VHD & HF - Valves Under Pressure
- Valvular lesions cause HF via two main pathways based on the type of hemodynamic stress:
- Stenosis: A pressure-loaded ventricle (↑ afterload) undergoes concentric hypertrophy (thickened walls, smaller cavity), leading to impaired relaxation and diastolic HF (HFpEF).
- Regurgitation: A volume-loaded ventricle (↑ preload) undergoes eccentric hypertrophy (dilated cavity), leading to eventual pump failure and systolic HF (HFrEF).
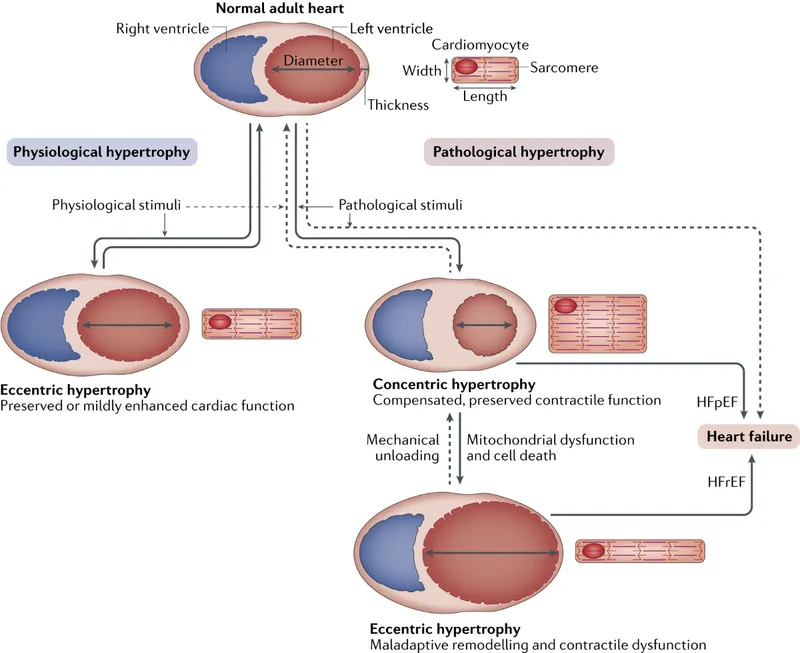
⭐ Acute, severe regurgitation (e.g., post-MI papillary muscle rupture) bypasses chronic remodeling, causing rapid cardiogenic shock.
Aortic Stenosis - The Stubborn Door
- Etiology: Age-related (senile) calcification or congenital bicuspid aortic valve.
- Pathophysiology: LV outflow obstruction → pressure overload → concentric LV hypertrophy → diastolic, then systolic dysfunction.
- Clinical Triad (📌 SAD): Syncope, Angina, Dyspnea are late, ominous signs.
- Murmur: Harsh crescendo-decrescendo systolic murmur radiating to carotids. Pulsus parvus et tardus (weak, delayed pulse).
- Severity: Valve area <1.0 cm² is severe.
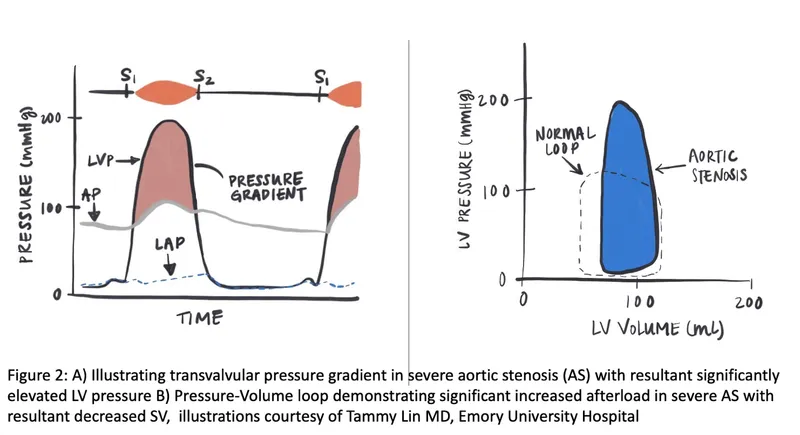
⭐ The onset of symptoms is a critical prognostic marker. Without valve replacement, average survival is grim: 2 years with syncope, 3 with angina, 5 with dyspnea.
Aortic Regurgitation - The Leaky Gate
- Etiology: Aortic root dilation (Marfan syndrome, syphilis), infective endocarditis, rheumatic fever.
- Pathophysiology: Backward flow into LV → LV volume overload → eccentric hypertrophy → ↑ stroke volume but eventual systolic dysfunction.
- Symptoms & Signs: Palpitations, dyspnea. ↑ Systolic & ↓ diastolic pressure → wide pulse pressure.
- Eponyms: Water-hammer pulse (Corrigan's), de Musset's sign (head bobbing), Quincke's pulses (capillary pulsations).
- Murmur: High-pitched, blowing, early diastolic decrescendo murmur best heard at the left sternal border.
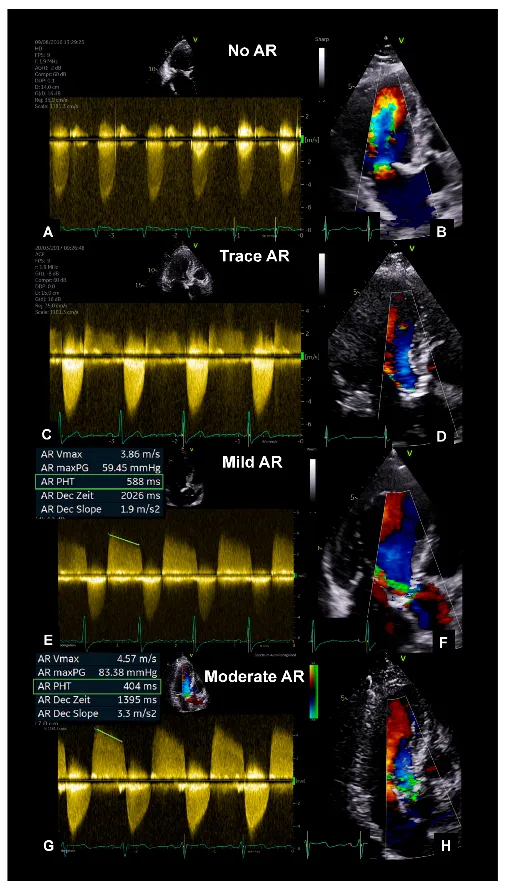
⭐ Exam Favorite: An Austin Flint murmur, a mid-diastolic rumble, can be heard. It's caused by the regurgitant jet striking the anterior mitral valve leaflet, mimicking mitral stenosis.
Mitral Stenosis - The Atrial Jam
- Etiology: Almost exclusively rheumatic heart disease.
- Pathophysiology: Obstruction at the mitral valve → ↑ LA pressure → LA enlargement → pulmonary hypertension → right-sided HF.
- Clinical Features:
- Murmur: Opening snap (OS) followed by a low-pitched mid-diastolic rumble, best heard at the apex.
- Complications: Atrial fibrillation (from LA stretch), hoarseness (Ortner's syndrome), dysphagia.
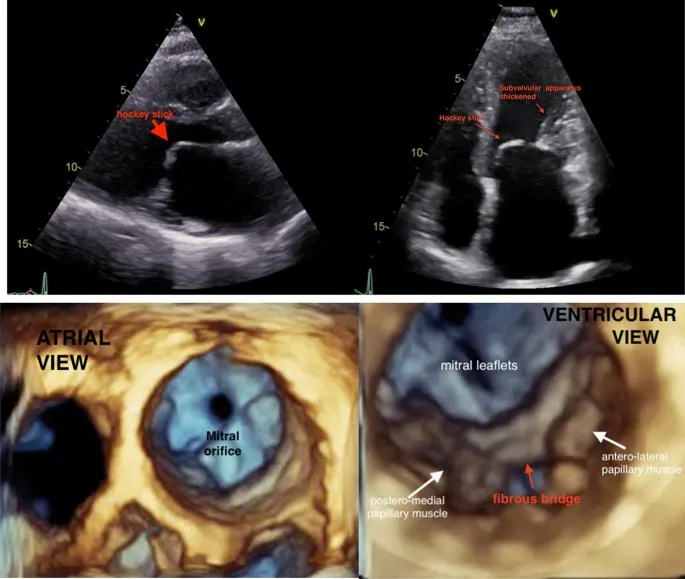
⭐ The interval between S2 and the opening snap is inversely proportional to the severity of the stenosis; a shorter S2-OS interval means more severe MS.
Mitral Regurgitation - The Backflow Problem
- Etiology: Most commonly from mitral valve prolapse; also ischemic damage to papillary muscles (post-MI), infective endocarditis, or rheumatic heart disease.
- Pathophysiology: Backflow into the left atrium (LA) causes volume overload in both the LA and left ventricle (LV).
- Leads to LA enlargement (↑ risk of atrial fibrillation) and eccentric LV hypertrophy.
- Eventually results in systolic dysfunction with a decreased ejection fraction.
- Murmur: Holosystolic, blowing murmur best heard at the apex, radiating to the axilla.
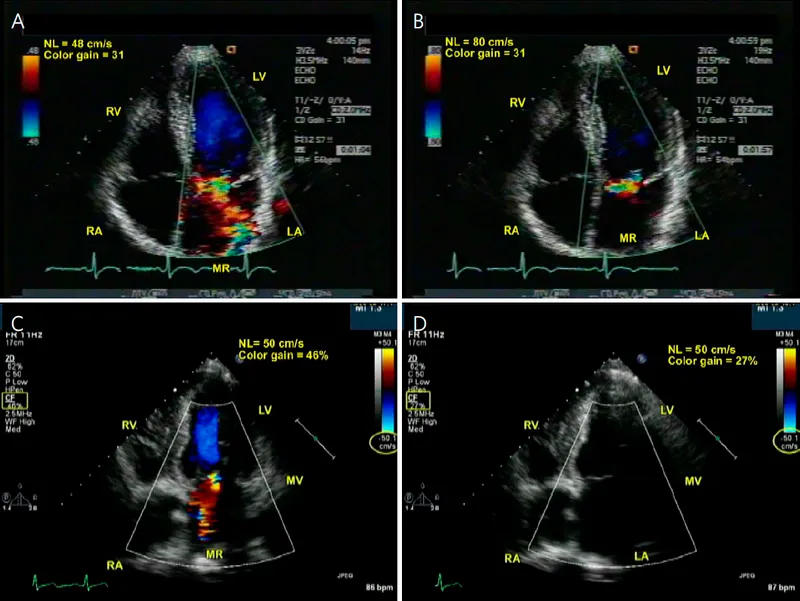
⭐ The intensity of the MR murmur does not correlate with its severity. A soft murmur can be severe, especially in acute MR where LA pressures are very high.
High‑Yield Points - ⚡ Biggest Takeaways
- Aortic stenosis is the most common valvular cause of HF; presents with syncope, angina, and dyspnea (SAD).
- Acute regurgitation (aortic/mitral) is a surgical emergency causing pulmonary edema and cardiogenic shock.
- Mitral regurgitation has a holosystolic murmur radiating to the axilla.
- Mitral stenosis (from rheumatic fever) leads to atrial fibrillation and right-sided HF.
- Aortic regurgitation causes a diastolic murmur and wide pulse pressure.
- Left-sided valve disease drives pulmonary hypertension and subsequent right-sided HF.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

