SVT Overview - The Heart's Short Circuits
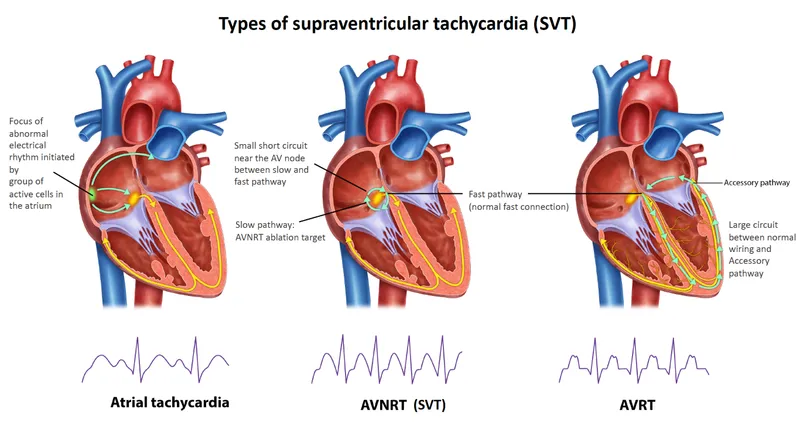
- Definition: Rapid, regular tachyarrhythmias originating above the His bundle.
- ECG Hallmark: Narrow QRS complex (<0.12s) is characteristic, unless there's aberrant conduction.
- Mechanism: Most commonly caused by a re-entrant circuit in the atria or AV node, creating a "short circuit."
- Primary Types:
- AV Nodal Re-entrant Tachycardia (AVNRT): A circuit within the AV node.
- AV Re-entrant Tachycardia (AVRT): Involves an accessory pathway (e.g., WPW syndrome).
- Atrial Tachycardia (AT): An ectopic focus within the atria.
⭐ AVNRT is the most common form of paroxysmal SVT (~60% of cases), frequently presenting in young adults without structural heart disease.
ECG Diagnosis - Reading the Rhythm
- Rate: >100 bpm, regular rhythm.
- QRS: Narrow (<0.12s) unless pre-existing bundle branch block.
- P waves: Key to diagnosis. Assess morphology & relation to QRS (RP interval).
| Rhythm | P wave | RP Interval | Key Feature |
|---|---|---|---|
| AVNRT | Buried in QRS or retrograde (inverted in II, III, aVF) | Short RP (<90ms) | Pseudo R' in V1 or S in inferior leads |
| AVRT | Retrograde, after QRS | Short or Long RP | Look for delta waves (WPW) on baseline ECG |
| AT | Abnormal axis (non-sinus) | Long RP (>90ms) | Warm-up/cool-down phenomenon |
⭐ Vagal maneuvers or adenosine can terminate AVNRT/AVRT by blocking the AV node. In atrial tachycardia or flutter, they will slow the ventricular rate and unmask the underlying atrial activity.
Acute Management - Taming the Tachycardia
- Assess Stability: First, determine if the patient is hemodynamically unstable (e.g., hypotension, altered mental status, shock, ischemic chest pain, acute heart failure).
- 📌 Stable SVT Meds: Adenosine → Beta-blocker → Calcium Channel Blocker.
⭐ In patients with known Wolff-Parkinson-White (WPW) syndrome, avoid AV nodal blockers (adenosine, CCBs, beta-blockers) if they present with an irregular wide-complex tachycardia (AFib with WPW), as this can precipitate VFib. Consider procainamide.
Chronic Control - Preventing Future Flutters
- Pharmacologic Prophylaxis:
- First-line: Beta-blockers (e.g., metoprolol) or non-dihydropyridine calcium channel blockers (verapamil, diltiazem).
- Second-line: Class Ic antiarrhythmics (flecainide, propafenone) for patients without structural or ischemic heart disease.
- Class III agents (sotalol, amiodarone) are also options.
- Definitive Therapy: Catheter Ablation
- Curative treatment of choice for most recurrent, symptomatic SVTs (AVNRT, AVRT, Atrial Flutter).
- High success rate (>95%) and low complication risk.
- Especially indicated for Wolff-Parkinson-White (WPW) syndrome.
⭐ In patients with pre-excitation (WPW) and atrial fibrillation, AV nodal blocking agents are contraindicated as they can precipitate ventricular fibrillation.
- SVT is any regular, narrow-complex tachycardia originating above the His bundle.
- AVNRT is the most common type, caused by a reentrant circuit within the AV node.
- AVRT (e.g., WPW syndrome) involves an accessory pathway; look for a delta wave and short PR interval on baseline EKG.
- Atrial flutter classically presents with a "sawtooth" pattern of P-waves.
- Acute management of stable SVT: attempt vagal maneuvers, then give IV adenosine.
- Any unstable patient requires immediate synchronized cardioversion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

