Pathophysiology - The Great Hardening
- Core Triad: Autoimmunity, non-inflammatory vasculopathy, and collagen deposition with fibrosis.
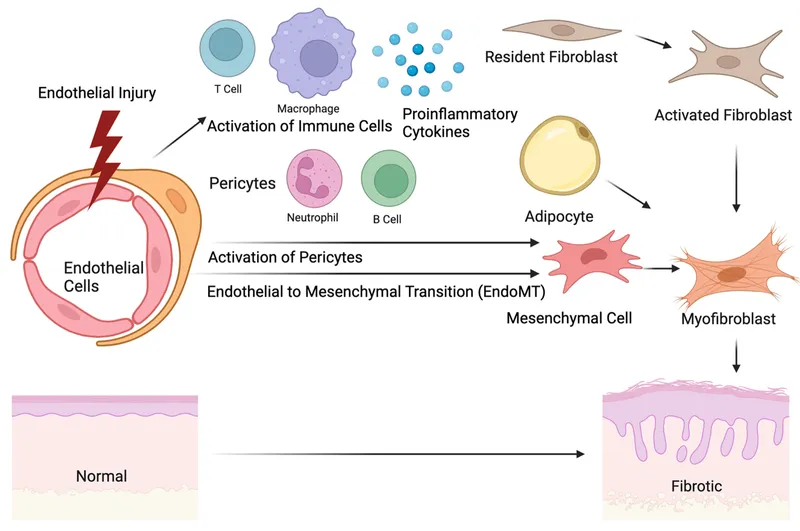
- Mechanism: An unknown trigger initiates endothelial/vascular injury, leading to inflammation.
- Activated T-cells release cytokines (TGF-β, IL-4, PDGF).
- These stimulate fibroblasts to overproduce collagen and extracellular matrix (ECM).
- Results in progressive fibrosis of skin and internal organs, plus vascular damage.
⭐ Anti-Scl-70 (anti-topoisomerase I) antibodies are strongly linked to diffuse cutaneous SSc and pulmonary fibrosis, highlighting the direct role of autoimmunity in organ damage.
Clinical Subtypes - Limited vs. Diffuse
| Feature | Limited Cutaneous (lcSSc) | Diffuse Cutaneous (dcSSc) |
|---|---|---|
| Skin Fibrosis | Distal to elbows/knees, face | Proximal & distal limbs, trunk |
| Progression | Slow, insidious | Rapid onset after Raynaud's |
| Organ Damage | Late, less severe (PAH) | Early, severe (ILD, renal crisis) |
| Antibodies | Anti-centromere (ACA) | Anti-Scl-70 (topoisomerase I) |
| Mnemonic | 📌 CREST Syndrome | - |
⭐ Diffuse scleroderma carries a worse prognosis due to rapid, severe involvement of internal organs like the lungs (interstitial lung disease) and kidneys (scleroderma renal crisis).
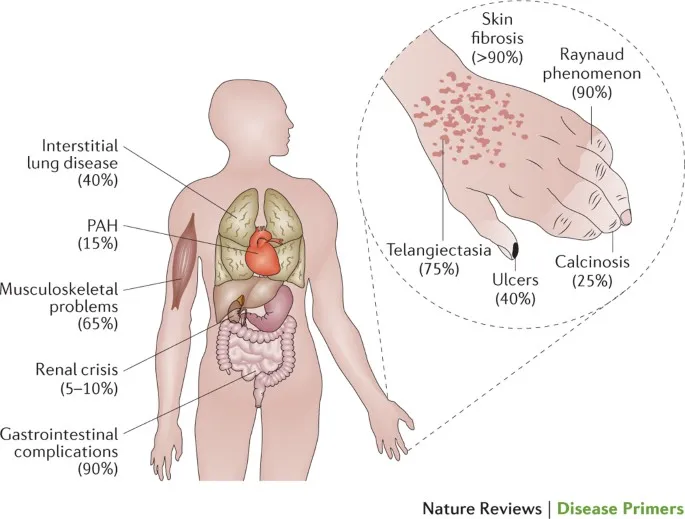
Organ Manifestations - An Inside Job
- Gastrointestinal (GI): Most common internal organ affected.
- Esophageal dysmotility → dysphagia, GERD.
- Gastric Antral Vascular Ectasia (GAVE) aka "watermelon stomach."
- Wide-mouthed diverticula.
- Pulmonary: Leading cause of mortality.
- Interstitial Lung Disease (ILD): Dry cough, dyspnea. NSIP pattern common.
- Pulmonary Arterial Hypertension (PAH): Screen with annual echo.
- Renal: Scleroderma Renal Crisis (SRC).
- Abrupt onset of severe hypertension and acute renal failure.
- Associated with anti-RNA polymerase III antibodies.
- Cardiac: Myocardial fibrosis, pericarditis, arrhythmias.
⭐ ACE inhibitors are the first-line treatment for Scleroderma Renal Crisis, even with an elevated creatinine.
Diagnosis - The Antibody Hunt
- ANA: Positive in >95% of cases (sensitive, not specific).
- Specific Antibodies (mutually exclusive):
- Anti-Scl-70 (anti-topoisomerase I): Linked to diffuse cutaneous (dcSSc) & severe interstitial lung disease (ILD).
- Anti-centromere: Strongly associated with limited cutaneous (lcSSc) / CREST syndrome.
- Anti-RNA Polymerase III: Tied to dcSSc, scleroderma renal crisis, and rapidly progressive skin thickening.
⭐ High-Yield: The presence of Anti-Scl-70 antibodies is a major red flag for aggressive diffuse disease and a higher likelihood of developing fatal pulmonary fibrosis.
Management - Damage Control
- Goal: Organ-specific therapy to halt fibrosis & dysfunction.
- Raynaud's: Dihydropyridine CCBs (e.g., Nifedipine).
- Scleroderma Renal Crisis (SRC): ACE inhibitors (e.g., Captopril) are critical.
- Interstitial Lung Disease (ILD): Mycophenolate mofetil (MMF), Cyclophosphamide.
- Pulmonary Arterial Hypertension (PAH): Bosentan, Sildenafil, Epoprostenol.
- GI Disease: PPIs for GERD; prokinetics for dysmotility.
- Skin Fibrosis: Methotrexate, MMF.
⭐ ACE inhibitors are first-line for Scleroderma Renal Crisis, even if creatinine is elevated. Withholding them is a major cause of mortality.

High‑Yield Points - ⚡ Biggest Takeaways
- Systemic sclerosis is an autoimmune disease causing widespread collagen deposition and fibrosis.
- Diffuse cutaneous (dcSSc) involves proximal skin and has a high risk of early interstitial lung disease; associated with anti-Scl-70 antibodies.
- Limited cutaneous (lcSSc), or CREST syndrome, primarily affects distal skin; linked to anti-centromere antibodies.
- Scleroderma renal crisis presents with malignant hypertension and requires urgent ACE inhibitor therapy.
- Pulmonary fibrosis and pulmonary arterial hypertension (PAH) are the leading causes of mortality.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

