GERD Pathophysiology - The Acid Backlash
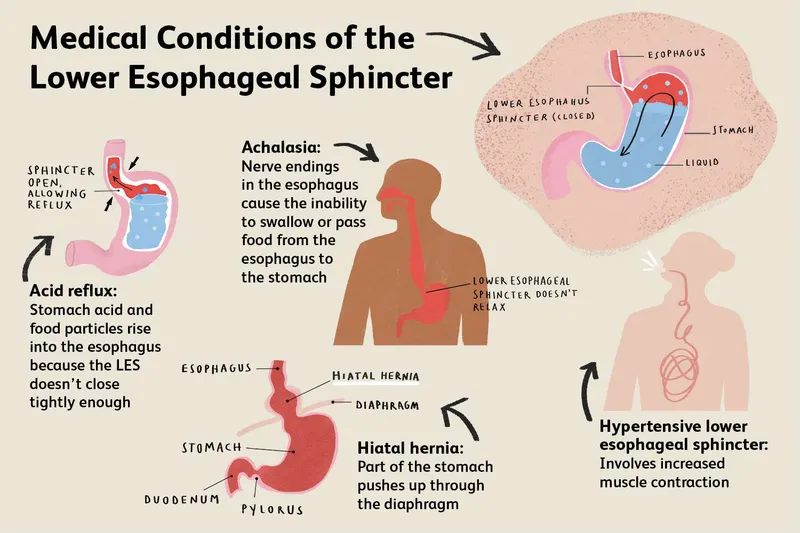
- Core Defect: ↓ Lower Esophageal Sphincter (LES) competence, leading to reflux of gastric contents.
- Key Mechanisms:
- Transient LES Relaxations (tLESRs): Most common cause (>60%). Not triggered by swallowing; often by gastric distention.
- Hypotensive (Low Pressure) LES: Resting pressure <10 mmHg.
- Anatomic Disruption: Hiatal hernia is a major contributor, displacing the gastroesophageal junction.
- Aggravating Factors:
- ↑ Intra-abdominal pressure (e.g., obesity, pregnancy).
- Delayed gastric emptying.
- Ineffective esophageal clearance.
⭐ Most reflux episodes occur due to transient LES relaxations (tLESRs), not a chronically hypotensive sphincter.
GERD Dx & Complications - Scope & Alarms
- Initial Dx: Primarily clinical. An empiric trial of a proton pump inhibitor (PPI) for 4-8 weeks is a common first step.
- Endoscopy (EGD) indicated for:
- Failure to respond to empiric PPI therapy.
- ⚠️ ALARM symptoms: Dysphagia, odynophagia, weight loss, anemia, GI bleeding.
- Screening for Barrett's in high-risk patients (chronic GERD >5 yrs, age >50).
- Complications: Erosive esophagitis, peptic stricture, Barrett's esophagus, and esophageal adenocarcinoma.
⭐ Barrett's esophagus is the single most important risk factor for esophageal adenocarcinoma, increasing risk 30-40x. Regular surveillance is key.
Motility Disorders - Pipe Problems
- Achalasia:
- Patho: Loss of Auerbach's (myenteric) plexus → LES fails to relax, loss of peristalsis.
- Sx: Dysphagia to solids and liquids.
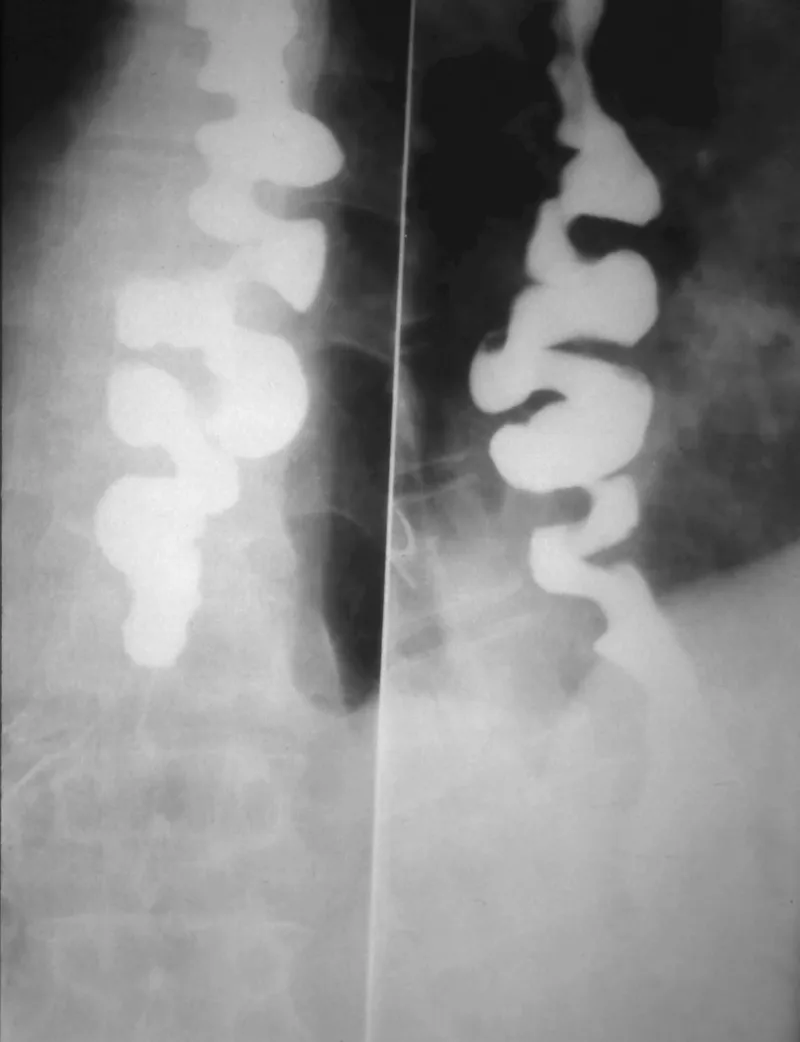
- Dx: Barium swallow shows "bird's beak." Manometry is gold standard (↑ LES pressure, aperistalsis).
- 📌 Mnemonic: Achalasia = Aperistalsis.
- Diffuse Esophageal Spasm (DES):
- Patho: Impaired inhibitory innervation → strong, uncoordinated contractions.
- Sx: Intermittent chest pain, dysphagia.
- Dx: Barium shows "corkscrew" esophagus. Manometry confirms.
- Tx: CCBs, nitrates.
- Scleroderma Esophagus:
- Patho: Collagen deposition & fibrosis → smooth muscle atrophy → ↓ LES tone & aperistalsis.
- Sx: Severe GERD, dysphagia. Often part of CREST syndrome.
⭐ Chagas disease (Trypanosoma cruzi infection) can cause secondary achalasia by destroying the myenteric plexus.
Other Esophagitides - Beyond Reflux
- Eosinophilic (EoE): Atopic young males with solid food dysphagia. Endoscopy shows rings ("trachealization"), furrows. Biopsy is key: ≥15 eosinophils/hpf. Tx: PPI trial, swallowed corticosteroids, elimination diet.
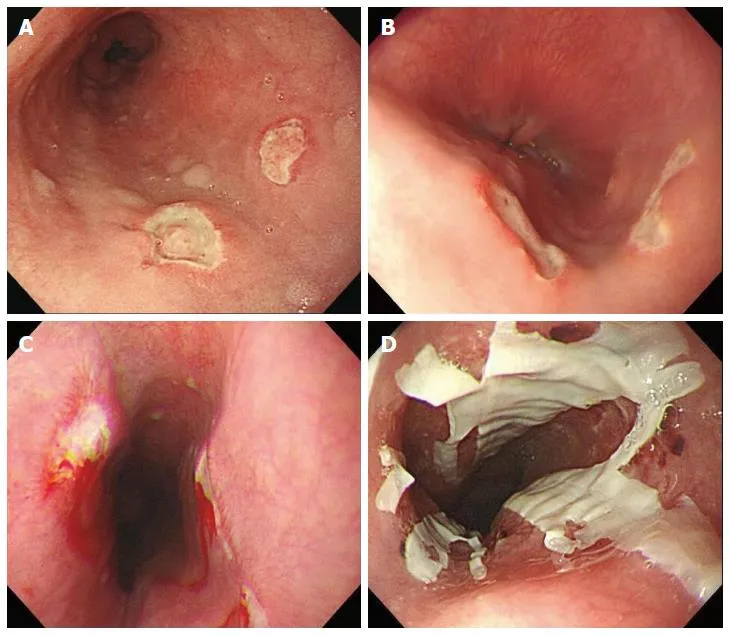
- Pill-Induced: Sudden odynophagia. Common meds: Bisphosphonates, Tetracyclines, NSAIDs, KCl. Endoscopy: discrete ulcer at sites of narrowing. 📌 Take pills with 4 oz water & stay upright for 30 min.
- Infectious: Occurs in immunocompromised hosts.
- Candida: White linear plaques. Tx: Fluconazole.
- CMV: Large, shallow linear ulcers. Tx: Ganciclovir.
- HSV: Small, deep, "punched-out" ulcers. Tx: Acyclovir.
⭐ In Eosinophilic Esophagitis, patients often have a history of food impaction requiring endoscopic intervention.
High‑Yield Points - ⚡ Biggest Takeaways
- GERD is caused by transient LES relaxation. The main complication is Barrett's esophagus, a precursor to adenocarcinoma.
- 24-hour pH monitoring is the diagnostic gold standard; endoscopy is for alarm symptoms.
- Achalasia presents with dysphagia to solids and liquids and a "bird's beak" sign.
- Eosinophilic esophagitis is seen in atopic patients; endoscopy shows trachealization.
- Adenocarcinoma is linked to Barrett's (distal 1/3); squamous cell to smoking/alcohol (proximal 2/3).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

