Advanced HF Staging - The Downward Spiral
Describes patients with refractory Stage D heart failure, often considered for Mechanical Circulatory Support (MCS) or transplant. The INTERMACS (Interagency Registry for Mechanically Assisted Circulatory Support) profiles categorize patients based on clinical severity, guiding therapy timing.
⭐ Patients in INTERMACS profiles 1-3 have the highest urgency and mortality risk, often necessitating immediate intervention with temporary or durable MCS as a bridge to transplant or as destination therapy.
Bridge to Transplant - Mechanical Life Support
Mechanical Circulatory Support (MCS) is used for refractory heart failure, stabilizing patients awaiting transplant.
-
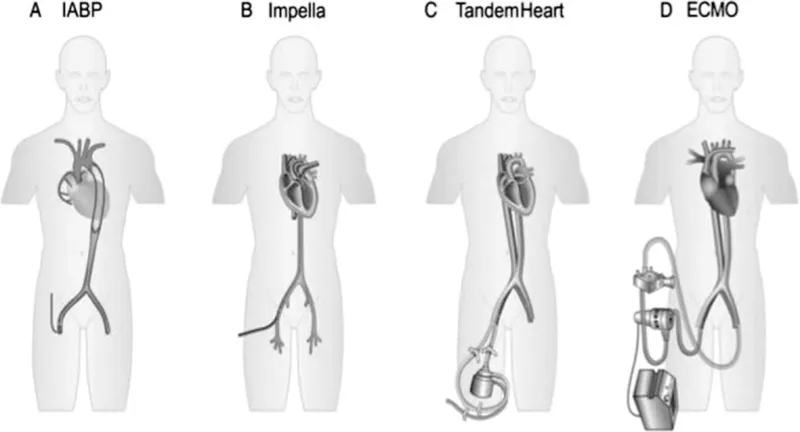
Intra-Aortic Balloon Pump (IABP):
- Mechanism: Counter-pulsation. Inflates in diastole (↑ coronary perfusion), deflates in systole (↓ afterload).
- Use: Short-term, acute cardiogenic shock.
-
Ventricular Assist Devices (VADs):
- Types: LVAD, RVAD, BiVAD.
- Function: Unloads the ventricle, improving end-organ perfusion.
- Indications: Bridge-to-transplant, destination therapy.
- Complications: Thromboembolism, bleeding (GI), infection.
-
ECMO (Extracorporeal Membrane Oxygenation):
- VA-ECMO: Provides both cardiac and respiratory support.
- Use: Most severe cases, cardiac arrest.
⭐ Patients with continuous-flow LVADs often have a non-palpable pulse and require lifelong anticoagulation (e.g., Warfarin + Aspirin) to prevent pump thrombosis.
Heart Transplantation - The Ultimate Upgrade
-
Indications: End-stage HF with refractory cardiogenic shock, NYHA Class III-IV symptoms despite optimal therapy, intractable angina, or malignant arrhythmias.
-
Contraindications (Absolute): Active malignancy, irreversible end-organ damage (e.g., severe pulmonary HTN with PVR >5 Wood units), active infection, significant psychosocial instability.
- Immunosuppression: Triple therapy is standard.
- Calcineurin Inhibitor (e.g., Tacrolimus)
- Antimetabolite (e.g., Mycophenolate Mofetil)
- Corticosteroids (tapered)
⭐ Post-transplant Complications: In the first year, the leading cause of mortality is infection. After the first year, cardiac allograft vasculopathy (CAV) and malignancy are the primary causes.
Post-Transplant Hurdles - New Heart, New Problems
- Rejection: A primary threat to the allograft, categorized by timing and mechanism.
- Hyperacute: Occurs within minutes; mediated by pre-formed anti-donor antibodies.
- Acute Cellular: Peaks in the first 1-3 months; T-cell mediated. Diagnosed via endomyocardial biopsy showing lymphocytic infiltrates. Treated with high-dose corticosteroids.
- Chronic: Cardiac Allograft Vasculopathy (CAV) is the leading cause of late graft failure.
- Infection: High risk from immunosuppression. Prophylaxis is key against CMV, Pneumocystis jirovecii, and Aspergillus.
- Malignancy: Increased long-term risk, especially skin cancers and Post-Transplant Lymphoproliferative Disorder (PTLD).
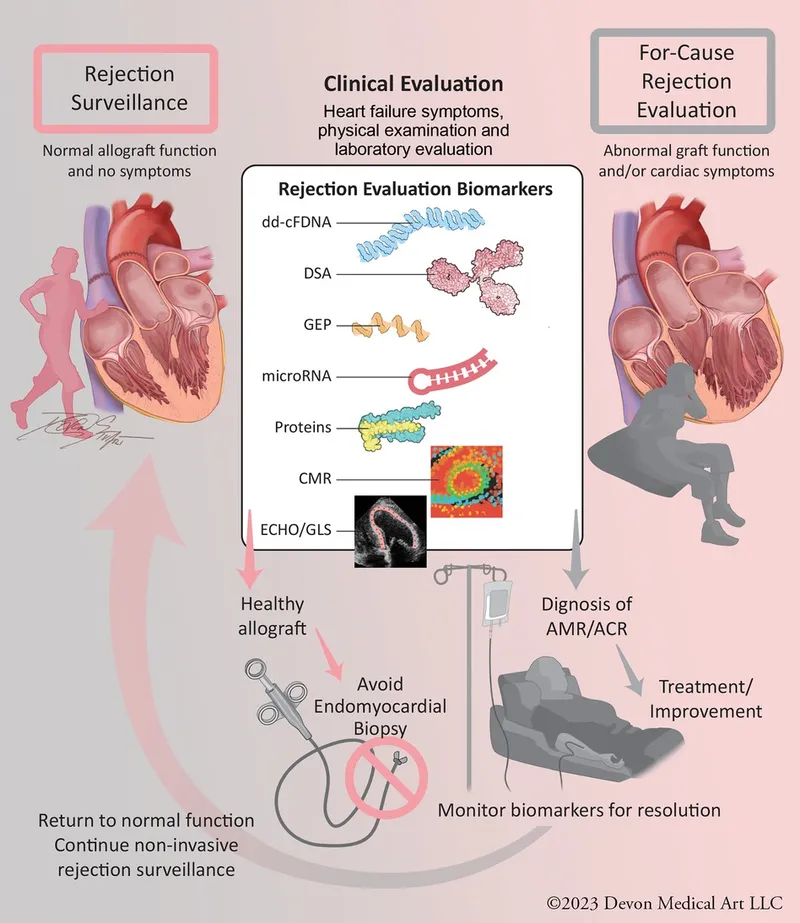
⭐ Cardiac Allograft Vasculopathy (CAV) is a diffuse, accelerated form of coronary artery disease in the transplanted heart. It's a leading cause of late graft failure and often clinically silent until advanced due to denervation of the donor heart.
High‑Yield Points - ⚡ Biggest Takeaways
- Advanced heart failure is defined by persistent, severe symptoms (NYHA Class III-IV) despite maximal medical and device therapy.
- Intravenous inotropes (e.g., milrinone) serve as a bridge to decision or for palliation but may increase long-term mortality.
- LVADs are used as a bridge to transplantation or as destination therapy; key risks include thrombosis, bleeding, and infection.
- Heart transplantation is the definitive therapy for eligible patients with refractory end-stage HF.
- Post-transplant issues include acute/chronic rejection, opportunistic infections, and cardiac allograft vasculopathy (CAV).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

