Hemorrhoids - Piles of Problems
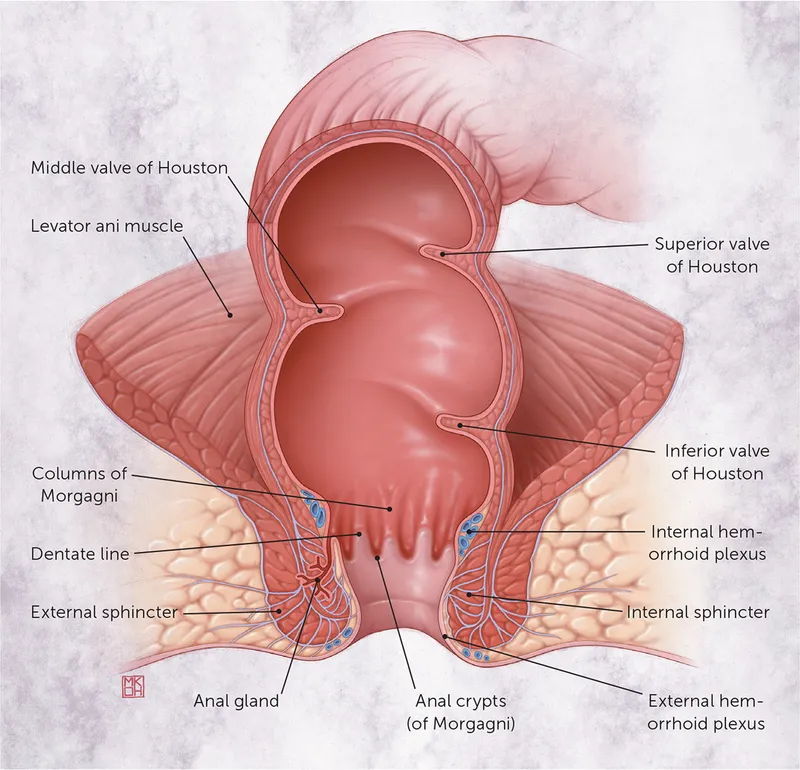
Dilated submucosal veins in the anorectal canal.
- Internal: Above dentate line (visceral afferents) → painless bright red bleeding. Graded I-IV.
- External: Below dentate line (somatic nerves) → painful, especially if thrombosed.
- Risks: Constipation, straining, pregnancy, portal HTN.
⭐ Acute, severe anorectal pain plus a tender, bluish nodule at the anal verge points strongly to a thrombosed external hemorrhoid.
Anal Fissures - Tears for Fears
- Definition: Longitudinal tear in the anoderm, distal to the dentate line.
- Etiology: Trauma from hard stool, local ischemia. Most common in the posterior midline.
- Clinical: Severe, tearing pain with defecation; bright red blood on toilet paper.
- Acute: < 6 weeks; superficial tear.
- Chronic: > 6 weeks; may have a sentinel pile (skin tag) and hypertrophied anal papilla.

- Management:
- Conservative: High-fiber diet, stool softeners, sitz baths.
- Medical: Topical vasodilators (nifedipine, nitroglycerin) to ↓ sphincter pressure.
- Surgical: Lateral internal sphincterotomy (LIS) for refractory cases.
⭐ Exam Favorite: Fissures located off the midline should raise suspicion for secondary causes like Crohn's disease, HIV, syphilis, or tuberculosis.
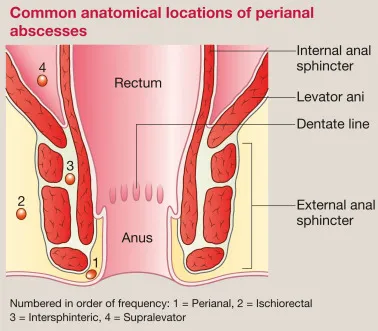
Anorectal Abscess & Fistula - Tracts of Trouble
- Anorectal Abscess: Arises from an infected anal crypt gland. Presents with acute, severe, constant perianal pain and swelling. Fever is common.
- Causative Organisms: E. coli, Bacteroides, Staphylococcus.
- Management: Crucial first step is incision and drainage (I&D). Antibiotics are secondary.
- Fistula-in-Ano: A chronic complication in ~50% of abscesses; an epithelialized tract connecting the abscess source to the perianal skin, causing persistent drainage.
⭐ Goodsall's Rule predicts fistula tract anatomy. Anterior external openings connect via a simple, straight radial tract. Posterior openings follow a complex, curved path to the posterior midline before entering the anal canal.
Fecal Incontinence - Leaky Logic
- Etiology: Most commonly due to obstetric trauma (pudendal nerve injury, sphincter laceration). Other causes: neurogenic (diabetes, spinal cord injury), overflow (impaction), or iatrogenic.
- Initial Management: Conservative approach first.
- Dietary modification (bulk-forming agents like psyllium).
- Pelvic floor exercises (Kegel exercises).
- Anti-diarrheal agents (loperamide).
⭐ Exam Favorite: Fecal incontinence presenting years after childbirth is often due to delayed pudendal nerve neuropathy. The nerve is stretched during delivery, leading to a progressive decline in sphincter function over time.
High‑Yield Points - ⚡ Biggest Takeaways
- Anal fissures cause tearing pain with defecation, typically at the posterior midline. A lateral fissure suggests Crohn's disease or other systemic illness.
- Internal hemorrhoids manifest with painless, bright red rectal bleeding. In contrast, external hemorrhoids are acutely painful when thrombosed.
- An anorectal abscess is a painful emergency requiring incision and drainage; it may evolve into a fistula-in-ano, strongly associated with Crohn's disease.
- Proctitis from STIs or IBD presents with tenesmus and discharge.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

