Initial Screen - First Steps First
The initial step is to determine surgical urgency and identify any active cardiac conditions. These are major clinical predictors that mandate intensive management and may delay or cancel elective surgery.
- Unstable Coronary Syndromes:
- Acute MI (<7 days) or recent MI (7-30 days) with evidence of significant ischemic risk.
- Unstable or severe angina.
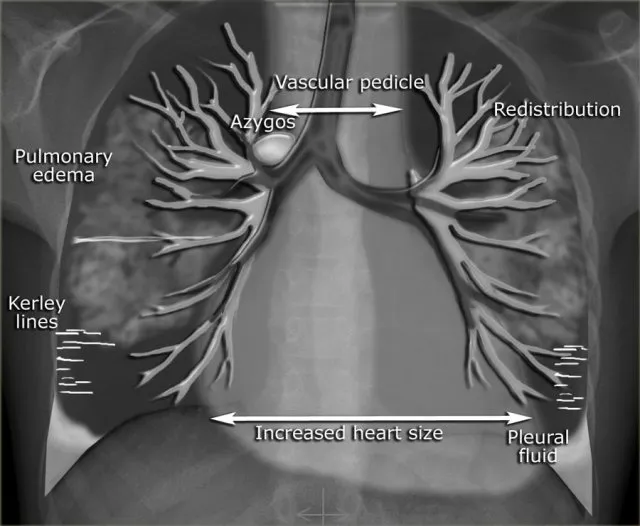
- Decompensated Heart Failure: NYHA Class IV symptoms or worsening pulmonary edema.
- Significant Arrhythmias: High-grade AV block, symptomatic ventricular arrhythmias, supraventricular arrhythmias with uncontrolled rate (>100 bpm).
- Severe Valvular Disease: Symptomatic severe aortic or mitral stenosis.
⭐ For emergent procedures, the pre-operative evaluation is bypassed. The focus shifts to intra-operative and post-operative risk mitigation and surveillance.
Risk Calculators - The Numbers Game
-
Revised Cardiac Risk Index (RCRI): Estimates risk of major adverse cardiac events (MACE).
- 1 point for each of:
- High-risk surgery (intraperitoneal, intrathoracic, suprainguinal vascular)
- History of Ischemic Heart Disease
- History of Congestive Heart Failure
- History of Cerebrovascular Disease (Stroke/TIA)
- Pre-operative Insulin use
- Pre-operative Serum Creatinine >2.0 mg/dL
- Scores & Risk: 0 pts (0.4%), 1 pt (0.9%), 2 pts (6.6%), ≥3 pts (11%).
- 1 point for each of:
-
ACS NSQIP Surgical Risk Calculator: More comprehensive online tool; uses 20+ patient variables.
⭐ In patients with stable coronary artery disease, routine pre-operative coronary revascularization (PCI/CABG) before non-cardiac surgery has NOT been shown to reduce perioperative MACE.
Functional Capacity & Testing - METs & Stress
-
Metabolic Equivalents (METs): A measure of exercise capacity. 1 MET is the resting metabolic rate.
- < 4 METs: Poor capacity. (e.g., slow walking, self-care, light housework)
- 4-10 METs: Moderate to good. (e.g., climbing stairs, brisk walking, golf)
- > 10 METs: Excellent capacity. (e.g., running, swimming, strenuous sports)
-
Assessment Guideline: If a patient can achieve ≥ 4 METs without symptoms, they have a low risk of perioperative cardiac events and may not require further testing.
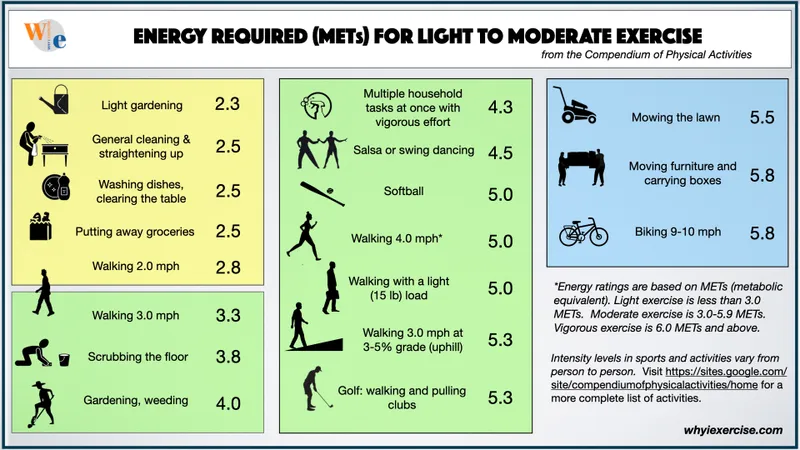 levels for various physical activities)
levels for various physical activities)
- Stress Testing: Indicated for patients with poor (< 4 METs) or unknown functional capacity undergoing elevated-risk surgery.
- Exercise ECG: For patients who can exercise with a normal baseline ECG.
- Pharmacologic Stress: For non-ambulatory patients.
- Vasodilators (adenosine, regadenoson) + nuclear imaging.
- Inotropes (dobutamine) + echocardiography.
⭐ Inability to climb two flights of stairs or walk four blocks (i.e., < 4 METs) is a key indicator of poor functional capacity and a strong predictor of postoperative cardiac complications.
Peri-Op Meds - To Stop or Not
-
CONTINUE:
- Beta-blockers: Prevents withdrawal tachycardia and ischemia.
- Statins: Plaque stabilization benefits.
- Alpha-2 agonists (Clonidine).
-
HOLD on Day of Surgery:
- ACE Inhibitors / ARBs: Risk of refractory hypotension.
- Diuretics: To avoid hypovolemia & electrolyte shifts.
- SGLT2 inhibitors: Risk of euglycemic DKA.
-
MANAGE (Bleed vs. Clot Risk):
- Antiplatelets (Aspirin, Clopidogrel): Stop 5-7 days prior unless stent thrombosis risk is high.
- Anticoagulants (Warfarin, DOACs): Bridge with heparin if high thromboembolic risk.
⭐ While beta-blockers must be continued, starting them de novo just before non-cardiac surgery in naive patients is not routinely recommended and may increase stroke risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Emergent surgeries bypass pre-op cardiac evaluation; proceed with medical optimization.
- The Revised Cardiac Risk Index (RCRI) is the primary tool for risk stratification.
- Poor functional capacity (<4 METs) is a major independent predictor of adverse cardiac events.
- Active cardiac conditions like unstable angina or decompensated HF require postponing elective surgery.
- Further cardiac testing is only indicated if the results will change management.
- Continue chronic beta-blockers; do not initiate them immediately before surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

