Pathophysiology - Wear and Tear Blues
- Primarily a degenerative, “wear and tear” process leading to joint failure, distinct from the autoimmune inflammation of rheumatoid arthritis.
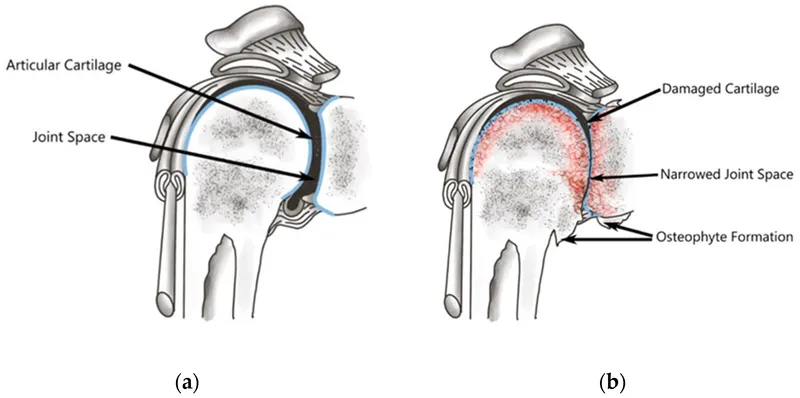
- Articular Cartilage Breakdown:
- Initial injury or stress triggers chondrocyte dysfunction.
- Chondrocytes release degradative enzymes (e.g., metalloproteinases).
- Results in loss of proteoglycans and collagen, causing cartilage to soften, fissure, and erode.
- Subchondral Bone Remodeling:
- Underlying bone thickens (sclerosis).
- Osteophytes (bone spurs) form at the joint margins.
⭐ Unlike inflammatory arthritis, osteoarthritis typically shows normal Erythrocyte Sedimentation Rate (ESR) and C-Reactive Protein (CRP) levels.
Clinical Presentation - Grumpy, Creaky Joints
- Onset: Insidious, typically asymmetrical.
- Pain: Deep, achy; worsens with activity/weight-bearing, improves with rest.
- Stiffness: Morning stiffness is brief (< 30 minutes); may experience gelling (stiffness after inactivity).
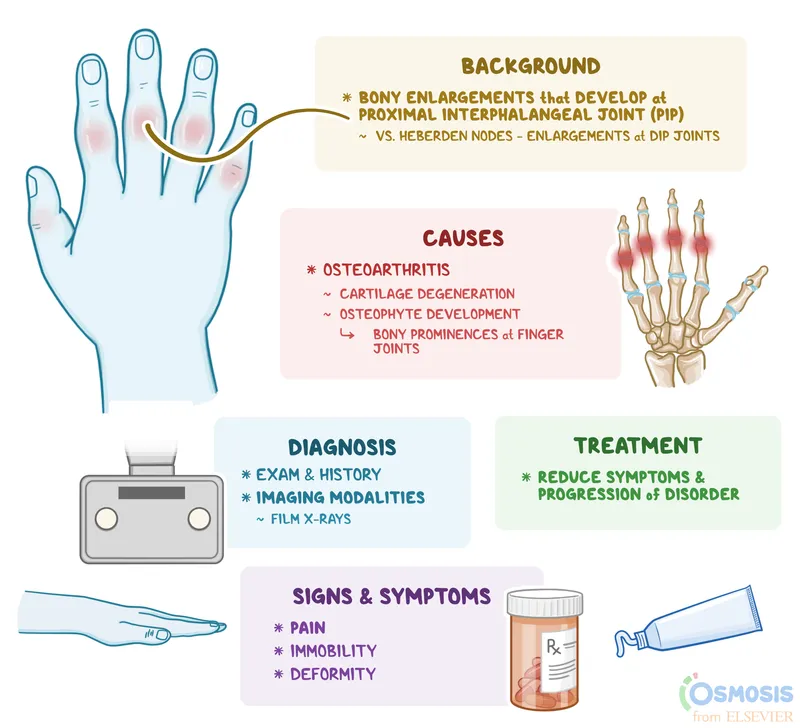
- Exam: Crepitus, limited range of motion, bony enlargements (osteophytes).
- Heberden's nodes: Distal interphalangeal (DIP) joints.
- Bouchard's nodes: Proximal interphalangeal (PIP) joints.
- Systemic: No constitutional symptoms (e.g., fever, fatigue, weight loss).
⭐ The brief duration of morning stiffness (< 30 min) is a key feature distinguishing OA from inflammatory arthritides like Rheumatoid Arthritis (> 60 min).
Diagnosis - The Joint Detective
- Primarily Clinical: Diagnosis is based on age, usage history, and exam findings (e.g., crepitus, bony enlargement). Morning stiffness is typically brief (< 30 minutes).
- Imaging (X-ray):
- 📌 JOSS Mnemonic:
- Joint space narrowing (asymmetric)
- Osteophytes
- Subchondral sclerosis
- Subchondral cysts
- 📌 JOSS Mnemonic:
- Labs: Normal ESR/CRP, negative RF/anti-CCP.
- Arthrocentesis: Non-inflammatory synovial fluid (WBC < 2,000/mm³).
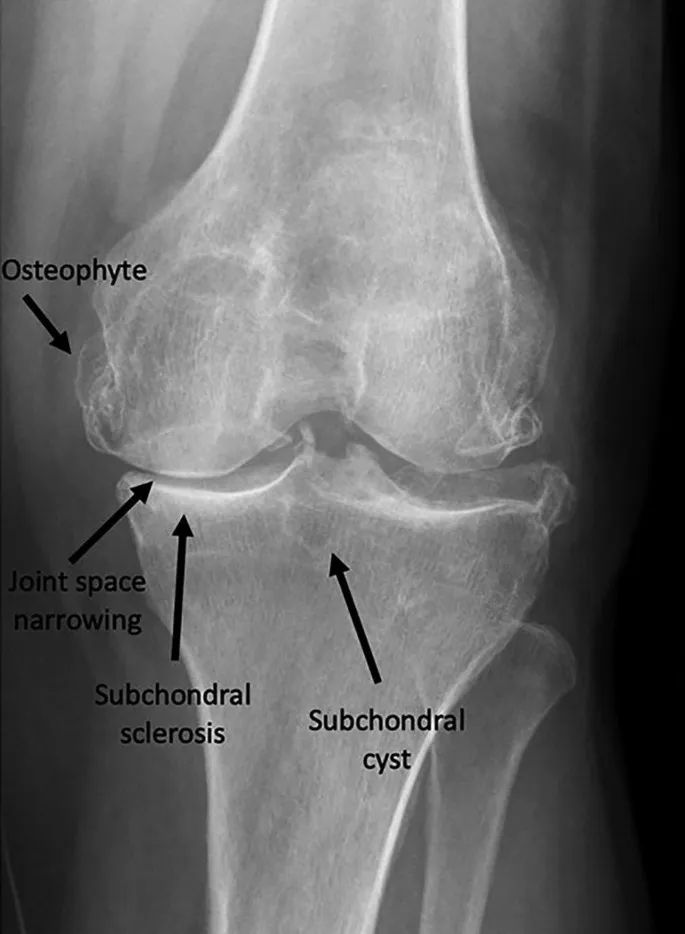
⭐ Exam Favourite: X-ray findings often correlate poorly with patient symptoms; treat the patient, not the X-ray.
Management - Soothing the Squeak
- Goal: Control pain, improve function, and slow joint damage using a stepwise approach, starting with conservative measures.
⭐ Weight loss is the most effective non-pharmacologic intervention for reducing pain and disability in knee OA.
High‑Yield Points - ⚡ Biggest Takeaways
- Degenerative "wear-and-tear" arthritis due to progressive cartilage loss, not an autoimmune process.
- Key symptom: morning stiffness lasting < 30 minutes that worsens with use throughout the day.
- Affects DIP (Heberden's nodes) and PIP (Bouchard's nodes); characteristically spares the MCP joints.
- Classic X-ray findings: asymmetric joint space narrowing, osteophytes, subchondral sclerosis, and cysts.
- Diagnosis is clinical; inflammatory markers (ESR, CRP) and RF are normal.
- Management: weight loss, physical therapy, then acetaminophen and NSAIDs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

