NAFLD Fundamentals - A Fatty Situation
- Definition: Hepatic steatosis (fat accumulation >5% by weight) without secondary causes like significant alcohol consumption.
- Core Pathophysiology: Insulin resistance is the key driver, leading to:
- ↑ Peripheral lipolysis & FFA delivery to the liver.
- ↑ Hepatic de novo lipogenesis.
- ↓ VLDL export.
- Disease Spectrum:
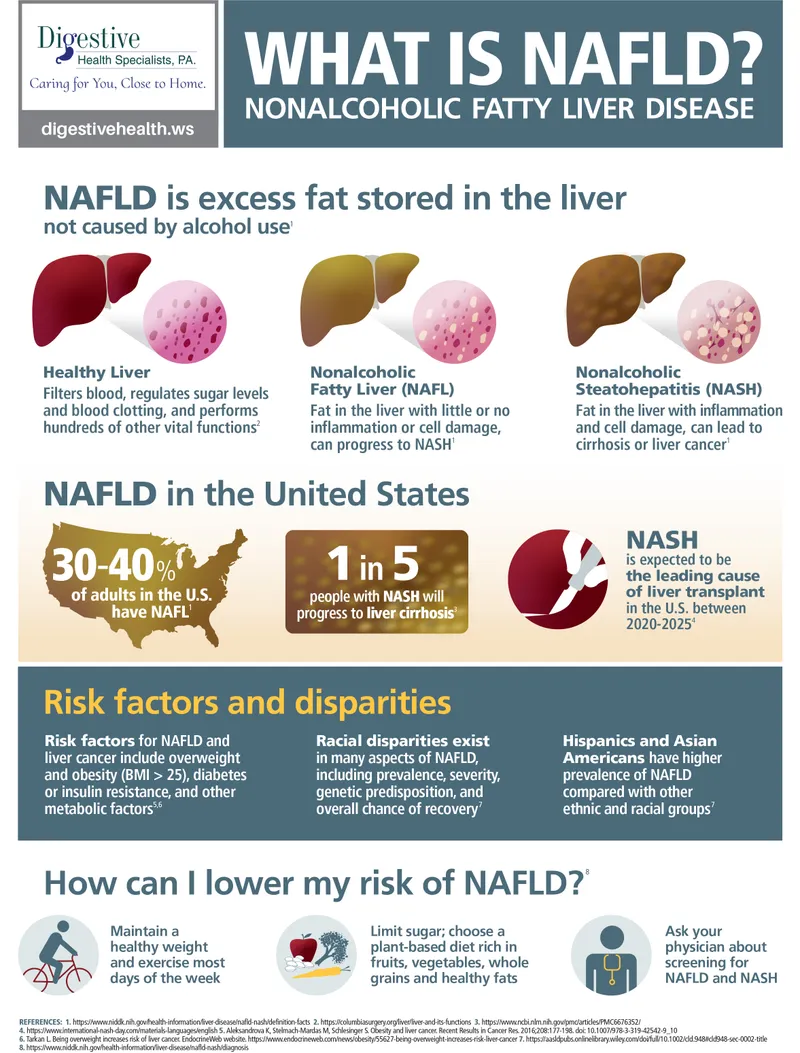
- NAFL (Simple Steatosis): Fat accumulation; generally benign.
- NASH (Nonalcoholic Steatohepatitis): Steatosis + inflammation + hepatocyte injury (e.g., ballooning). Carries risk of fibrosis progression.
- Cirrhosis & HCC: End-stage complications.
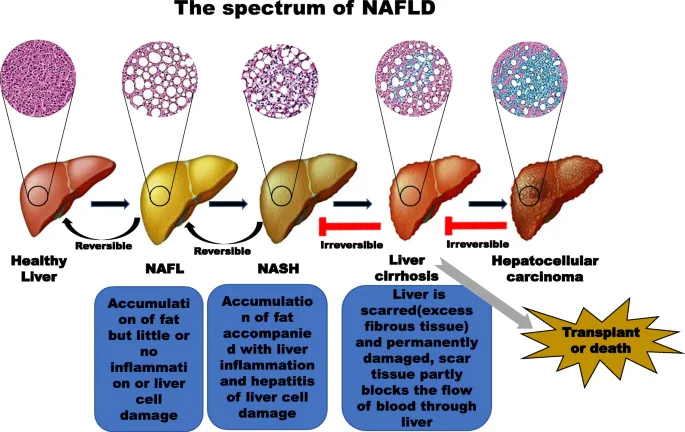
⭐ NAFLD is the hepatic manifestation of metabolic syndrome and the most common chronic liver disease in the United States.
Diagnosis - Catching the Culprit
- Initial Clues: Often asymptomatic; discovered via incidental finding of elevated aminotransferases.
- AST/ALT ratio is typically < 1, distinguishing it from alcoholic liver disease (where the ratio is often > 2).
- Non-Invasive Assessment: First, rule out other liver disease causes (viral, alcohol, autoimmune).
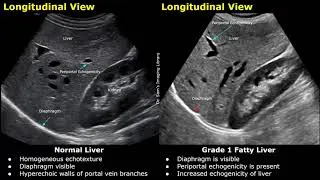
- Imaging: Ultrasound is the primary screening tool, revealing hepatic steatosis (a bright, echogenic liver).
- Fibrosis Scoring: Use tools like the FIB-4 or NAFLD Fibrosis Score to estimate fibrosis risk using patient age, AST, ALT, and platelet count.
- Elastography: Transient elastography (FibroScan) or MRE can quantify liver stiffness to assess fibrosis non-invasively.
- Gold Standard:
- Liver Biopsy: The definitive test to differentiate simple steatosis (NAFL) from NASH (inflammation, ballooning) and to accurately stage fibrosis. Reserved for cases where the diagnosis is uncertain or there's a high risk of advanced fibrosis.
⭐ The diagnosis of NAFLD is fundamentally a diagnosis of exclusion. A thorough workup to rule out other etiologies of chronic liver disease is a critical first step.
Management - The Great Reversal
-
Cornerstone: Lifestyle Modification
- Weight Loss: The most effective intervention. Target >7-10% of body weight to resolve steatosis and inflammation.
- Diet: Mediterranean diet is preferred. Crucially, ↓ intake of high-fructose corn syrup.
- Exercise: 150-200 mins/week of moderate-intensity aerobic activity.
- Control comorbidities: Aggressively manage diabetes, hypertension, and dyslipidemia.
-
Pharmacotherapy (for biopsy-proven NASH & fibrosis ≥ F2)
- Vitamin E (Tocopherol): An antioxidant that improves liver histology.
- Pioglitazone: Insulin sensitizer, improves steatosis and inflammation.
⭐ For patients with co-existing Type 2 Diabetes, Pioglitazone is a key consideration as it addresses both insulin resistance and liver inflammation in NASH.
High‑Yield Points - ⚡ Biggest Takeaways
- NAFLD is a spectrum from simple steatosis to NASH, which can progress to cirrhosis and HCC.
- It's the liver manifestation of metabolic syndrome, driven by insulin resistance.
- Most patients are asymptomatic with incidentally elevated liver enzymes.
- Lab hallmark is an AST/ALT ratio < 1, unlike alcoholic liver disease.
- Liver biopsy is the gold standard to diagnose NASH and stage fibrosis.
- Management cornerstone is weight loss and managing metabolic comorbidities.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

