Pericardial Anatomy - The Heart's Sac
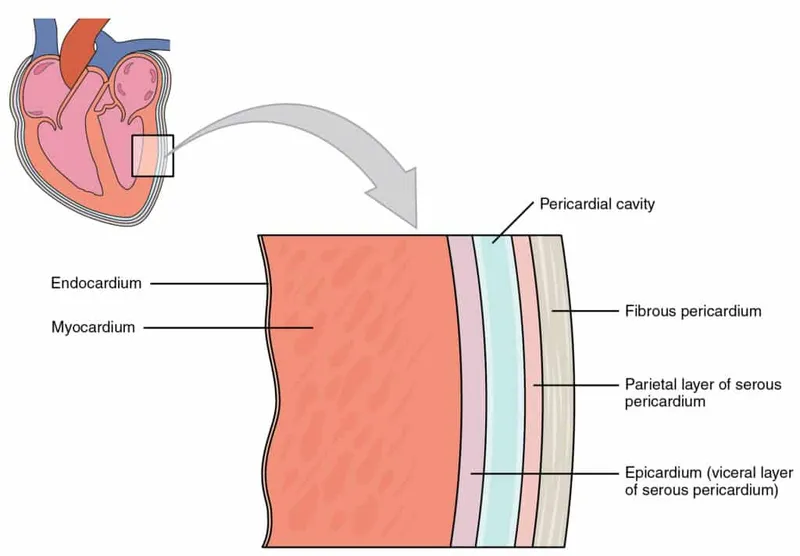
- Structure: A fibro-serous, double-walled sac enclosing the heart.
- Fibrous Pericardium: Tough, inelastic outer layer. Anchors the heart.
- Serous Pericardium: Thin, double-layered membrane.
- Parietal layer: Lines the inner surface of the fibrous pericardium.
- Visceral layer (Epicardium): Adheres to the heart muscle.
- Pericardial Cavity: The potential space between the two serous layers. Contains 15-50 mL of ultrafiltrate for lubrication.
⭐ Clinical Pearl: The phrenic nerve (C3-C5) innervates the pericardium, causing referred pain to the trapezius ridge (shoulder) in pericarditis.
Acute Pericarditis - Fiery Friction Rub
- Etiology: Primarily idiopathic (viral, e.g., Coxsackie B), post-MI (early or Dressler syndrome), uremia, autoimmune (SLE), malignancy.
- Clinical Triad:
- Chest Pain: Sharp, pleuritic, and postural-worsens when supine, improves by leaning forward.
- Pericardial Friction Rub: High-pitched, scratchy sound best heard at the left sternal border; may be transient.
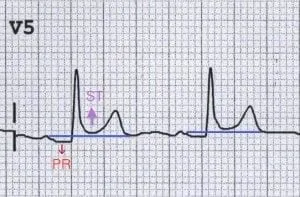
- ECG Changes: Diffuse, concave ST-segment elevation and PR depression.
- Diagnostics:
- ECG is key. Echocardiogram to assess for complications like pericardial effusion.
- ECG is key. Echocardiogram to assess for complications like pericardial effusion.
- Management:
- NSAIDs (e.g., ibuprofen) and colchicine (reduces recurrence).
- Corticosteroids for refractory cases or contraindications to NSAIDs.
⭐ PR-segment depression is the most specific ECG finding for acute pericarditis.
Effusion & Tamponade - Beck's Deadly Trio
-
Pericardial Effusion: Abnormal fluid in the pericardial sac, impairing cardiac function.
- Etiology: Often idiopathic/viral; also uremia, malignancy, post-MI (Dressler's).
- Clinical: May be asymptomatic. Look for dyspnea, cough, distant heart sounds.
- Diagnostics:
- ECG: Low-voltage QRS, electrical alternans (swinging heart).
- CXR: Enlarged, globular, "water-bottle" cardiac silhouette.
- Echo: Gold standard for detection.
-
Cardiac Tamponade: Life-threatening compression from a large/rapid effusion.
- 📌 Beck's Triad: Hypotension + Jugular Venous Distension (JVD) + Muffled Heart Sounds.
- Pulsus Paradoxus: Inspiratory systolic BP drop >10 mmHg.
- Management: Urgent pericardiocentesis.
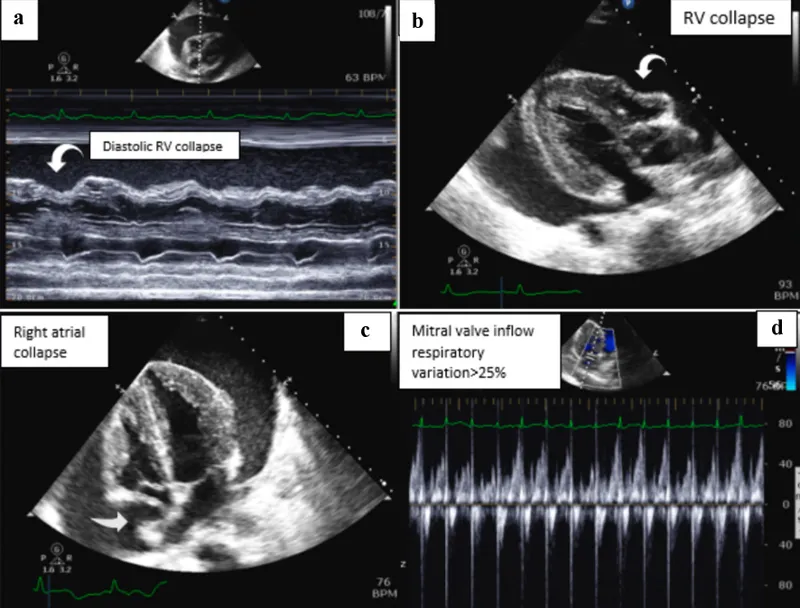
⭐ Echocardiography is key, showing right atrial and ventricular diastolic collapse-the most specific sign of tamponade.
Constrictive Pericarditis - Heart in a Cage
- Pathophysiology: Thickened, fibrotic, often calcified pericardium encases the heart, severely limiting diastolic filling.
- Etiologies: Idiopathic/viral, post-cardiac surgery, radiation therapy, tuberculosis.
- Clinical Signs:
- Right heart failure signs dominate: ascites, peripheral edema, hepatomegaly.
- Kussmaul's sign: Paradoxical ↑ in JVP with inspiration.
- Pericardial knock: High-pitched early diastolic sound.
- Diagnosis:
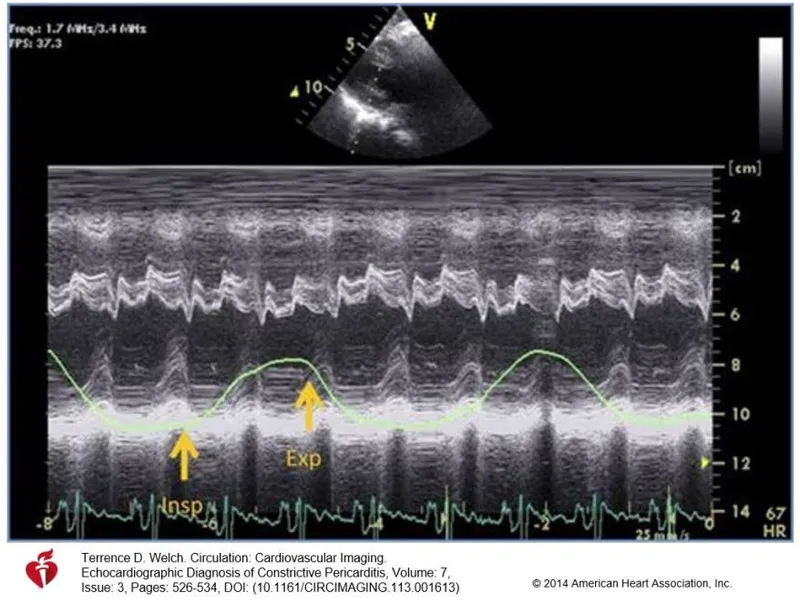
- Echocardiogram: Septal bounce, respiratory interventricular dependence.
- Cardiac Cath: Equalization of diastolic pressures across all chambers; "dip-and-plateau" or square root sign in ventricular pressure tracings.
⭐ In constrictive pericarditis, ventricular diastolic pressures (RVEDP & LVEDP) are equalized and high, typically within 5 mmHg of each other.
High‑Yield Points - ⚡ Biggest Takeaways
- Acute pericarditis presents with pleuritic chest pain that improves when leaning forward, a friction rub, and diffuse ST-segment elevation.
- Cardiac Tamponade is marked by Beck's triad (hypotension, JVD, muffled heart sounds) and pulsus paradoxus (>10 mmHg SBP drop on inspiration).
- Constrictive Pericarditis features a pericardial knock, Kussmaul's sign (JVP ↑ on inspiration), and signs of right-sided heart failure.
- Electrical alternans on EKG is highly specific for a large pericardial effusion.
- Dressler syndrome is a delayed, post-MI autoimmune pericarditis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

