CKD Definition & Staging - Know The Score
- Definition: Kidney damage (e.g., albuminuria) OR Glomerular Filtration Rate (GFR) <60 mL/min/1.73m² for >3 months.
- Staging (KDIGO 2012): Classified by cause, GFR category (G-stage), and albuminuria category (A-stage).
| GFR Stage | GFR (mL/min/1.73m²) | Description |
|---|---|---|
| G1 | ≥90 | Normal or high |
| G2 | 60-89 | Mildly decreased |
| G3a | 45-59 | Mildly-moderately ↓ |
| G3b | 30-44 | Moderately-severely ↓ |
| G4 | 15-29 | Severely decreased |
| G5 | <15 | Kidney Failure |
| Albuminuria Stage | ACR (mg/g) | Description |
|---|---|---|
| A1 | <30 | Normal to mildly ↑ |
| A2 | 30-300 | Moderately ↑ |
| A3 | >300 | Severely ↑ |
CKD Etiology - The Usual Suspects
-
Diabetes Mellitus (#1 Cause):
- Hyperglycemia → non-enzymatic glycation of proteins → GBM thickening.
- Leads to diabetic nephropathy.
- Pathognomonic finding: Kimmelstiel-Wilson lesions (nodular glomerulosclerosis).
-
Hypertension (#2 Cause):
- Chronic high pressure damages renal vessels → nephrosclerosis.
- Causes hyaline arteriolosclerosis of small arterioles.
- Leads to glomerulosclerosis and interstitial fibrosis.
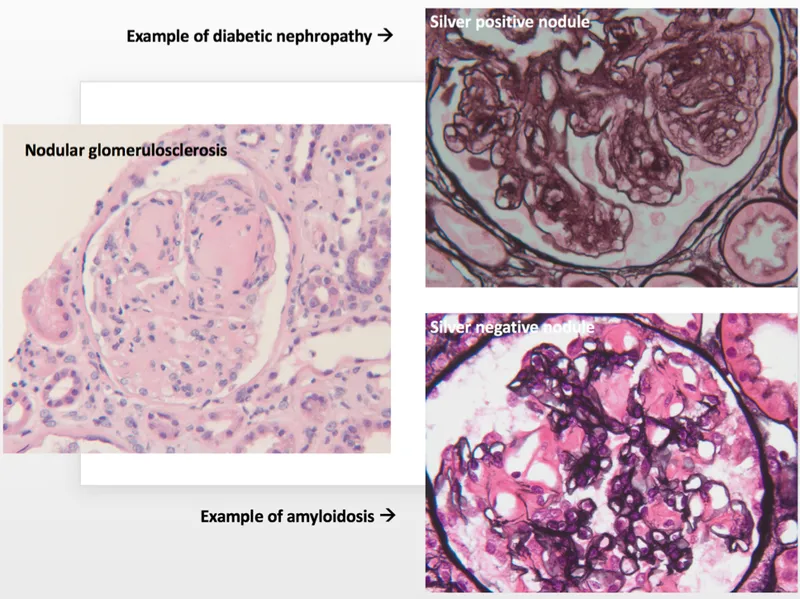
⭐ In diabetic nephropathy, the earliest detectable change is microalbuminuria. Regular screening is crucial for early intervention.
CKD Pathophysiology - The Vicious Cycle
-
Hyperfiltration Hypothesis: The final common pathway in CKD. Initial nephron loss from any cause (e.g., diabetes, HTN) forces remaining nephrons to increase their single-nephron GFR to compensate.
-
The Cycle:
- This sustained hyperfiltration ↑ glomerular capillary pressure and shear stress.
- Causes endothelial and podocyte injury, leading to glomerulosclerosis.
- Results in proteinuria and progressive interstitial fibrosis.
- Ultimately, this destroys more nephrons, perpetuating the cycle.
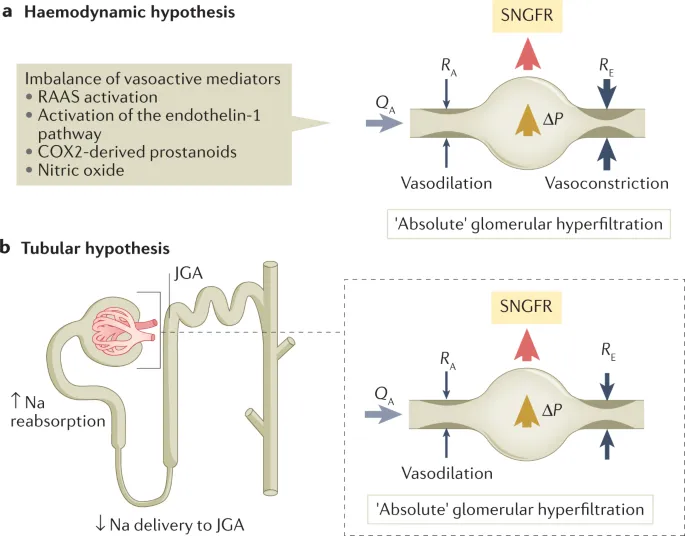
- Key Mediators:
- Angiotensin II: Drives efferent arteriole vasoconstriction (↑ pressure) and stimulates TGF-β.
- TGF-β: Key cytokine promoting fibrosis.
- Proteinuria: Directly toxic to tubular cells, causing inflammation and scarring.
⭐ ACE inhibitors and ARBs slow CKD progression by blocking Angiotensin II, thus dilating the efferent arteriole, which decreases intraglomerular pressure and reduces proteinuria.
Systemic Complications - Uremia's Domino Effect
| Complication | Pathophysiology & Key Features |
|---|---|
| Anemia | Normocytic anemia from ↓ erythropoietin (EPO) production. Iron deficiency may coexist. |
| CKD-Mineral Bone Disorder (MBD) | ↓ active Vit D & ↑PO₄ retention → ↓serum $Ca^{2+}$ → ↑PTH (secondary hyperparathyroidism) & ↑FGF-23. Leads to renal osteodystrophy. |
| Metabolic Acidosis | Impaired excretion of H⁺ and reabsorption of $HCO_3^−$, leading to a high anion gap metabolic acidosis. |
| Uremic Syndrome | Accumulation of waste products. Manifests as encephalopathy (asterixis), uremic pericarditis, and platelet dysfunction (bleeding). |
High‑Yield Points - ⚡ Biggest Takeaways
- Diabetes and hypertension are the leading causes of CKD.
- Pathophysiology involves nephron loss, leading to compensatory hyperfiltration and eventual glomerulosclerosis.
- Persistent albuminuria is a key marker of kidney damage and predicts progression.
- Uremic symptoms manifest late, typically when GFR is <15 mL/min.
- Major complications include anemia (↓ EPO), mineral and bone disorder (secondary hyperparathyroidism), and metabolic acidosis.
- ACE inhibitors/ARBs are crucial for slowing progression, especially with proteinuria.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

