Nephritic vs. Nephrotic - The Great Divide
- Nephritic (Inflammatory): Glomerular inflammation (immune complex deposition).
- Presents with: Hematuria (RBC casts), HTN, oliguria, azotemia.
- Proteinuria: Mild-to-moderate (< 3.5 g/day).
- Nephrotic (Non-inflammatory): Podocyte damage leading to ↑ permeability.
- Presents with: Massive proteinuria (> 3.5 g/day), hypoalbuminemia, severe edema, hyperlipidemia/lipiduria (oval fat bodies).
- 📌 Mnemonic: PALE (Proteinuria, hypoAlbuminemia, Lipidemia, Edema).
⭐ Nephrotic syndrome causes a hypercoagulable state due to urinary loss of Antithrombin III, increasing risk for thromboembolism.
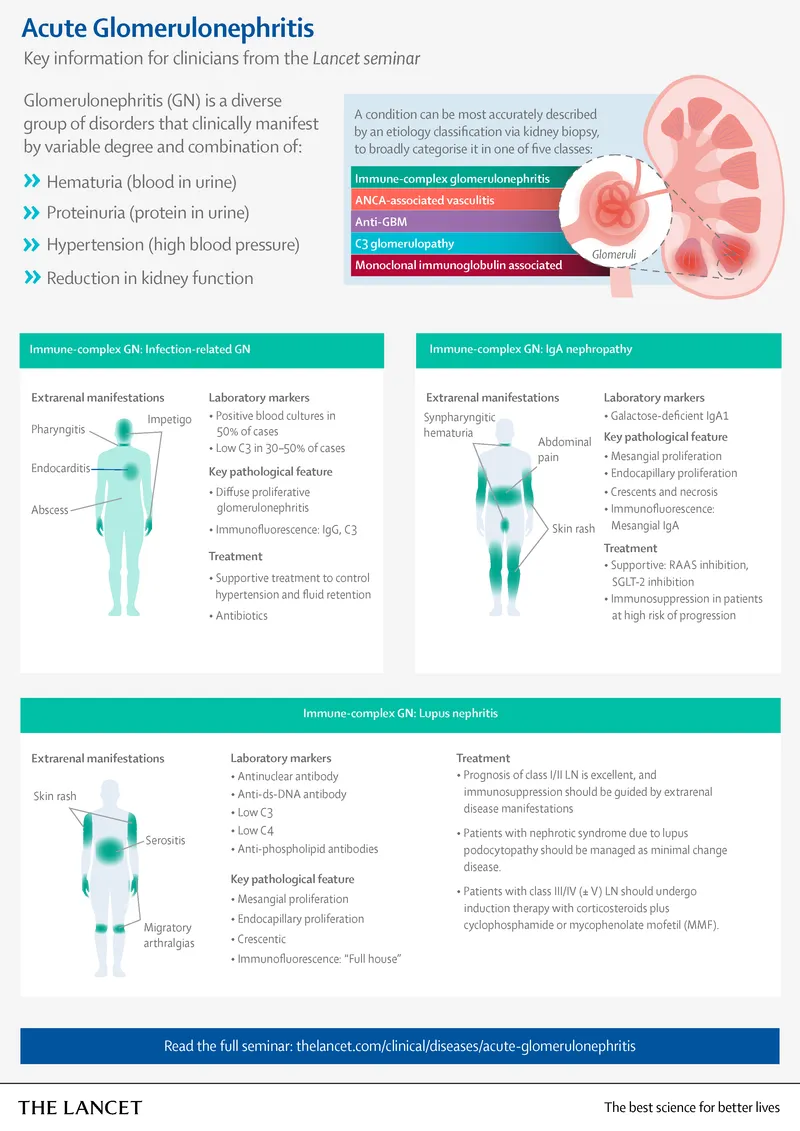
Nephrotic Syndromes - The Protein Leakers
- Hallmarks: Proteinuria >3.5 g/day, hypoalbuminemia, severe edema, hyperlipidemia/lipiduria (oval fat bodies).
- Minimal Change Disease (MCD):
- Most common cause in children; often follows infection.
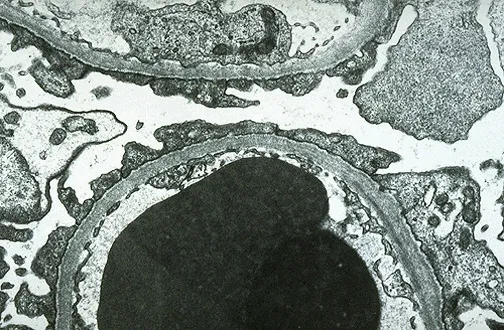
- LM: Normal. EM: Diffuse effacement of podocyte foot processes.
- Excellent, rapid response to corticosteroids.
- Focal Segmental Glomerulosclerosis (FSGS):
- Most common cause in adults (esp. African American).
- Sclerosis in segments of some glomeruli.
- Associations: HIV, heroin use, sickle cell, obesity.
- Membranous Nephropathy (MN):
- Subepithelial immune complex deposits → "spike and dome" on EM.
- Associated with anti-PLA2R Abs, HBV, NSAIDs, malignancy.
⭐ In an adult with new-onset nephrotic syndrome, especially Membranous Nephropathy, always consider and screen for an underlying solid tumor (e.g., lung, colon).
Nephritic Syndromes - The Inflammatory Crew
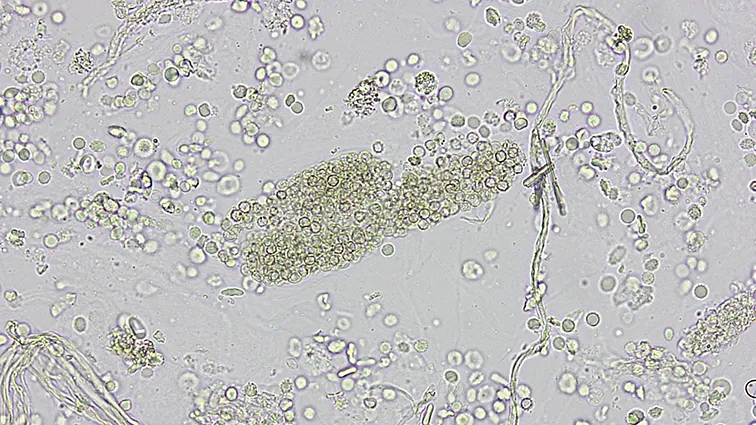
- Hallmark: Glomerular inflammation & bleeding.
- Presentation: Hematuria (cola-colored urine), RBC casts, hypertension, oliguria, and mild proteinuria (< 3.5 g/day).
Classification by Complement (C3) Levels:
-
Normal C3
- IgA Nephropathy (Berger's Disease): Most common cause worldwide. Often follows URI/GI infection.
- Pauci-Immune GN: ANCA-associated (e.g., GPA, MPA).
- Alport Syndrome: Hereditary (Type IV collagen defect); associated with deafness & ocular findings.
-
Low C3
- Post-Streptococcal GN (PSGN): Follows GAS infection (1-3 weeks post-pharyngitis, 3-6 weeks post-impetigo).
- Membranoproliferative GN (MPGN): "Tram-track" appearance on histology.
⭐ Exam Tip: IgA nephropathy presents with hematuria syn-pharyngitically (concurrently with infection), while PSGN has a significant latency period after the infection resolves.
Mixed Pictures - Nephritic-Nephrotic Overlap
- Presents with features of both nephritic (hematuria, HTN) and nephrotic (>3.5 g/day proteinuria, edema) syndromes.
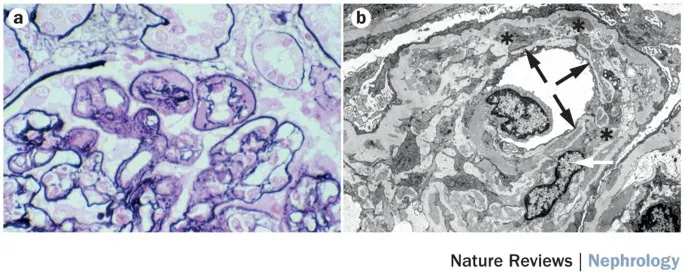
- Membranoproliferative Glomerulonephritis (MPGN): Thickened glomerular basement membrane (GBM) & mesangial proliferation.
- Classic "tram-track" appearance on light microscopy.
- Can be primary or secondary (e.g., HCV, SLE, cryoglobulinemia).
- Diffuse Proliferative Glomerulonephritis (DPGN): Most common & severe lupus nephritis (Class IV).
- Features "wire-loop" lesions from subendothelial deposits.
⭐ MPGN Type I is strongly associated with Hepatitis C virus (HCV), while Type II (Dense Deposit Disease) is linked to C3 nephritic factor, an autoantibody that stabilizes C3 convertase, leading to persistent complement activation and low C3 levels.
- Nephritic syndrome = inflammation (hematuria, HTN). Nephrotic syndrome = podocyte damage (massive proteinuria >3.5 g/day, edema).
- Linear IgG deposits on immunofluorescence are pathognomonic for Goodpasture's syndrome.
- Subepithelial "humps" are classic for Post-streptococcal GN.
- "Spike and dome" appearance on electron microscopy indicates Membranous Nephropathy.
- Crescent formation signifies Rapidly Progressive Glomerulonephritis (RPGN), a nephrologic emergency.
- IgA Nephropathy is the most common primary glomerulonephritis worldwide.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

