Malabsorption - The Leaky Pipeline
- Pathophysiology: Impaired intestinal absorption of nutrients, leading to nutritional deficiencies & GI symptoms.
- Hallmark Sign: Steatorrhea (fatty, foul-smelling stools), weight loss, abdominal distension.
- Classification:
- Pre-mucosal: Defective digestion (e.g., pancreatic insufficiency).
- Mucosal: Damaged absorptive surface (e.g., Celiac disease, Whipple's disease).
- Post-mucosal: Impaired nutrient transport (e.g., lymphatic obstruction).
- Key Diagnostics:
- Qualitative stool fat (Sudan III stain).
- D-xylose test to differentiate mucosal from pancreatic causes.
⭐ D-xylose Test: A monosaccharide absorbed without pancreatic enzymes. A low urinary D-xylose level suggests mucosal damage (e.g., Celiac disease), as the intestine cannot absorb it.
Diagnostic Workup - Following the Clues
- Initial Labs: CBC (anemia), iron studies, folate, vitamin B12, albumin, prothrombin time (PT).
- Stool Studies:
- Qualitative: Sudan III stain for fecal fat.
- Quantitative: 72-hour fecal fat collection is the gold standard (abnormal: >7 g/day).
⭐ The D-xylose test is key: it's a monosaccharide absorbed in the proximal intestine without pancreatic enzymes. A low urinary/serum level after an oral dose points to mucosal defects (e.g., celiac disease), not pancreatic insufficiency.
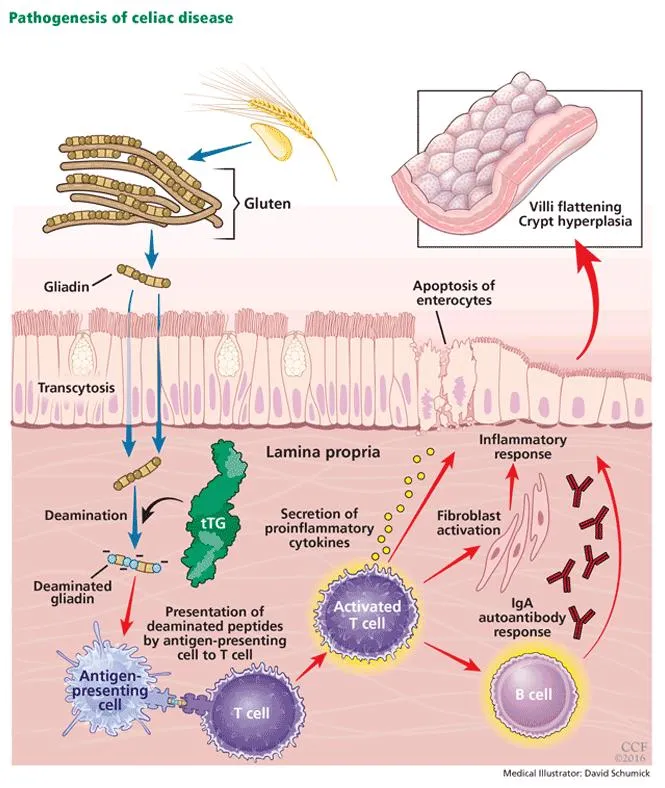
Celiac Disease - Gluten's Gut Grudge
- Pathophysiology: Autoimmune reaction to gliadin (a gluten protein) in individuals with HLA-DQ2/DQ8 haplotypes, leading to inflammation and damage of the small bowel mucosa.
- Clinical Features:
- GI: Chronic diarrhea/steatorrhea, bloating, weight loss.
- Extra-intestinal: Dermatitis herpetiformis (pruritic papulovesicular rash on extensor surfaces), iron deficiency anemia, fatigue.
- Diagnosis:
- Serology: ↑ IgA anti-tissue transglutaminase (tTG) is the preferred initial test.
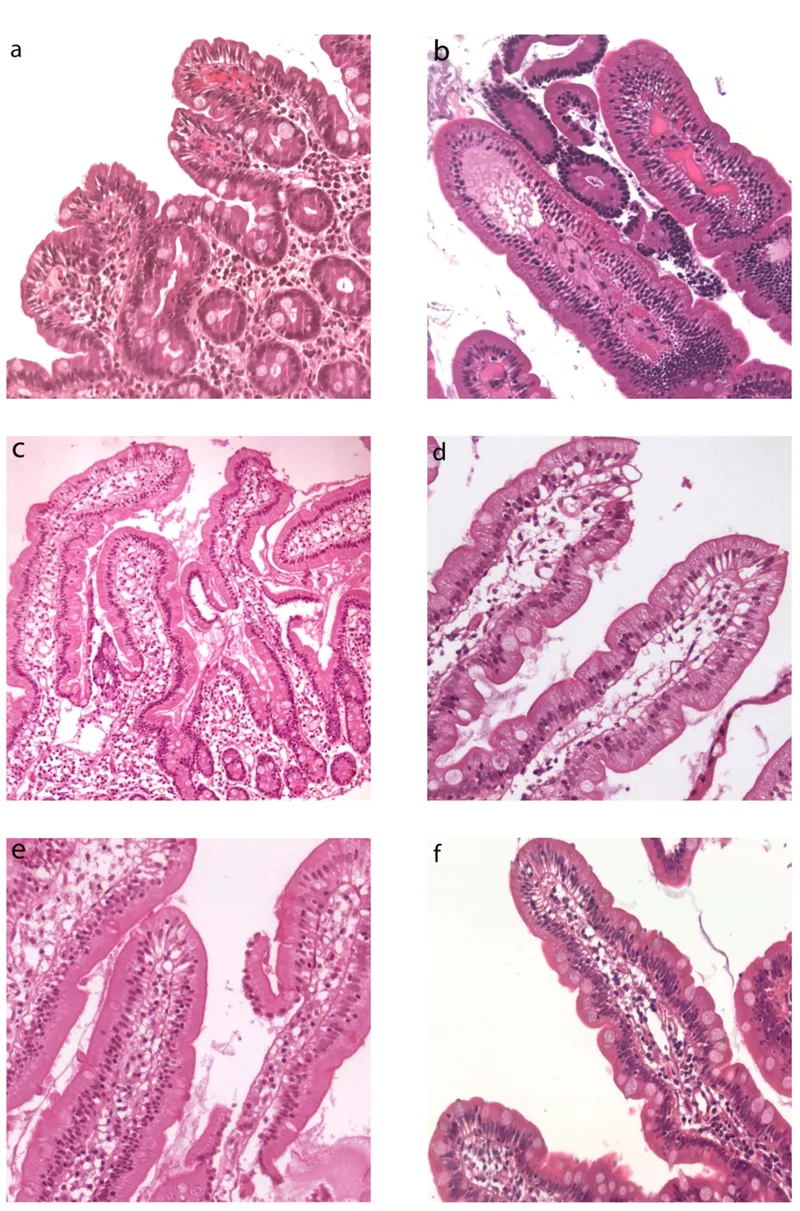
- Biopsy: Duodenal biopsy is the gold standard, showing villous atrophy, crypt hyperplasia, and intraepithelial lymphocytosis.
⭐ Associated Malignancy: Patients have an increased risk of developing enteropathy-associated T-cell lymphoma (EATL) and small bowel adenocarcinoma.
Other Syndromes - The Rogues' Gallery
-
Whipple Disease
- Systemic infection with Tropheryma whipplei.
- Presents with migratory polyarthritis, abdominal pain, diarrhea, and weight loss. May have CNS or cardiac signs.
- 📌 Mnemonic: "Foamy WHIPPed cream" for Foamy macrophages in Whipple disease.
-
⭐ Biopsy reveals PAS-positive, diastase-resistant macrophages in the lamina propria.
-
Tropical Sprue
- Acquired syndrome in tropical regions, likely infectious.
- Chronic diarrhea and megaloblastic anemia (↓ folate/B12) after travel.
- Responds to antibiotics (e.g., tetracycline) and folic acid.
-
Short Bowel Syndrome
- Malabsorption post-surgical resection. Severity depends on length/site.
- Loss of ileum is most critical (↓ bile salt and B12 absorption).
-
Small Intestinal Bacterial Overgrowth (SIBO)
- Excess bacteria deconjugate bile acids, causing malabsorption.
- Presents with bloating, flatulence, watery diarrhea.
High-Yield Points - ⚡ Biggest Takeaways
- Celiac disease is strongly associated with HLA-DQ2/DQ8, villous atrophy, and dermatitis herpetiformis.
- Whipple disease presents with a classic triad of diarrhea, weight loss, and arthralgia; look for PAS-positive macrophages on biopsy.
- Pancreatic insufficiency (e.g., chronic pancreatitis, cystic fibrosis) is a primary cause of steatorrhea and fat-soluble vitamin deficiencies.
- The D-xylose test helps distinguish mucosal defects (abnormal result) from pancreatic causes (normal result).
- Lactose intolerance causes osmotic diarrhea and bloating after dairy intake.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

