COPD Pathophysiology - The Inflamed Airway
- Chronic inflammation triggered by noxious particles (tobacco smoke, pollution) recruits key inflammatory cells: neutrophils, macrophages, and CD8+ T-cells.
- This leads to two core pathologic processes:
- Parenchymal Destruction (Emphysema): An imbalance of ↑proteases (like neutrophil elastase) and ↓antiproteases (like α1-antitrypsin) destroys alveolar walls, causing loss of elastic recoil.
- Small Airway Disease: Inflammation and oxidative stress lead to goblet cell hyperplasia (chronic bronchitis) and peribronchiolar fibrosis, which narrows the airway.
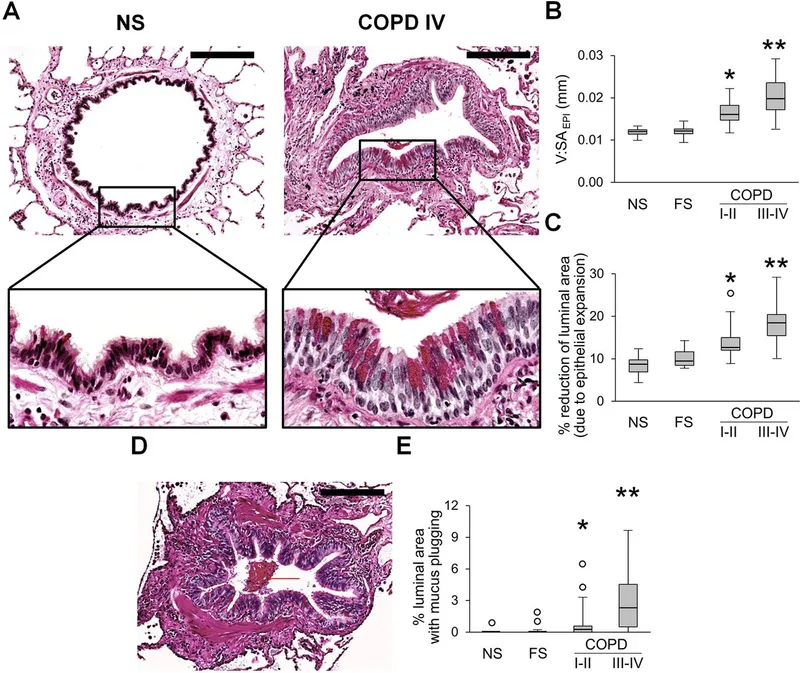
⭐ The primary site of airflow limitation in early COPD is the small conducting airways (<2 mm in diameter), often preceding significant alveolar destruction.
COPD Diagnosis - The Breathless Patient
-
Clinical Suspicion: Based on symptoms (progressive dyspnea, chronic cough, sputum) & risk factor exposure (tobacco smoke, occupational dusts).
- History: >20 pack-year smoking history is a classic risk.
- Exam findings: Barrel chest, pursed-lip breathing, decreased breath sounds.
-
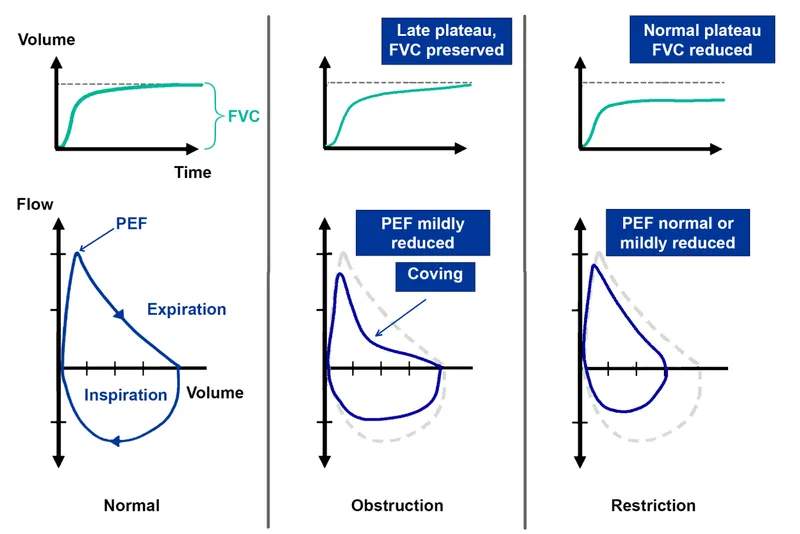
Spirometry: Gold standard for diagnosis. Must be performed post-bronchodilator.
- Diagnostic Hallmark: Fixed airflow obstruction with FEV1/FVC < 0.70.
⭐ In young patients (<45 years) or non-smokers with a family history, screen for Alpha-1 Antitrypsin (AAT) deficiency, which causes basilar-predominant emphysema.
COPD Staging - The GOLD Standard
-
Staging begins after a post-bronchodilator FEV1/FVC < 0.70 confirms diagnosis. Airflow limitation severity (spirometric grade) is based on FEV1:
- GOLD 1 (Mild): FEV1 ≥ 80% predicted
- GOLD 2 (Moderate): 50% ≤ FEV1 < 80%
- GOLD 3 (Severe): 30% ≤ FEV1 < 50%
- GOLD 4 (Very Severe): FEV1 < 30%
-
The refined ABCD assessment tool guides therapy by combining symptom burden (mCAT/CCQ scores) with exacerbation risk.
⭐ Treatment decisions are primarily guided by the patient's ABCD assessment group, not the spirometric grade alone.
High‑Yield Points - ⚡ Biggest Takeaways
- COPD is characterized by persistent, irreversible airflow limitation, with cigarette smoking as the number one risk factor.
- The core pathophysiology involves a protease-antiprotease imbalance, leading to alveolar destruction (emphysema).
- Spirometry is required for diagnosis, confirming a post-bronchodilator FEV1/FVC ratio < 0.7.
- Suspect α1-antitrypsin deficiency in young patients (<45 years) with panacinar emphysema and no smoking history.
- Unlike asthma, the airflow obstruction is not fully reversible with bronchodilators.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

