VHD Basics - The Squeaky Leaky Gates
- Stenosis (Squeaky Gate): Narrowed valve obstructs forward flow, causing a pressure gradient ($↑ΔP$). Leads to pressure overload & concentric hypertrophy.
- Regurgitation/Insufficiency (Leaky Gate): Valve doesn't close, causing backflow. Leads to volume overload & eccentric hypertrophy.
- Murmurs are turbulent blood flow sounds.
⭐ Dynamic Auscultation: Maneuvers that ↑ preload (squatting, leg raise) generally ↑ murmur intensity, except in HOCM and MVP click/murmur. Handgrip (↑ afterload) ↑ regurgitant murmurs (AR, MR, VSD).
Aortic Valve Dramas - The Pressure Cooker & Blowback
-
Aortic Stenosis (AS): Pressure Cooker
- LV outflow obstruction → concentric LV hypertrophy.
- 📌 SAD Triad: Syncope, Angina, Dyspnea on exertion.
- Systolic crescendo-decrescendo murmur radiating to carotids.
-
Aortic Regurgitation (AR): Blowback
- Backflow → LV volume overload → eccentric hypertrophy.
- Diastolic, high-pitched, blowing murmur.
- Wide pulse pressure ($↑P_{systolic} - ↓P_{diastolic}$), water-hammer pulse.
⭐ Heyde's Syndrome: Aortic stenosis can cause acquired von Willebrand disease, leading to GI bleeding from angiodysplasia.
Mitral Valve Mishaps - The Rumbling Domino & Floppy Flap
-
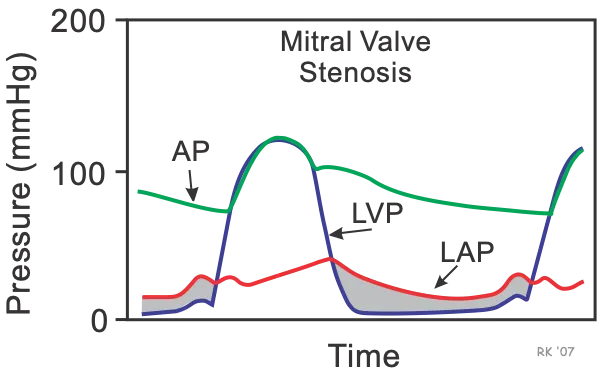
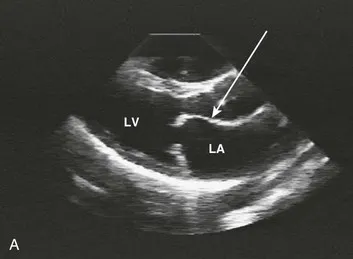
Mitral Stenosis (MS) - The Rumbling Domino
- Etiology: Chronic rheumatic heart disease is the primary cause.
- Auscultation: Loud S1, an opening snap after S2, followed by a low-pitched mid-diastolic rumble.
- Pathophys: Valve leaflets thicken and fuse → obstructs LV inflow → ↑LA pressure.
-
Mitral Regurgitation (MR) & Prolapse (MVP) - The Floppy Flap
- Etiology: MVP (myxomatous degeneration), ischemic damage, infective endocarditis.
- Auscultation:
- MVP: Mid-systolic click, may have a late systolic murmur.
- MR: Holosystolic murmur, radiates to the axilla.
⭐ Ortner's Syndrome: Severe mitral stenosis can cause massive left atrial enlargement, which may compress the left recurrent laryngeal nerve, leading to hoarseness.
Right-Sided & MVP Quirks - The Other Valves
- Tricuspid Regurgitation (TR): Holosystolic murmur at left lower sternal border. Common causes: RV dilation, infective endocarditis (esp. IVDU). 📌 Right-sided murmurs ↑ with Inspiration.
- Pulmonic Stenosis (PS): Harsh, systolic ejection murmur ± click at left upper sternal border. Usually a congenital defect (e.g., Tetralogy of Fallot).
- Mitral Valve Prolapse (MVP): Mid-systolic click, late systolic murmur. Due to myxomatous degeneration.
⭐ MVP Maneuvers: Standing/Valsalva (↓ preload) → click is earlier, murmur is longer. Squatting (↑ preload) → click is later, murmur is shorter.
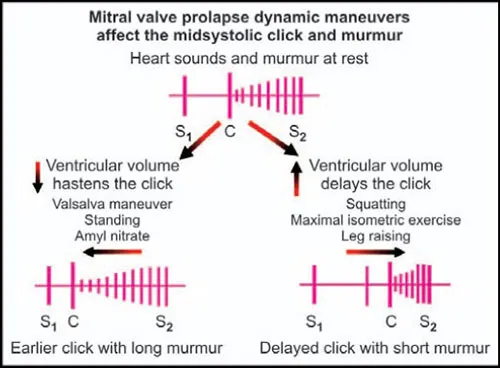
Murmur Maneuvers - Shifting Sounds & Squats
| Maneuver | Action | Most Murmurs | HOCM / MVP |
|---|---|---|---|
| Valsalva, Standing | ↓ Preload | ↓ Intensity | ↑ Intensity |
| Squatting, Leg Raise | ↑ Preload | ↑ Intensity | ↓ Intensity |
| Handgrip | ↑ Afterload | ↑ AR, MR, VSD | ↓ HOCM, AS |
📌 Think: A smaller, emptier ventricle (↓ preload) worsens the outflow obstruction in HOCM and increases prolapse in MVP.
High-Yield Points - ⚡ Biggest Takeaways
- Aortic Stenosis presents with the classic triad of Syncope, Angina, and Dyspnea (SAD).
- Mitral Stenosis is almost always due to rheumatic fever and features an opening snap.
- Aortic Regurgitation is characterized by a diastolic decrescendo murmur and wide pulse pressure.
- Mitral Regurgitation presents as a holosystolic murmur radiating to the axilla.
- Valsalva and standing decrease preload, making most murmurs quieter except for MVP and HOCM.
- Inspiration selectively increases the intensity of right-sided heart murmurs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

