Intra-abdominal Infections - Guts Under Siege
- Etiology: Peritonitis (inflammation of peritoneum) or Abscess (walled-off infection). Often polymicrobial from gut flora leakage (e.g., perforation, diverticulitis).
- Pathogens: Gram-negatives (E. coli, Klebsiella) & anaerobes (Bacteroides fragilis).
- Presentation: Fever, tachycardia, severe abdominal pain with guarding or rebound tenderness.
- Diagnosis: CT Abdomen/Pelvis with IV contrast is the gold standard to identify abscesses, free air, or inflammation.
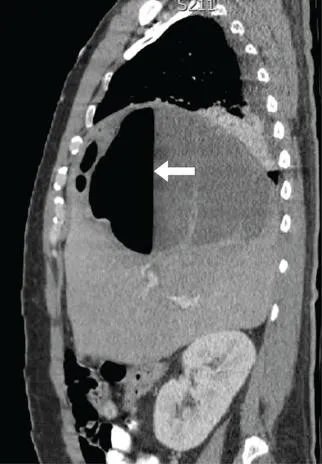
⭐ Source control is paramount! Antibiotics alone are insufficient for abscesses or significant perforations. Management requires prompt surgical intervention or percutaneous drainage.
Diagnosis & Workup - Bellyache Breakdown
- Initial Assessment: History (acute onset, fever, focal pain) & physical exam (guarding, rebound tenderness).
- Labs:
- CBC (leukocytosis with left shift), CMP.
- ↑ Lactate, ↑ CRP, ↑ Procalcitonin.
- Blood cultures x2 (before antibiotics).
- Amylase/Lipase for pancreatitis.
- Imaging: Modality depends on suspected source.
⭐ SBP Diagnosis: For ascites, perform paracentesis. A peritoneal fluid absolute neutrophil count (ANC) of >250 cells/mm³ is diagnostic for Spontaneous Bacterial Peritonitis.
Management Principles - Drain & Tame
Core tenets: 1) Resuscitate, 2) Drain (Source Control), 3) Tame (Antibiotics).
-
Source Control: Crucial first step. Remove infected/necrotic tissue & drain abscesses.
- Percutaneous catheter drainage (PCD) for simple abscesses.
- Surgical exploration (laparotomy/laparoscopy) for complex collections or diffuse peritonitis.
-
Antibiotics: Broad-spectrum empiric therapy, then tailor to culture results.
- Community-Acquired: Cover GNRs & anaerobes (e.g., Ceftriaxone + Metronidazole; Piperacillin-Tazobactam).
- Hospital-Acquired: Broader coverage needed (e.g., Carbapenems).
⭐ Failure to improve in 48-72h despite antibiotics suggests inadequate source control or resistant organisms.
Common Culprits - A Rogues' Gallery
The usual suspects are gut-derived gram-negative aerobes and anaerobes. Think polymicrobial, especially after perforation.
| Site of Infection | Common Pathogens | Key Feature |
|---|---|---|
| Biliary Tract | E. coli, Klebsiella, Enterococcus | Ascending infection |
| Liver Abscess | K. pneumoniae, E. coli, Bacteroides | Single or multiple |
| SBP | Monomicrobial: E. coli, Klebsiella | In cirrhosis/ascites |
| Secondary Peritonitis | Polymicrobial: E. coli, B. fragilis | Gut perforation |
High‑Yield Points - ⚡ Biggest Takeaways
- Spontaneous Bacterial Peritonitis (SBP) in cirrhosis requires paracentesis showing PMN > 250 cells/mm³; treat with third-gen cephalosporins.
- Secondary peritonitis from a perforated viscus is a surgical emergency requiring broad-spectrum antibiotics.
- Diverticulitis classically causes LLQ pain; CT scan is the best diagnostic test.
- Appendicitis presents with migratory RLQ pain and requires appendectomy.
- Acute cholecystitis and cholangitis cause RUQ pain; ultrasound is the initial imaging of choice.
- Liver abscesses require drainage and targeted antibiotics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

