Diagnosis & Staging - The Pressure Check
- Proper Measurement: Rest 5 min, no caffeine/exercise 30 min prior. Use correct cuff size on a bare arm, supported at heart level.
- Diagnosis: Based on an average of ≥2 readings on ≥2 separate occasions.
| Category | Systolic (SBP) | Diastolic (DBP) | |
|---|---|---|---|
| Normal | <120 | and | <80 |
| Elevated | 120-129 | and | <80 |
| Stage 1 | 130-139 | or | 80-89 |
| Stage 2 | ≥140 | or | ≥90 |
Etiology & Complications - The Usual Suspects
- Primary (Essential) Hypertension: >90% of cases; idiopathic, multifactorial (genetics, age, obesity, salt).
- Secondary Hypertension: Suspect in young (<30), resistant, or acute-onset severe HTN.
- 📌 Mnemonic: CHAPS (Cushing's, Hyperaldosteronism, Aortic coarctation, Pheochromocytoma, Stenosis of renal arteries).
| Secondary Cause | Classic Clue |
|---|---|
| Renal Artery Stenosis (RAS) | Abdominal bruit, ↑Creatinine with ACE-I |
| Primary Aldosteronism | HTN with hypokalemia, metabolic alkalosis |
| Pheochromocytoma | Paroxysmal HTN, palpitations, headache, sweating |
| Cushing's Syndrome | Central obesity, striae, hyperglycemia |
| Obstructive Sleep Apnea (OSA) | Snoring, daytime somnolence |
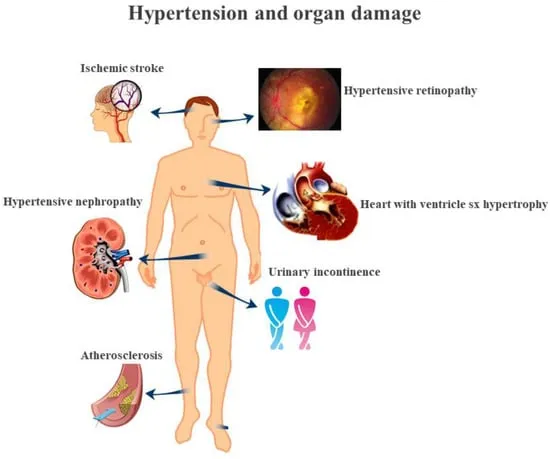
- **Heart**: Left Ventricular Hypertrophy (LVH), Heart Failure
- **Brain**: Stroke, dementia
- **Kidney**: Chronic Kidney Disease (CKD)
- **Eyes**: Hypertensive retinopathy
⭐ In a young female with new-onset hypertension and an abdominal bruit, suspect fibromuscular dysplasia as the cause of renal artery stenosis.
Treatment Algorithm - The Pressure Drop
The universal treatment goal is a blood pressure <130/80 mmHg.
- Lifestyle Modification is foundational: Enforce DASH diet, aerobic exercise (150 min/week), sodium restriction (<1.5g/day), weight loss, and limited alcohol.
- Pharmacotherapy: If lifestyle changes are insufficient, initiate a first-line agent. For most, this includes Thiazide diuretics, ACE inhibitors (ACEi)/ARBs, or long-acting Dihydropyridine Calcium Channel Blockers (CCBs).
- 📌 Mnemonic for major classes: A B C D (ACEi/ARB, Beta-blocker, CCB, Diuretic).
Choice of initial drug is heavily guided by compelling indications.
⭐ ACE inhibitors can cause a dry, non-productive cough due to bradykinin accumulation. Angiotensin II Receptor Blockers (ARBs) do not have this side effect and are the preferred alternative in such cases.
Special Cases & Crises - Code Red Pressure
| Feature | Hypertensive Urgency | Hypertensive Emergency |
|---|---|---|
| Definition | BP >180/120 mmHg | BP >180/120 mmHg + acute end-organ damage |
| Goal | Gradual ↓BP | Lower MAP by ~25% in 1st hour |
| Timeline | 24-48 hours | Immediate |
| Treatment | Oral agents (e.g., Clonidine) | IV agents (Labetalol, Nicardipine) |
- Special Populations:
- Pregnancy: Use safe agents. 📌 "Hypertensive Moms Love Nifedipine" (Hydralazine, Methyldopa, Labetalol, Nifedipine).
- CKD/Diabetes: ACE inhibitors or ARBs are first-line therapy.
⭐ ACE inhibitors and ARBs are teratogenic and absolutely contraindicated in pregnancy.
High‑Yield Points - ⚡ Biggest Takeaways
- Diagnosis requires ≥2 readings on ≥2 occasions; ambulatory monitoring is the gold standard.
- First-line agents include thiazides, ACE inhibitors/ARBs, and calcium channel blockers.
- ACE inhibitors/ARBs are crucial for patients with CKD, diabetes, or heart failure.
- Beta-blockers are reserved for compelling indications like post-MI or rate control.
- Hypertensive emergency means end-organ damage, requiring immediate IV medication.
- Always consider secondary hypertension in very young or resistant cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

