HP Pathophysiology - The Allergic Lung
- Definition: A diffuse, granulomatous interstitial lung disease (ILD) from repeated inhalation of an organic antigen in a sensitized individual.
- Immunologic Mechanism: A combination of hypersensitivity reactions, distinct from asthma.
- Type III (Immune Complex): Antigen-antibody complexes deposit in alveoli, activating complement and causing acute inflammation.
- Type IV (Delayed, Cell-Mediated): T-cell activation leads to the formation of characteristic granulomas upon chronic exposure.
⭐ The presence of poorly formed non-caseating granulomas on biopsy is a classic finding, but not pathognomonic; it's also a key feature of sarcoidosis.
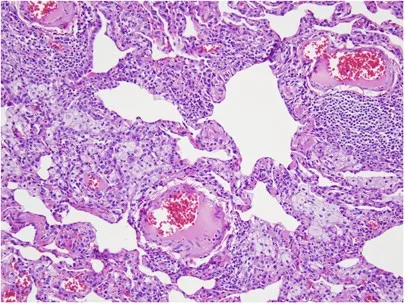
Etiologies & Antigens - Feather & Spore Culprits
Inhaled organic dusts containing antigens are the primary triggers. Diagnosis hinges on identifying the specific exposure. Key syndromes include:
| Syndrome | Antigen Source & Exposure | Antigen(s) |
|---|---|---|
| Farmer's Lung | Moldy hay, grain, compost | Saccharopolyspora rectivirgula |
| Bird Fancier's Lung | Bird droppings & feathers | Avian proteins |
| Hot Tub Lung | Contaminated hot tubs, humidifiers | Mycobacterium avium complex |
| Bagassosis | Moldy sugarcane fiber (bagasse) | Thermophilic actinomycetes |
⭐ Farmer's Lung is the most common type of hypersensitivity pneumonitis.
Clinical Picture & Diagnosis - The Telltale Crackles
- Clinical Presentations Vary:
- Acute: Abrupt onset (4-8 hrs post-exposure) of flu-like symptoms (fever, myalgia), cough, & dyspnea. Resolves with antigen avoidance.
- Subacute: Insidious onset of productive cough & dyspnea over weeks to months.
- Chronic: Progressive dyspnea, cough, and fatigue, leading to irreversible pulmonary fibrosis.
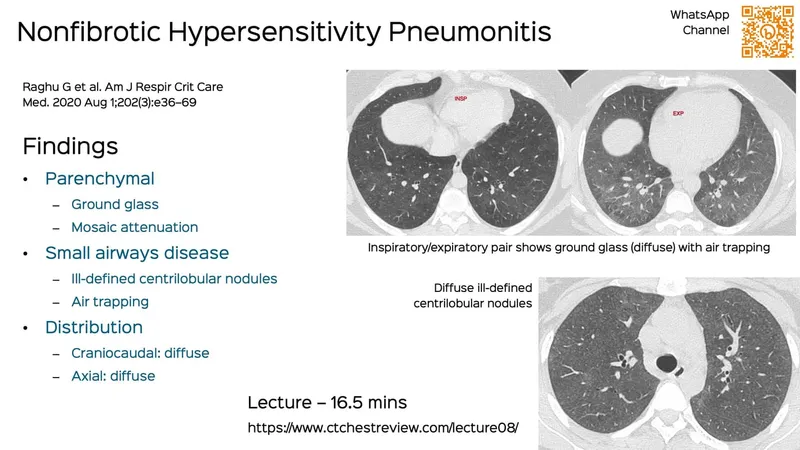
⭐ On high-resolution CT (HRCT), the combination of ground-glass opacities, centrilobular nodules, and air trapping (mosaic attenuation) is highly suggestive of HP.
Management & Prognosis - Dodge, Suppress, Survive
- Antigen Avoidance: The absolute cornerstone of management. Complete removal of the offending agent is paramount for halting disease progression.
- Corticosteroids: Mainstay for symptomatic acute or subacute disease (e.g., prednisone) to suppress inflammation.
- Chronic/Fibrotic HP: May require long-term steroids or other immunosuppressants (e.g., mycophenolate, azathioprine). Lung transplantation is the final option for severe, end-stage fibrotic disease.
- Prognosis: Excellent for acute HP if the antigen is removed; guarded to poor for chronic fibrotic HP.
⭐ The single most important factor determining prognosis in hypersensitivity pneumonitis is the identification and removal of the causative antigen.
- A Type III/IV hypersensitivity reaction to inhaled organic antigens (e.g., moldy hay in Farmer's Lung, avian proteins in Bird Fancier's Lung).
- Acute form presents with sudden fever, cough, and dyspnea 4-8 hours post-exposure.
- Chronic exposure leads to insidious progressive dyspnea and irreversible pulmonary fibrosis.
- Imaging shows diffuse ground-glass opacities (acute) or reticular/nodular patterns with honeycombing (chronic).
- BAL reveals marked lymphocytosis.
- Antigen avoidance is the most critical step in management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

