Etiology & Pathophysiology - The Pressure Backlog
- Most Common Cause: Left heart failure (LHF). Pressure backs up from the failing LV into the pulmonary circulation, increasing RV afterload.
- Other Causes (leading to Cor Pulmonale):
- Chronic lung disease (COPD, ILD)
- Idiopathic pulmonary arterial hypertension
- Recurrent pulmonary emboli
- Right-sided valvular disease (e.g., tricuspid regurgitation, pulmonic stenosis)
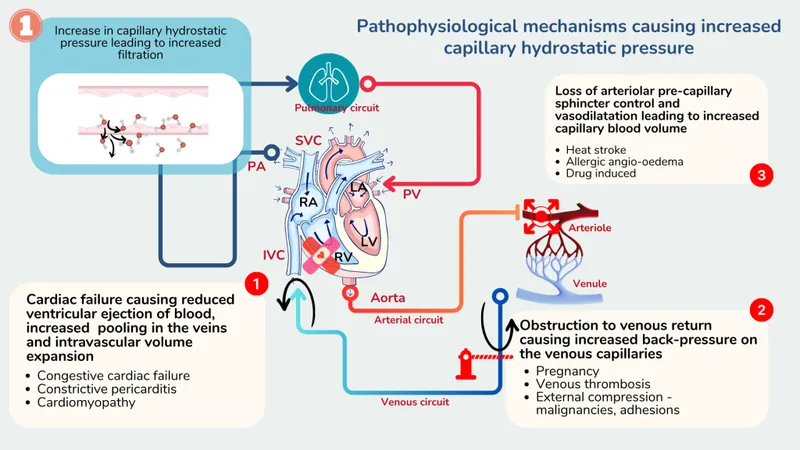
⭐ Cor pulmonale is right heart failure arising from a primary disorder of the respiratory system, creating pulmonary hypertension. RHF due to LHF or congenital heart disease is not cor pulmonale.
Clinical Presentation - Systemic Swamp
Failure of the right ventricle causes a backup of blood in the systemic venous circuit, leading to fluid overload.
- Jugular Venous Distension (JVD): Hallmark of ↑ CVP.
- JVP >8 cm H₂O.
- Positive hepatojugular reflux (HJR).
- Dependent Pitting Edema:
- Ankles and presacral area.
- Can progress to anasarca.
- Congestive Hepatopathy:
- Tender hepatomegaly (RUQ pain).
- Pulsatile liver.
- Chronic congestion → "cardiac cirrhosis."
- GI Tract Congestion:
- Ascites.
- Anorexia, nausea, early satiety.
⭐ Kussmaul's Sign: A paradoxical rise in JVP on inspiration, indicating limited RV filling. Seen in severe RHF and constrictive pericarditis.
📌 Mnemonic (AW HEAD): Anorexia, Weight gain, Hepatomegaly, Edema, Ascites, Distended neck vein.

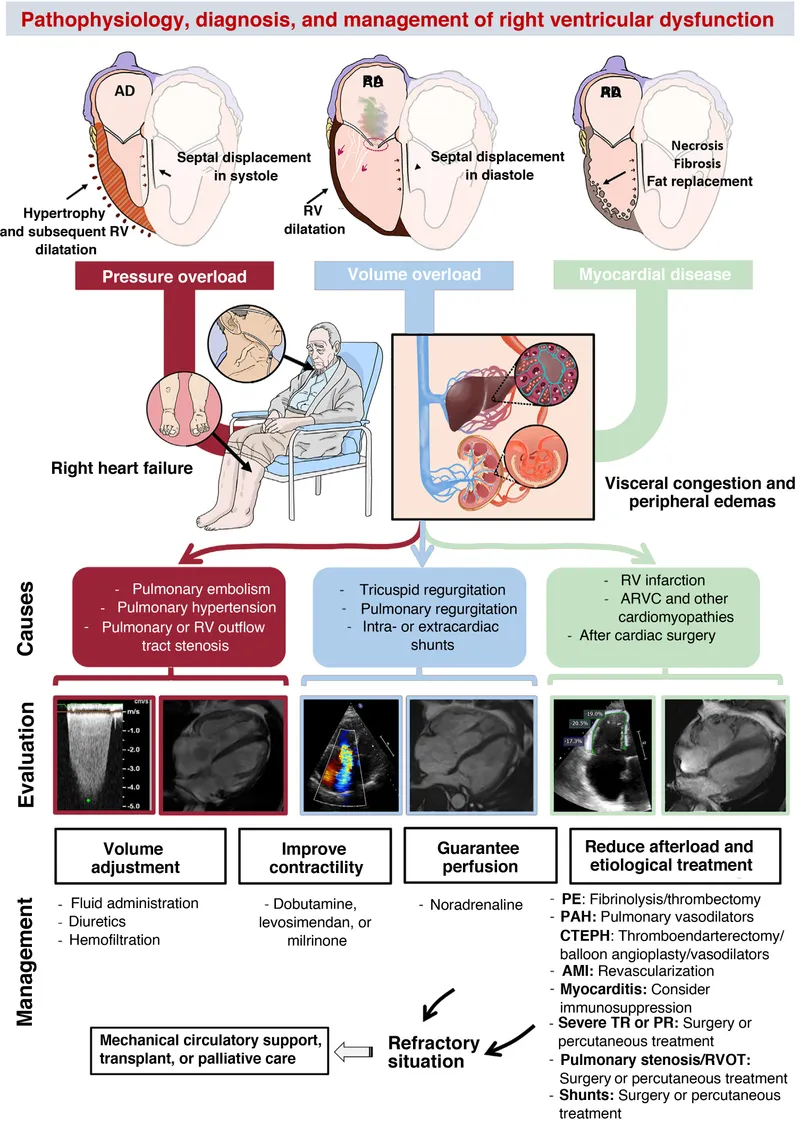
Diagnosis - The Right-Sided Reveal
- Physical Exam: Key findings include:
- Jugular Venous Distension (JVD)
- Positive Hepatojugular Reflux (HJR)
- Symmetrical peripheral pitting edema
- Tender hepatomegaly & ascites
- Echocardiogram (Best Initial Test):
- Shows RV dilation & hypokinesis.
- Estimates RV systolic pressure (RVSP) & pulmonary artery pressure.
- Assesses for tricuspid regurgitation.
- Right Heart Catheterization (Gold Standard):
- Confirms diagnosis and quantifies severity.
- Measures: ↑ CVP, ↑ PVR, normal/low PCWP.
⭐ Kussmaul's Sign: A paradoxical rise in JVP during inspiration is highly specific for impaired RV filling, seen in severe RHF or constrictive pericarditis.
Management - Diuresis & Decongestion
- Primary Goal: Relieve congestive symptoms (peripheral edema, ascites, JVD) by reducing central venous pressure through fluid removal.
- First-line Therapy: IV Loop Diuretics for acute decompensation (e.g., Furosemide, Bumetanide).
- IV route preferred due to poor oral bioavailability from gut edema.
- Monitor: Daily weights, strict I/Os, electrolytes (K⁺, Mg²⁺), and renal function (BUN, Cr).
- Strategy for Diuretic Resistance:
⭐ For diuretic resistance, administer a thiazide (e.g., metolazone) 30 minutes before a loop diuretic. This timing maximizes sequential nephron blockade, preventing distal tubule hypertrophy from compensating for the loop's effect.
- Ultrafiltration: A mechanical fluid removal option for patients with severe, refractory volume overload, especially with worsening renal function (cardiorenal syndrome).
High‑Yield Points - ⚡ Biggest Takeaways
- The most common cause of right heart failure (RHF) is left-sided heart failure.
- Isolated RHF is most frequently caused by cor pulmonale, often secondary to COPD.
- Clinical manifestations are dominated by systemic venous congestion, not pulmonary symptoms.
- Key signs include jugular venous distension (JVD), pitting lower extremity edema, and congestive hepatosplenomegaly.
- Kussmaul's sign (a paradoxical rise in JVP on inspiration) is a characteristic finding.
- Echocardiography is the best initial test; right heart catheterization is the gold standard for diagnosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

