Pathophysiology & Triggers - The Reaction Ignition
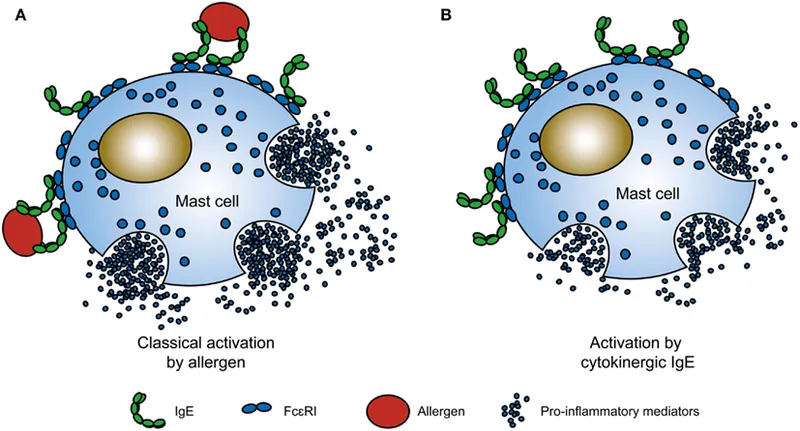
- Type I (Immediate) Hypersensitivity: Initial exposure to an allergen prompts IgE antibody production. Subsequent exposure leads to allergen cross-linking of IgE on mast cells and basophils.
- Massive Mediator Release: This triggers degranulation, releasing pre-formed mediators like histamine and tryptase, causing vasodilation, increased vascular permeability, and smooth muscle spasm.
- Common Triggers:
- Foods: Peanuts, tree nuts, shellfish, milk
- Medications: Penicillin, NSAIDs, anesthetics
- Insect Stings: Bees, wasps, fire ants
- Other: Latex, exercise
⭐ Serum tryptase is a specific marker for mast cell activation and helps confirm an anaphylaxis diagnosis, peaking 1-2 hours post-reaction.
Clinical Presentation - Signs of System Shock
Symptoms manifest rapidly, often within 5-30 minutes of allergen exposure across multiple systems.
- Cutaneous (~90%):
- Urticaria (hives), diffuse pruritus
- Angioedema (swelling of lips, tongue, face)
- Respiratory:
- Dyspnea, wheezing (bronchospasm)
- Stridor, hoarseness (laryngeal edema)
- Cardiovascular:
- Hypotension (SBP < 90 mmHg or >30% drop)
- Tachycardia, dizziness, or syncope
- Gastrointestinal:
- Nausea, vomiting, abdominal cramps
⭐ Be aware: Cutaneous findings may be absent in up to 20% of cases, especially in rapid-onset, profound shock.
Diagnostic Criteria - Nailing the Diagnosis
- Diagnosis is clinical. Any 1 of the following 3 criteria confirms anaphylaxis.
- Confirmatory Test: Serum tryptase can confirm the diagnosis retrospectively; levels peak 1-2 hours after reaction onset.
⭐ Hypotension is not required for diagnosis. The most common presentations involve skin and respiratory symptoms without a drop in blood pressure.
Acute Management - The Epi‑sode Response
Immediate Action: ABCs & Epinephrine
-
FIRST-LINE: Intramuscular (IM) Epinephrine is critical.
- Adult Dose: 0.3-0.5 mg (1:1000 solution) into anterolateral thigh.
- Pediatric Dose: 0.01 mg/kg (max 0.3 mg).
- May repeat every 5-15 minutes.
-
ADJUNCTIVE THERAPY:
- Antihistamines: H1 blockers (Diphenhydramine) + H2 blockers (Ranitidine/Famotidine).
- Glucocorticoids: (Methylprednisolone) to prevent biphasic reactions.
- Supportive: IV fluids for refractory hypotension; nebulized albuterol for bronchospasm.
⭐ A biphasic reaction (symptom recurrence 1-72 hours after initial resolution without re-exposure) can occur in up to 20% of patients. Observation is key.
Biphasic & Refractory - The Second Wave
- Biphasic Anaphylaxis: Symptom recurrence 1-72 hours post-resolution without re-exposure to the allergen.
- Refractory Anaphylaxis: Persistent symptoms despite receiving ≥2 doses of epinephrine.
- Management: IV epinephrine drip. Consider glucagon for patients on beta-blockers.
- Disposition: Observe patients for 4-8 hours after complete symptom resolution to monitor for a potential second wave.
⭐ Corticosteroids are administered with the aim of preventing biphasic reactions, though evidence for efficacy is varied.
High‑Yield Points - ⚡ Biggest Takeaways
- Anaphylaxis is a Type I (IgE-mediated) hypersensitivity reaction; requires prior sensitization.
- Intramuscular epinephrine is the first-line, life-saving treatment and should never be delayed.
- Airway compromise (stridor, hoarseness) is a primary cause of death; secure the airway early.
- Biphasic reactions can occur 1-72 hours after apparent resolution; always observe patients.
- Aggressive IV fluids are critical to counter distributive shock from massive vasodilation.
- Adjunctive therapies (antihistamines, corticosteroids) treat symptoms but do not replace epinephrine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

