Esophageal Dysmotility - Unruly Swallowing
-
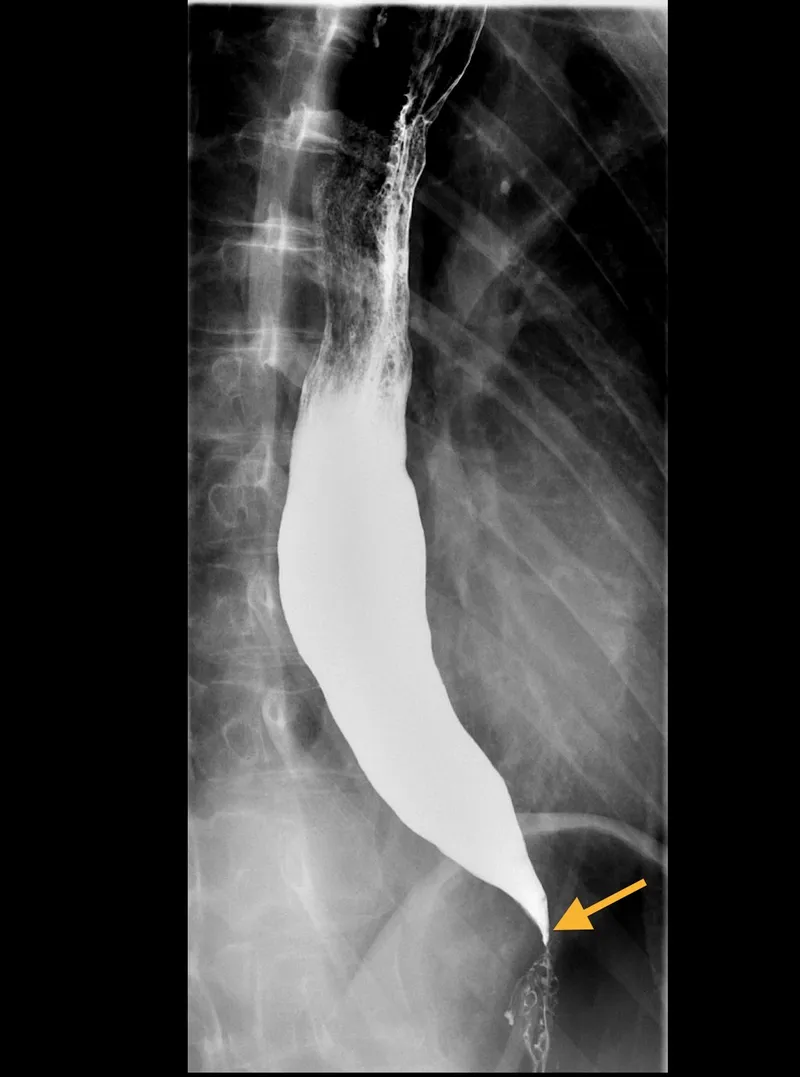
Achalasia: Failure of LES to relax + loss of peristalsis.
- Cause: Degeneration of inhibitory neurons in Auerbach's plexus.
- Barium swallow shows a "bird-beak" appearance.
- Manometry is diagnostic: ↑ LES pressure, incomplete relaxation.
-
Diffuse Esophageal Spasm (DES): Uncoordinated, strong contractions.
- Presents with intermittent chest pain and dysphagia.
- Barium swallow reveals a "corkscrew" or "rosary bead" esophagus.
- Manometry: High-amplitude, simultaneous contractions.
⭐ Exam Favorite: Chagas disease, caused by Trypanosoma cruzi, can destroy the myenteric plexus, leading to secondary achalasia.
Gastroparesis - The Stomach on Strike
Delayed gastric emptying without mechanical obstruction. Often linked to poor glycemic control in diabetics.
- Etiology: Idiopathic (~50%), Diabetes Mellitus (autonomic neuropathy), post-surgical (vagal injury), medications (opioids, anticholinergics).
- Clinical Features: Nausea, vomiting of undigested food, early satiety, bloating, abdominal pain.
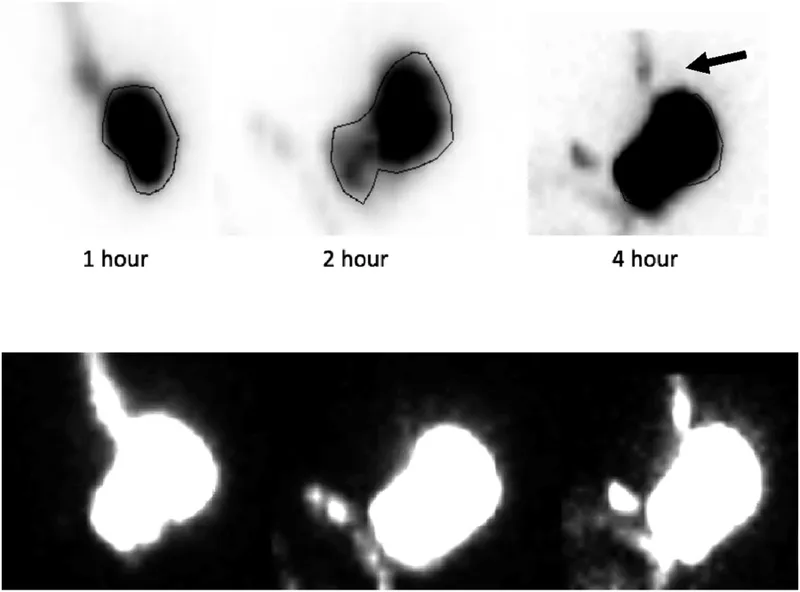
- Diagnosis: First, rule out mechanical obstruction with EGD. Gold standard is a gastric emptying study (scintigraphy) showing >10% retention at 4 hours.
- Management:
- Dietary modification: Small, frequent, low-fat, low-fiber meals.
- Prokinetics: Metoclopramide, Erythromycin.
⭐ Erythromycin acts on motilin receptors to promote gastric emptying, but its effectiveness can decrease over time due to tachyphylaxis.
Ileus & Pseudo-obstruction - Deceptive Standstills
- Paralytic Ileus: Functional, non-mechanical bowel hypomotility.
- Causes: Post-op (common), hypokalemia, sepsis, opiates.
- Clinical: N/V, absent bowel sounds, no flatus/stool.
- AXR: Uniformly dilated loops of both small & large bowel.
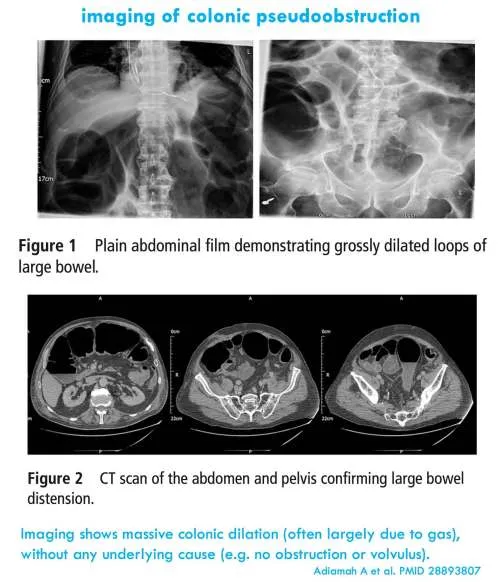
- Ogilvie's Syndrome (ACPO): Acute colonic pseudo-obstruction. Massive dilation without a physical blockage.
- Risk: Elderly, sick patients (trauma, infection).
- AXR: Cecal diameter >10-12 cm indicates high perforation risk.
⭐ Ogilvie's Syndrome: If conservative management fails, administer IV neostigmine. Must exclude mechanical obstruction first to prevent perforation.
Irritable Bowel Syndrome - The Sensitive Gut
- Chronic functional GI disorder characterized by abdominal pain and altered bowel habits. Core pathophysiology involves visceral hypersensitivity and gut-brain axis dysregulation.
- Diagnosis of Exclusion: Based on Rome IV criteria-recurrent abdominal pain (≥1 day/week in last 3 months) with ≥2 of:
- Related to defecation
- Change in stool frequency
- Change in stool form (Bristol Stool Scale)
- Subtypes: Predominant constipation (IBS-C), diarrhea (IBS-D), or mixed (IBS-M).
- Management: Lifestyle/dietary changes (low FODMAP), fiber, antispasmodics, and targeted therapy for constipation or diarrhea.
⭐ Alarm features warranting further investigation include rectal bleeding, nocturnal diarrhea, unintentional weight loss, anemia, and age of onset >50 years.
High-Yield Points - ⚡ Biggest Takeaways
- Achalasia presents with dysphagia to solids and liquids and a "bird's beak" on barium swallow, resulting from the loss of the myenteric plexus.
- GERD is most often caused by transient LES relaxation; its main complication is Barrett's esophagus, a precursor to adenocarcinoma.
- Diabetic gastroparesis is a state of delayed gastric emptying without obstruction; treat with metoclopramide.
- Hirschsprung disease is a congenital aganglionosis of the colon; diagnose with rectal biopsy.
- Diffuse esophageal spasm appears as a "corkscrew" esophagus on imaging.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

