Pathophysiology & Definitions - The Body's Overreaction
- Sepsis: Life-threatening organ dysfunction due to a dysregulated host response to infection. Essentially, the body's response to an infection damages its own tissues.
- Septic Shock: A subset of sepsis with profound circulatory, cellular, and metabolic abnormalities, associated with a greater risk of mortality.
- Criteria: Persistent hypotension requiring vasopressors to maintain MAP ≥65 mmHg AND serum lactate >2 mmol/L despite adequate fluid resuscitation.
⭐ Even in patients who are not hypotensive, a serum lactate level >2 mmol/L suggests occult hypoperfusion (cryptic shock) and is a key diagnostic and prognostic marker.
Diagnosis & Workup - Spotting the Signs
- Initial Assessment: Secure Airway, Breathing, Circulation (ABCs).
- Bedside Screening (qSOFA): For non-ICU patients with suspected infection. Score ≥ 2 suggests organ dysfunction.
- Respiratory Rate ≥ 22/min
- Altered Mental Status (GCS < 15)
- Systolic BP ≤ 100 mmHg
- Sepsis Diagnosis: Confirmed by suspected infection + an acute SOFA score increase of ≥ 2 points.
- Septic Shock: Sepsis with persistent hypotension requiring vasopressors to maintain MAP ≥ 65 mmHg AND serum lactate > 2 mmol/L despite adequate fluid resuscitation.
- Core Workup:
- Labs: Lactate, CBC, CMP, coags, CRP, procalcitonin.
- Cultures: Two sets (aerobic/anaerobic) from separate sites before antibiotics.
⭐ Obtain blood cultures before starting antibiotics, but never delay antimicrobial therapy if sample collection is prolonged.
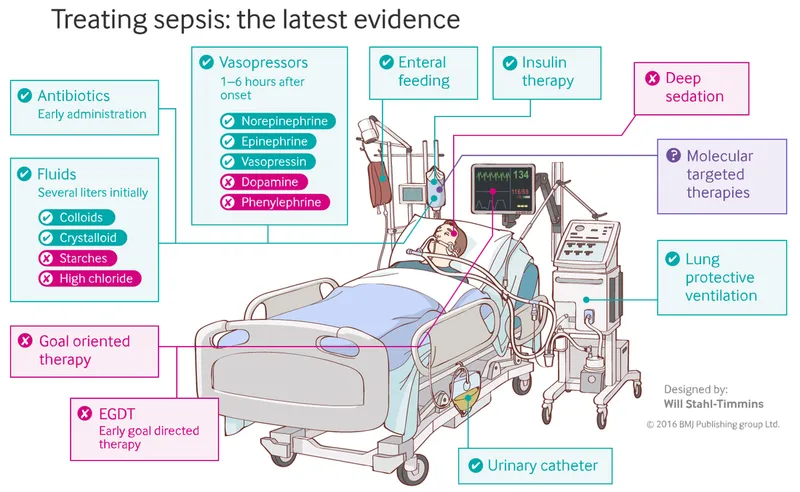
Management - Hour-1 Protocol
- "Surviving Sepsis Campaign: Hour-1 Bundle" - immediate, life-saving interventions.
- Measure lactate level: Remeasure if initial lactate is > 2 mmol/L.
- Obtain blood cultures: Crucial before administering antibiotics.
- Administer broad-spectrum antibiotics: Within the first hour of recognition.
- Rapid fluid resuscitation: Administer 30 mL/kg IV crystalloid for hypotension or lactate ≥ 4 mmol/L.
- Apply vasopressors: If hypotension persists during or after fluids, to maintain Mean Arterial Pressure (MAP) ≥ 65 mmHg.
- Target MAP: $MAP \approx (2 \times DBP + SBP) / 3$
⭐ Exam Favorite: For every hour delay in administering antibiotics in septic shock, mortality increases by approximately 7.6%. Early source control and antibiotics are paramount.
High‑Yield Points - ⚡ Biggest Takeaways
- Sepsis is life-threatening organ dysfunction (↑ SOFA ≥2) from a dysregulated host response to infection. Use qSOFA (AMS, RR ≥22, SBP ≤100) for rapid screening.
- Septic shock is sepsis with persistent hypotension requiring vasopressors to maintain MAP ≥65 mmHg and a serum lactate >2 mmol/L despite adequate fluid resuscitation.
- Key interventions include broad-spectrum antibiotics within 1 hour and 30 mL/kg IV crystalloid for hypotension.
- Norepinephrine is the first-line vasopressor.
- Obtain blood cultures before antibiotics and aggressively pursue source control.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

