Pathophysiology - The Gut's Acid Trip
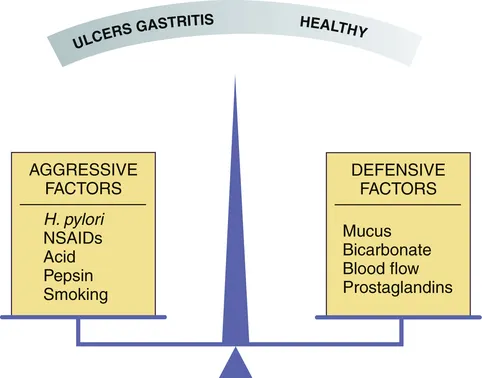
- Core Imbalance: Aggressive factors (gastric acid, pepsin) overwhelm mucosal defenses (mucus, bicarbonate, prostaglandins, blood flow).
- Two Main Culprits:
- H. pylori: Most common. Produces urease to survive in acid. Toxins (CagA, VacA) incite inflammation, leading to mucosal damage.
- NSAIDs: Inhibit COX-1, decreasing protective prostaglandins ($PGE_2$), which reduces mucus, bicarbonate, and mucosal blood flow.
⭐ In duodenal ulcers, H. pylori in the antrum decreases somatostatin output, leading to unchecked gastrin release and ↑ total acid production.
Presentation & Diagnosis - Spotting the Ulcer
- Hallmark: Epigastric pain (dyspepsia), often gnawing or burning.
- Duodenal Ulcer (DU): Pain 2-5 hours post-meal, at night. Relieved by food/antacids.
- Gastric Ulcer (GU): Pain 15-30 mins post-meal. Worsened by food, causing anorexia/weight loss.
- Alarm Features: Age >60, unintentional weight loss, progressive dysphagia, persistent vomiting, iron deficiency anemia, GI bleeding (melena/hematemesis).
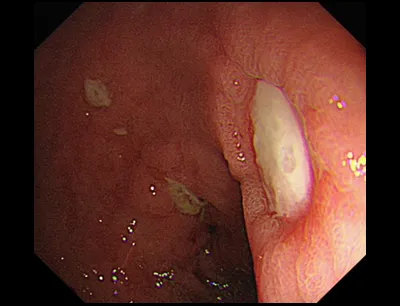
- Gold Standard: EGD (Endoscopy) for direct visualization & biopsy.
- Biopsy for histology & rapid urease test (H. pylori).
⭐ Exam Favorite: Any gastric ulcer found on imaging or endoscopy must be biopsied due to malignancy risk. Duodenal ulcers are almost never malignant.
Management - Dousing the Flames
- Core Goal: Heal existing ulcers & prevent recurrence.
- Acid Suppression: Proton Pump Inhibitors (PPIs) are first-line (e.g., Omeprazole). H2 blockers are second-line.
- H. pylori Eradication: Crucial if positive.
- Standard Triple Therapy: Clarithromycin + Amoxicillin + PPI for 14 days.
- Quadruple Therapy: (Used for macrolide resistance or treatment failure).
- 📌 Buy My Tasty Pepperoni: Bismuth subsalicylate + Metronidazole + Tetracycline + PPI.
- NSAID-Induced Ulcers: Discontinue NSAID if possible. If not, co-prescribe a PPI.
⭐ Warning: For gastric ulcers, always repeat endoscopy in 8-12 weeks after treatment to confirm healing and rule out underlying malignancy. Duodenal ulcers rarely harbor malignancy and do not require routine follow-up endoscopy.
Complications - When Ulcers Go Rogue
- Hemorrhage (Most Common): Presents as melena, hematemesis, or coffee-ground emesis. Endoscopy is crucial for diagnosis and hemostasis.
- Perforation: Acute, severe abdominal pain; a surgical emergency. Classic sign is free air under the diaphragm on upright chest X-ray.
- Gastric Outlet Obstruction (GOO): Caused by edema or scarring. Leads to early satiety, projectile non-bilious vomiting, and weight loss.
- Penetration: Ulcer erodes into an adjacent organ (e.g., pancreas), causing persistent, radiating back pain.
⭐ A posterior duodenal ulcer may perforate and erode the gastroduodenal artery, leading to massive hemorrhage.

High‑Yield Points - ⚡ Biggest Takeaways
- Most common causes: H. pylori infection and NSAID use.
- Classic symptom: Epigastric pain. Duodenal ulcers improve with food, while gastric ulcers worsen.
- Gold standard diagnosis: Upper endoscopy (EGD) with biopsy, especially for gastric ulcers to rule out malignancy.
- H. pylori treatment: Triple therapy (a PPI + clarithromycin + amoxicillin) is a standard regimen.
- Major complication: Perforation presents as sudden, severe abdominal pain and requires urgent surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

