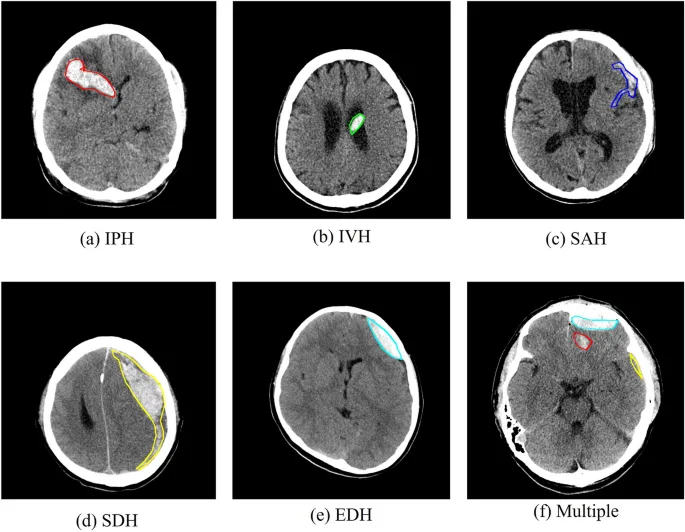
- Hemorrhagic stroke: CT immediately reveals hyperdense (bright) blood.
- Hemorrhage often presents with severe headache, vomiting, and altered mental status.
- This distinction is vital: tPA is for ischemic strokes and is contraindicated in hemorrhagic strokes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

