Overview - Backbone Blues, No RF Clues
- Inflammatory arthritis of the axial skeleton (sacroiliac joints, spine).
- Key features: inflammatory back pain (improves with exercise, worse with rest), enthesitis (inflammation at tendon insertions), and dactylitis (“sausage digits”).
- Strongly associated with the HLA-B27 gene.
- 📌 Mnemonic PAIR: Psoriatic arthritis, Ankylosing spondylitis, IBD-associated arthritis, Reactive arthritis.
⭐ Seronegative means Rheumatoid Factor (RF) and anti-CCP antibodies are absent.
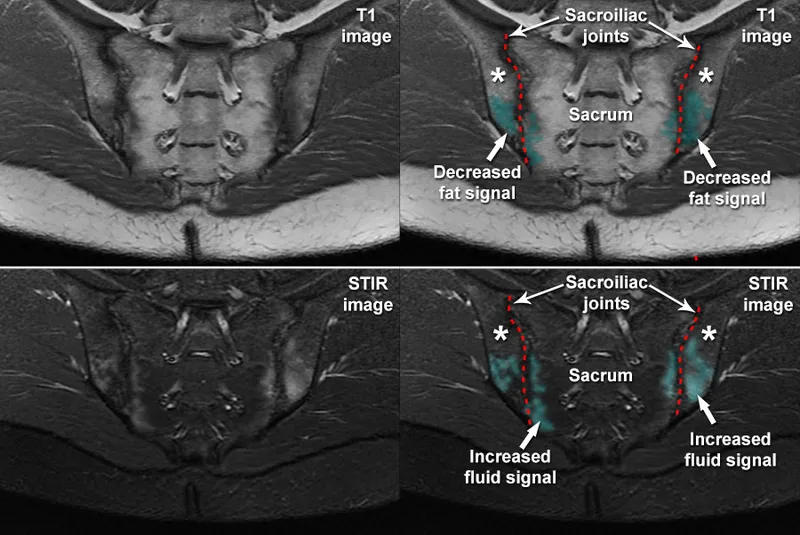
Ankylosing Spondylitis - Bamboo Spine, Aching Design
- Chronic, inflammatory arthritis of the axial skeleton and sacroiliac joints; strong HLA-B27 association (>90%).
- Presents in young men (<40y) with low back pain and morning stiffness that improves with activity.
- Key findings: sacroiliitis, syndesmophytes, and eventual spinal fusion (“bamboo spine”).
- Extra-articular features: anterior uveitis, aortitis, restrictive lung disease.
- Tx: NSAIDs, physical therapy, TNF-α inhibitors (e.g., infliximab).
⭐ Restrictive lung disease in AS is due to chest wall fusion and ↓ mobility, not interstitial lung disease.
Psoriatic Arthritis - Silvery Scales, Sausage Nails
- Asymmetric oligoarthritis, often with dactylitis (“sausage digits”) and enthesitis.
- Skin precedes arthritis in 80% of cases; look for psoriatic plaques (silvery scales on an erythematous base).
- Nail signs: Pitting, onycholysis, oil spots.
- X-ray hallmark: “Pencil-in-cup” deformity of DIP joints.
- Assoc: HLA-B27 (especially with axial disease).
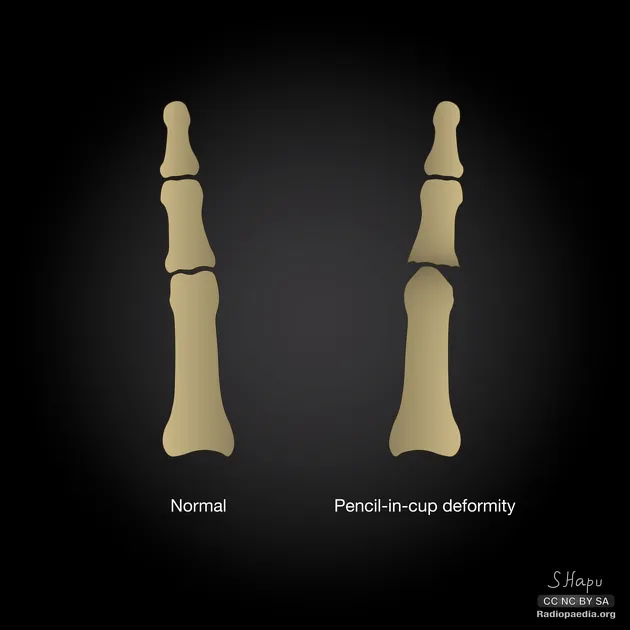
⭐ High-Yield: DIP joint involvement is classic for psoriatic arthritis, distinguishing it from Rheumatoid Arthritis.
Reactive Arthritis - Can't See, Can't Pee
- Seronegative spondyloarthropathy triggered 1-4 weeks after a GU (Chlamydia) or GI (Salmonella, Shigella, Campylobacter) infection.
- 📌 Classic Triad: "Can't see, can't pee, can't climb a tree."
- Uveitis/Conjunctivitis: Can't see.
- Urethritis/Cervicitis: Can't pee.
- Asymmetric Oligoarthritis: Can't climb a tree (joint pain).
- Also presents with enthesitis, dactylitis ("sausage digits"), and mucocutaneous lesions (keratoderma blenorrhagicum).
⭐ Strongly associated with HLA-B27.
Enteropathic Arthritis - Gut Feeling, Joint Squealing
- Arthritis associated with IBD (Crohn's, Ulcerative Colitis).
- Two patterns:
- Peripheral: Asymmetric, oligoarticular (≤4 joints), large joints. Arthritis activity often parallels gut flares.
- Axial: Sacroiliitis & spondylitis. Activity is independent of IBD activity; strong HLA-B27 association.
- Extra-articular signs: Erythema nodosum, pyoderma gangrenosum, uveitis.
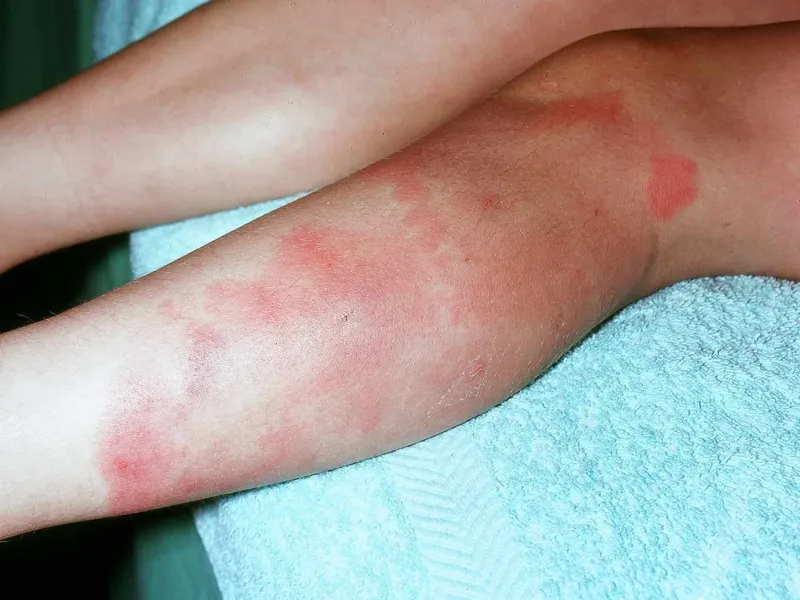
⭐ High-Yield: Treating the underlying IBD often improves peripheral arthritis, but axial (spinal) disease activity is independent of gut inflammation and may require separate targeted therapy.
Diagnosis & Management - Clues & Cures
-
Diagnosis:
- Clinical: Inflammatory back pain (improves with activity), enthesitis, dactylitis, uveitis.
- Labs: HLA-B27 (+), ↑ ESR/CRP. Seronegative (RF & ANA negative).
- Imaging: Sacroiliitis on X-ray or MRI. Advanced ankylosing spondylitis may show "bamboo spine."
-
Management:
⭐ While methotrexate helps peripheral arthritis in psoriatic arthritis, it is not effective for axial (spinal) disease in seronegative spondyloarthropathies. Use TNF-α inhibitors for that.
- Hallmarks include HLA-B27 association, negative RF/ANA, and inflammatory axial arthritis.
- Ankylosing Spondylitis leads to sacroiliitis and spinal fusion (bamboo spine).
- Psoriatic Arthritis is linked to psoriasis, nail pitting, and pencil-in-cup deformities.
- Reactive Arthritis triad: "can't see, can't pee, can't climb a tree" after a GI/GU infection.
- Common features include enthesitis, dactylitis, and uveitis.
- Treatment often involves NSAIDs and TNF-α inhibitors.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

