Pathophysiology & Diagnosis - The Failing Pump
- Vicious Cycle: A primary cardiac insult (e.g., large MI) drastically reduces contractility, leading to a sharp ↓ in Cardiac Output (CO) and subsequent hypotension.
- Maladaptive Compensation: The body's response-↑ sympathetic tone and ↑ Systemic Vascular Resistance (SVR)-paradoxically increases cardiac afterload and myocardial oxygen demand, which further impairs pump function and worsens ischemia.
- Diagnosis: Based on clinical signs of hypoperfusion (cool, clammy skin; altered mental status; oliguria) and congestion (JVD, rales).
- Hemodynamic Criteria (Invasive Monitoring):
- Systolic BP < 90 mmHg
- Pulmonary Capillary Wedge Pressure (PCWP) > 18 mmHg
- Cardiac Index (CI) < 2.2 L/min/m²
- Hemodynamic Criteria (Invasive Monitoring):
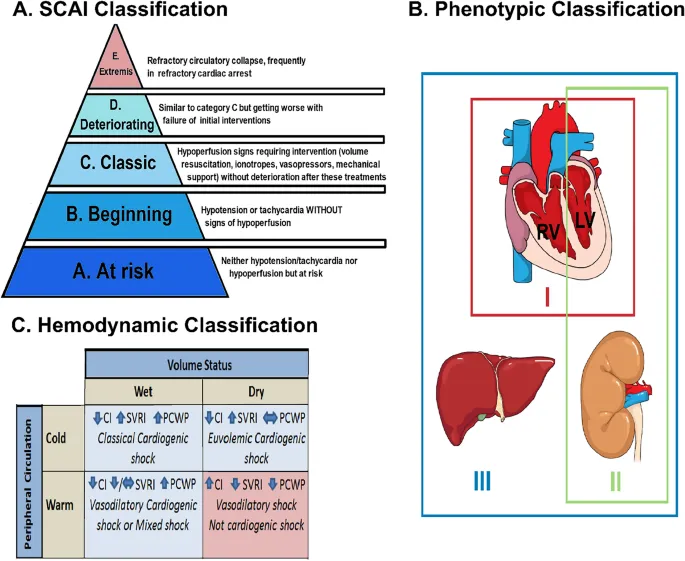
⭐ The classic hemodynamic signature is a low Cardiac Index (< 2.2) with a high PCWP (> 18), differentiating it from hypovolemic or distributive shock.
Initial Management - First-Response ABCs
- A - Airway: Assess patency. Low threshold for endotracheal intubation in patients with altered mental status or impending respiratory collapse to reduce the work of breathing.
- B - Breathing:
- Administer supplemental O₂ to maintain SpO₂ > 90%.
- Consider Non-Invasive Positive Pressure Ventilation (NIPPV) for acute pulmonary edema if the patient is alert and hemodynamically stable.
- Proceed to mechanical ventilation if NIPPV fails or is contraindicated.
- C - Circulation:
- Secure 2 large-bore peripheral IVs.
- Treat unstable arrhythmias (tachycardia/bradycardia) per ACLS.
- ⚠️ Judicious fluid challenge: 250-500 mL isotonic crystalloid only if no signs of fluid overload (e.g., pulmonary rales).
⭐ Unlike other shock types, large-volume fluid resuscitation is harmful in cardiogenic shock as it exacerbates pulmonary edema and cardiac strain.
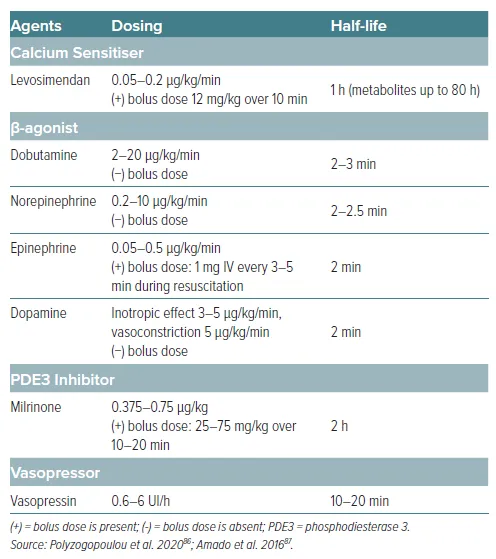
Pharmacotherapy - Potent Potion Push
-
Goal: Improve cardiac output (CO) & maintain mean arterial pressure (MAP) > 65 mmHg.
-
First-line therapy depends on blood pressure.
-
Key Agents:
- Norepinephrine: α1 > β1 agonist. ↑SVR, ↑MAP. First choice in hypotension.
- Dobutamine: β1 > β2 agonist. ↑CO, ↓SVR. Can cause hypotension. Use when BP is stable or with a pressor.
- Milrinone: PDE-3 inhibitor. Inodilator (↑CO, ↓SVR). Useful if patient is on beta-blockers.
- Diuretics (Furosemide): Use cautiously for pulmonary congestion if BP allows.
⭐ In cardiogenic shock with profound hypotension, norepinephrine is the initial vasopressor of choice. Dobutamine can be added once MAP is stabilized (>65 mmHg) to specifically improve cardiac contractility and output.
Mechanical Support - The Big Guns
- Intra-Aortic Balloon Pump (IABP):
- Mechanism: Counter-pulsation. Inflates in diastole (↑coronary perfusion), deflates in systole (↓afterload).
- Provides modest hemodynamic support.
- ⚠️ CI: Significant aortic regurgitation, aortic dissection.
- Percutaneous VADs (e.g., Impella):
- Mechanism: Axial flow pump actively pulls blood from the left ventricle to the aorta.
- Directly unloads the LV, providing superior support to IABP.
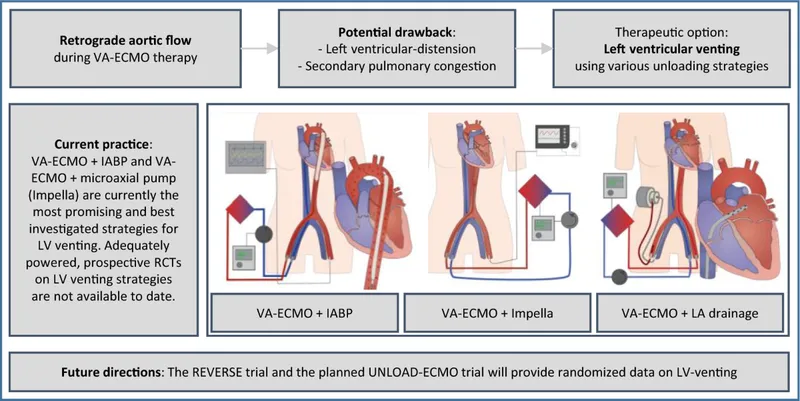
- VA-ECMO (Veno-Arterial ECMO):
- Provides full cardiopulmonary support; highest level of support.
⭐ VA-ECMO increases LV afterload, which can worsen pulmonary edema. May require LV venting (e.g., with an Impella).
High‑Yield Points - ⚡ Biggest Takeaways
- Cardiogenic shock is defined by low cardiac output and high PCWP (>18 mmHg).
- Initial stabilization may require inotropes (dobutamine) and vasopressors (norepinephrine).
- Use IV fluids cautiously or not at all, as they can worsen pulmonary edema.
- Definitive treatment targets the underlying cause, most commonly urgent revascularization for acute MI.
- Intra-aortic balloon pump (IABP) can serve as a bridge to definitive therapy.
- Avoid beta-blockers and nitrates during the acute hypotensive phase.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

