Platelet Basics - The Sticky Situation
- Genesis & Lifespan: From bone marrow megakaryocytes. Lifespan 8-10 days. Normal count: 150,000-450,000/μL.
- Primary Hemostasis Steps:
- Adhesion: von Willebrand Factor (vWF) links subendothelial collagen to the platelet GpIb receptor.
- Activation: Shape change; release of ADP & TXA2 recruits more platelets.
- Aggregation: Fibrinogen cross-links platelets via GpIIb/IIIa receptors, forming the plug.
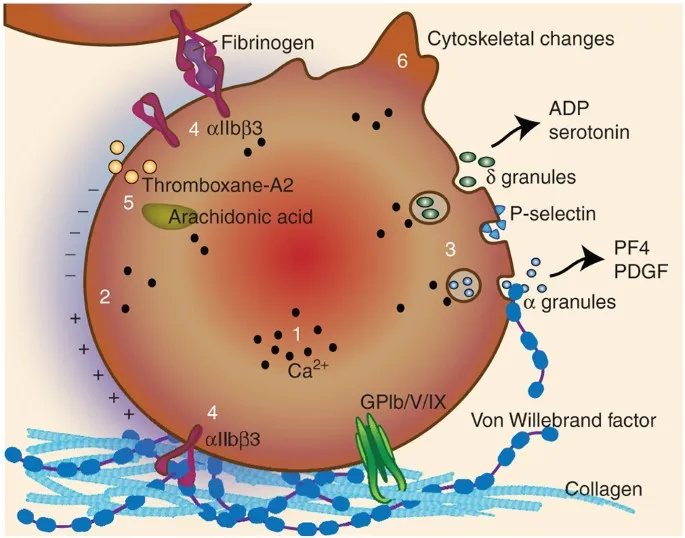
⭐ Bernard-Soulier syndrome (impaired GpIb) causes defective adhesion. Glanzmann thrombasthenia (impaired GpIIb/IIIa) causes defective aggregation.
Thrombocytopenia - The Great Platelet Drop
- Definition: Platelet count < 150,000/μL. Bleeding risk ↑ significantly when < 20,000/μL.
- Etiology Buckets:
- ↓ Production: Marrow failure (aplastic anemia, MDS), chemo, radiation, alcohol, viral (HIV, HCV).
- ↑ Destruction:
- Immune: ITP, HIT, SLE, drug-induced.
- Non-immune (MAHA): TTP, HUS, DIC, HELLP. Schistocytes on smear are key!
- Sequestration: Splenomegaly (e.g., from cirrhosis).
- Dilutional: Massive transfusions.
⭐ Spontaneous bleeding is uncommon unless the platelet count drops below 10,000-20,000/μL. Petechiae and ecchymoses are classic signs.
MAHAs - Shreds, Clots & Trouble
- Pathophysiology: Microvascular endothelial damage leads to platelet-rich thrombi, shearing RBCs into schistocytes ("helmet cells"), causing intravascular hemolysis.
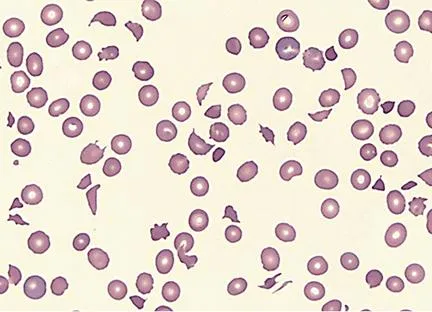
- Core Syndromes:
- TTP (Thrombotic Thrombocytopenic Purpura): ↓ADAMTS13 activity. Causes large vWF multimers → platelet trapping. Neurologic symptoms are prominent.
- HUS (Hemolytic Uremic Syndrome): Often follows E. coli O157:H7 infection (Shiga toxin). Predominantly acute kidney injury.
- DIC (Disseminated Intravascular Coagulation): Widespread clotting & fibrinolysis. ↑PT/PTT, ↑D-dimer, ↓Fibrinogen.
⭐ The classic TTP pentad (fever, anemia, thrombocytopenia, renal & neuro findings) is rare. Suspect TTP with unexplained MAHA and thrombocytopenia alone.
Qualitative Disorders - Flawed & Useless Platelets
- Presentation: Normal platelet count, but ↑ Bleeding Time. Patients present with mucocutaneous bleeding (epistaxis, gingival bleeding, petechiae).
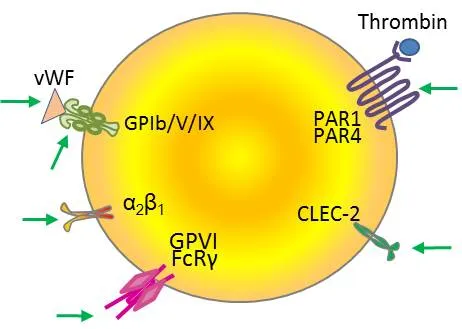
| Disorder | Defect | Platelet Size | Key Lab Finding |
|---|---|---|---|
| Bernard-Soulier | ↓ GpIb | Large (Big) | No aggregation with Ristocetin |
| Glanzmann | ↓ GpIIb/IIIa | Normal | No aggregation with ADP, Epi, Collagen |
| Aspirin/NSAIDs | Acquired | Normal | Impaired thromboxane A2 synthesis |
| Uremia | Acquired | Normal | Impaired adhesion & aggregation |
📌 Mnemonic: Bernard-Soulier has Big Suckers (large platelets).
High‑Yield Points - ⚡ Biggest Takeaways
- Immune Thrombocytopenia (ITP) presents with isolated thrombocytopenia from anti-GpIIb/IIIa antibodies.
- Thrombotic Thrombocytopenic Purpura (TTP) results from ADAMTS13 deficiency, causing the classic FAT-RN pentad.
- Hemolytic Uremic Syndrome (HUS) is a triad of MAHA, thrombocytopenia, and AKI, often post-E. coli O157:H7.
- von Willebrand Disease, the most common inherited type, causes impaired platelet adhesion.
- DIC consumes clotting factors, causing ↑ PT/PTT/D-dimer with ↓ fibrinogen and platelets.
- Bernard-Soulier (GpIb defect) impairs adhesion; Glanzmann's (GpIIb/IIIa defect) impairs aggregation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

