Basics & Pathophysiology - Gut's Little Pockets
- Diverticulosis: Asymptomatic herniation of mucosa and submucosa through the muscularis propria, forming pseudodiverticula.
- Diverticulitis: Inflammation and potential microperforation of a diverticulum, often due to an obstructing fecalith.
- Pathophysiology: Chronic low-fiber diet and constipation ↑ intraluminal pressure. This forces outpouchings at weak points in the colonic wall, typically where the vasa recta penetrate the circular muscle layer.
- Location: Predominantly affects the sigmoid colon (~95%) due to its narrow diameter, which generates the highest wall tension per Laplace's law.
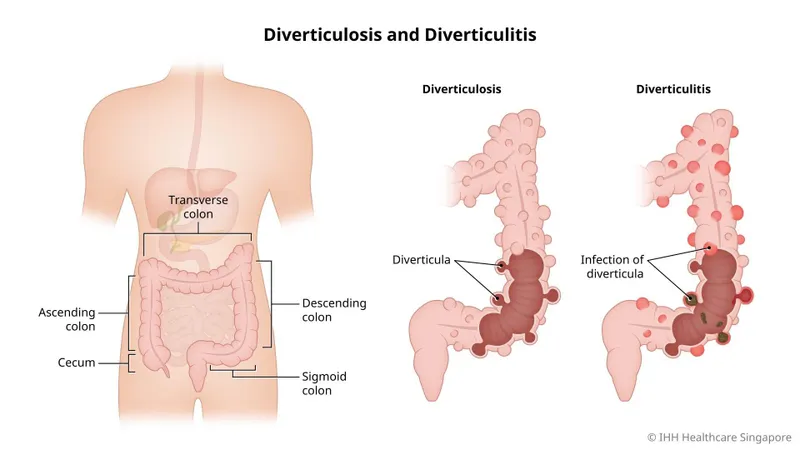
⭐ Most colonic diverticula are pseudodiverticula (false diverticula), lacking a muscularis externa layer. True diverticula, containing all gut wall layers, are rare (e.g., Meckel's diverticulum).
Presentation & Diagnosis - When Pockets Protest
- Asymptomatic Diverticulosis: The majority of cases. Usually an incidental finding during a colonoscopy performed for other reasons.
- Acute Diverticulitis Presentation:
- Classic: Constant, aching LLQ pain (sigmoid colon is the most common site).
- Associated: Low-grade fever, anorexia, nausea, and a change in bowel habits (constipation or diarrhea).
- Physical Exam: Localized LLQ tenderness, guarding, and sometimes a palpable, tender mass.
- Diagnostic Gold Standard:
- Abdominal/Pelvic CT scan with IV contrast is the preferred imaging test.
- Key CT findings: Focal bowel wall thickening (>4 mm), pericolic fat stranding, abscess, or free air (perforation).
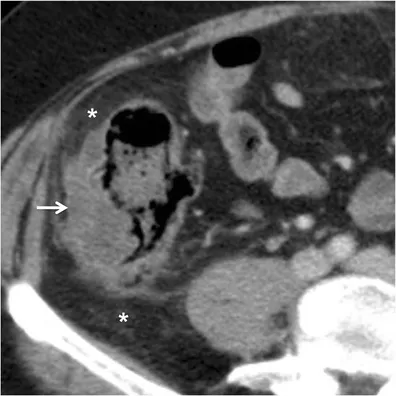
- ⚠️ Contraindicated in Acute Phase: Colonoscopy and barium enema due to high perforation risk. Perform 6-8 weeks post-resolution to rule out malignancy.
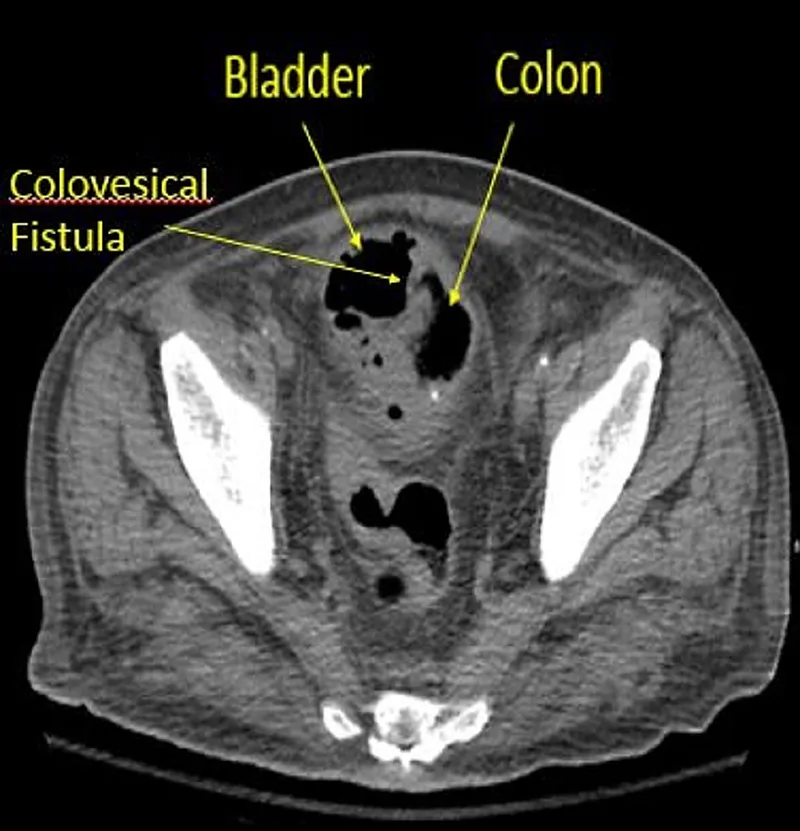
⭐ The most common fistula in diverticulitis is a colovesical fistula, presenting with pneumaturia (air in urine), fecaluria, and recurrent UTIs.
Management Algorithm - Calming the Colon
- Antibiotics: Cover gram-negatives & anaerobes (e.g., Ciprofloxacin + Metronidazole) for 7-10 days.
- Complicated Cases:
- Abscess > 3 cm: Percutaneous drainage.
- Perforation / Peritonitis: Emergent surgery (e.g., Hartmann's procedure).
- Post-Recovery: High-fiber diet to prevent recurrence. All patients need a follow-up colonoscopy to exclude malignancy.
⭐ After an initial episode of uncomplicated diverticulitis, colonoscopy is crucial to rule out an underlying colorectal cancer, which can present with a similar clinical and radiographic picture.
Complications - Danger Zones
- Abscess: Most common complication; suspect with persistent fever despite antibiotics.
- Fistula: Colovesical is classic → pneumaturia, fecaluria. Colovaginal also possible.
- Obstruction: Can cause large bowel obstruction from stricturing or edema.
- Perforation: Free air on imaging; high risk of sepsis.
- Bleeding (Painless): Abrupt, large-volume hematochezia.
⭐ While most diverticular bleeding stops spontaneously (>75%), colovesical fistula is the most common fistula type associated with diverticulitis.
- Diverticulosis is typically asymptomatic; diverticulitis is inflammation/infection of a diverticulum.
- Most common cause of painless lower GI bleeding in adults >60 years old.
- Acute diverticulitis presents with LLQ abdominal pain, fever, and leukocytosis.
- CT scan of the abdomen and pelvis is the best initial test for diagnosis.
- Colonoscopy is contraindicated during an acute episode due to perforation risk.
- Uncomplicated cases are treated with bowel rest and antibiotics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

