Anemia of CKD - The Pale Kidney
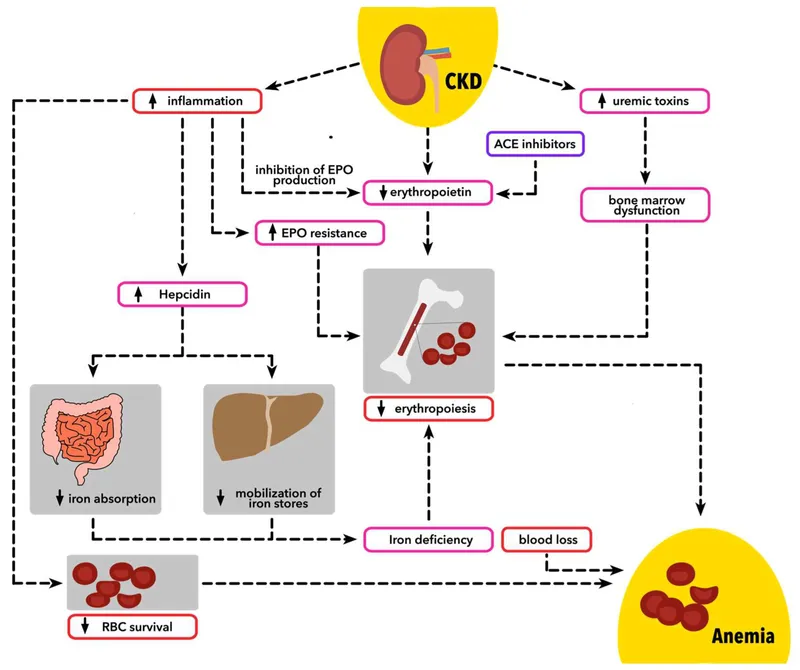
- Pathophysiology: Normocytic, normochromic anemia from ↓ erythropoietin (EPO) production by failing peritubular cells. Uremic toxins also shorten RBC lifespan.
- Diagnosis: Workup initiated when Hemoglobin <10 g/dL. Always rule out iron deficiency first (ferritin, TSAT).
- Management:
- 1. Iron Repletion: If needed. Goal: Ferritin >100 ng/mL, TSAT >20%.
- 2. ESAs: Erythropoiesis-stimulating agents (e.g., epoetin alfa, darbepoetin).
- Hb Target: 10-11.5 g/dL. ⚠️ Avoid normalizing Hb (>13 g/dL) due to ↑ thromboembolic risk.
⭐ The most common side effect of ESA therapy is new-onset or worsening hypertension.
CKD-MBD - Bone & Mineral Mayhem
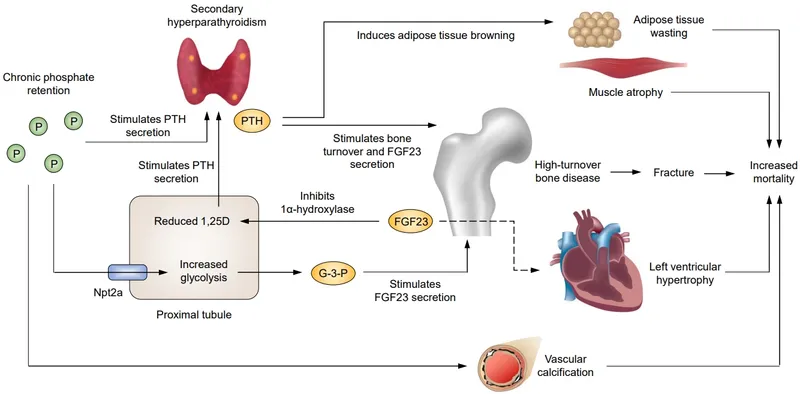
- Pathophysiology: ↓ GFR → ↑ PO₄ & ↓ active Vitamin D → ↓ Ca²⁺ → secondary hyperparathyroidism (↑ PTH).
- Renal Osteodystrophy Spectrum:
- Osteitis Fibrosa Cystica: High-turnover from severe ↑ PTH; bone pain, fractures.
- Adynamic Bone Disease: Low-turnover, often from PTH over-suppression.
- Osteomalacia: Defective mineralization.
- Management:
- Phosphate Binders: Sevelamer, calcium acetate (goal PO₄ < 5.5 mg/dL).
- Vitamin D Analogs: Calcitriol (suppresses PTH).
- Calcimimetics: Cinacalcet (↑ CaSR sensitivity).
⭐ Adynamic bone disease is now the most common renal osteodystrophy, often resulting from iatrogenic oversuppression of PTH during treatment.
Metabolic Acidosis - The pH Plunge
- Pathophysiology: ↓ GFR leads to impaired renal excretion of H+ and ↓ regeneration of bicarbonate ($HCO_3^-$).
- Complications: Worsens bone demineralization (renal osteodystrophy) and muscle catabolism. Can accelerate CKD progression.
- Diagnosis: ↓ Serum $HCO_3^-$ (< 22 mEq/L) and ↓ arterial pH.
- Treatment:
- Goal: Maintain serum $HCO_3^-$ ≥ 22 mEq/L.
- Initiate oral alkali replacement (sodium bicarbonate or citrate) when $HCO_3^-$ < 22 mEq/L.
⭐ Correcting acidosis may slow CKD progression, reduce muscle wasting, and improve bone health.
Hyperkalemia - Potassium's Peril
- EKG Changes: Peaked T waves → flattened P waves → widened QRS → sine wave pattern.
- Management Steps: 📌 C BIG K Drop
- Cardiac Membrane Stabilization: IV Calcium Gluconate (if EKG changes).
- Beta-agonists / Bicarb / Insulin + Glucose: Shift K+ intracellularly.
- Kayexalate (SPS) / Diuretics / Dialysis: Remove K+ from body.
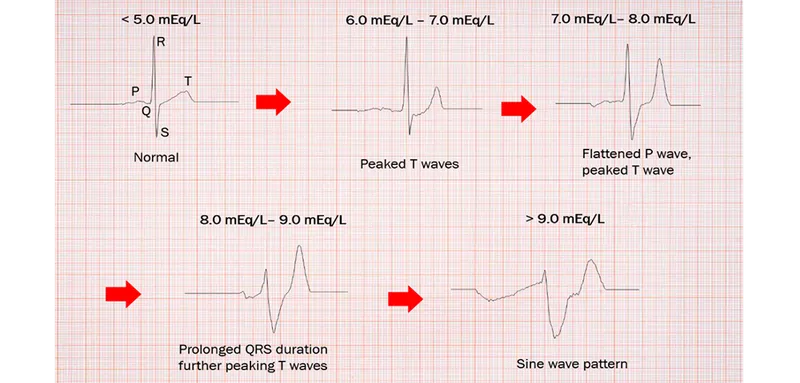
⭐ With EKG changes, the first and most crucial step is IV Calcium Gluconate to stabilize the cardiac membrane, preventing fatal arrhythmias.
HTN & Volume Overload - The Pressure Cooker
CKD impairs sodium and water excretion, leading to volume overload and hypertension. Management is crucial to slow progression.
- Volume Control:
- Dietary sodium restriction: < 2 g/day.
- Loop diuretics (e.g., furosemide) are preferred, especially with GFR < 30 mL/min.
- Blood Pressure Control:
- Target: < 130/80 mmHg.
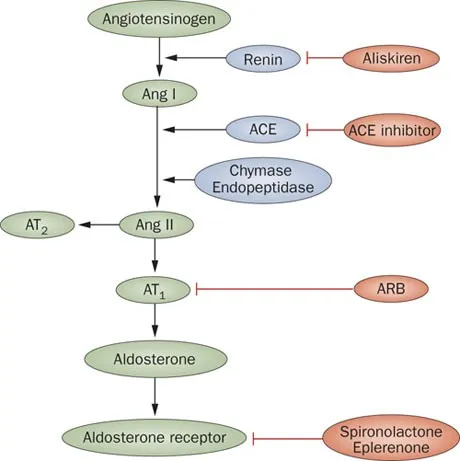
- ACE inhibitors (ACEi) or ARBs are first-line agents, particularly in patients with albuminuria.
⭐ An initial, self-limiting increase in serum creatinine (up to 30%) after starting an ACEi/ARB is acceptable and not a reason to discontinue.
High‑Yield Points - ⚡ Biggest Takeaways
- Anemia of CKD is managed with iron and ESAs; target Hb 10-11.5 g/dL.
- CKD-MBD (↑PO₄, ↓Ca, ↑PTH) requires phosphate binders and vitamin D analogs.
- Treat metabolic acidosis with sodium bicarbonate if serum bicarb is <22 mEq/L.
- Acute hyperkalemia requires calcium gluconate for cardioprotection, then agents to shift K⁺ intracellularly.
- Uremic pericarditis is an absolute indication for immediate hemodialysis.
- Manage fluid overload with loop diuretics and sodium restriction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

