Electrolyte Arrhythmias - The Ion Imbalance
- Core Principle: Imbalances in key ions ($K^+$, $Ca^{2+}$, $Mg^{2+}$) alter myocardial action potentials, leading to arrhythmias.
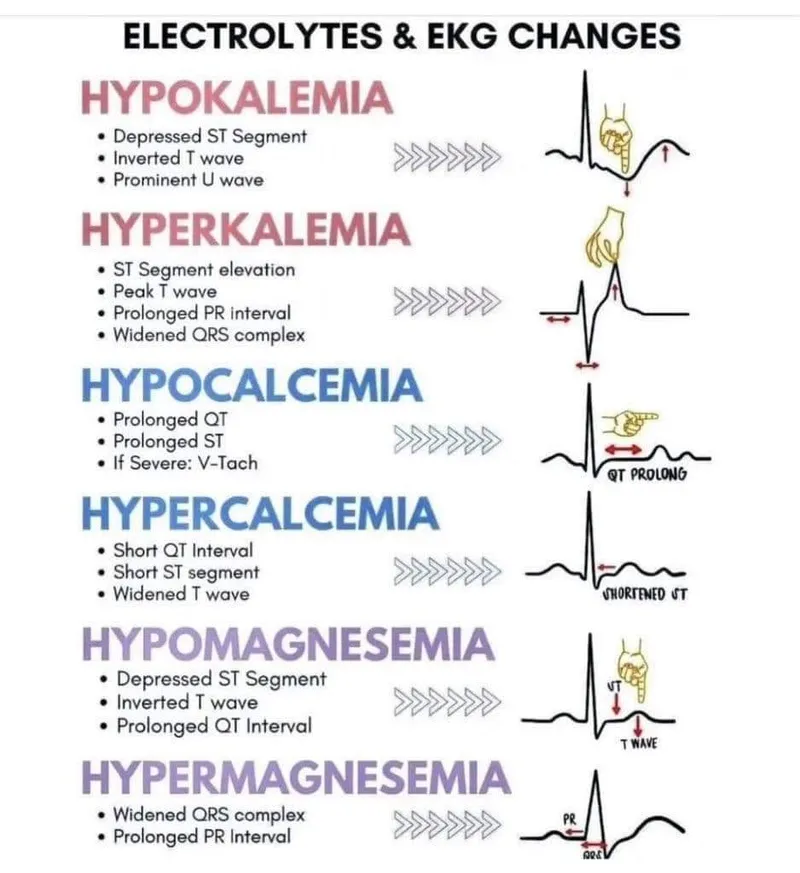
| Electrolyte | ECG Findings | Clinical Notes / Associations |
|---|---|---|
| Potassium ($K^+$) | Hyperkalemia (>5.5): Peaked T waves → Wide QRS → Sine wave. Hypokalemia (<3.5): U waves, Flat T waves, ST depression. | Hyper: Renal failure, ACE-I/ARBs, DKA. Hypo: Diuretics, diarrhea, vomiting. |
| Calcium ($Ca^{2+}$) | Hypercalcemia (>10.5): Short QT interval. Hypocalcemia (<8.5): Long QT interval. | Hyper: Malignancy, hyperparathyroidism. Hypo: Hypoparathyroidism, CKD. |
| Magnesium ($Mg^{2+}$) | Hypermagnesemia (>2.5): ↑PR, Wide QRS (rare). Hypomagnesemia (<1.5): Torsades de Pointes (TdP). | Hyper: Iatrogenic, renal failure. Hypo: Alcoholism, diuretics, PPIs. |
Drug-Induced Arrhythmias - Pharma's Funky Rhythms
Many drugs can prolong the QT interval, increasing the risk for Torsades de Pointes (TdP), a polymorphic ventricular tachycardia. A corrected QT ($QT_c$) interval > 500 ms is a major risk factor.
📌 Mnemonic for QT-prolonging drugs: 'ABCDE'
- Antiarrhythmics (Class IA, III)
- Quinidine, Procainamide, Amiodarone, Sotalol
- Antibiotics (Macrolides, Fluoroquinolones)
- Erythromycin, Azithromycin, Ciprofloxacin
- Anticychotics (Typical & Atypical)
- Haloperidol, Olanzapine, Risperidone
- Antidepressants (TCAs, SSRIs)
- Amitriptyline, Citalopram
- Antiemetics
- Ondansetron, Promethazine
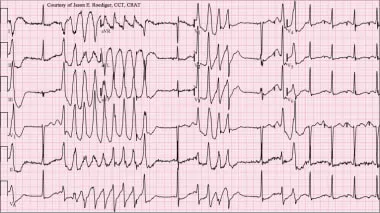
⭐ Exam Favourite: Amiodarone causes significant QT prolongation but has a surprisingly low incidence of Torsades de Pointes compared to other Class III antiarrhythmics.
Clinical Approach - Taming the Rogue Wave
Initial management focuses on stabilization and identifying the underlying reversible cause. The goal is to treat the trigger, not just the rhythm.
⭐ For Torsades de Pointes (TdP), the first-line treatment is IV Magnesium Sulfate, which works by stabilizing the cardiac membrane, even in patients with normal serum magnesium levels.
High‑Yield Points - ⚡ Biggest Takeaways
- Hyperkalemia causes peaked T waves, a widened QRS, and ultimately a sine wave pattern.
- Hypokalemia presents with U waves and flattened T-waves, increasing risk for Torsades de Pointes (TdP).
- Hypomagnesemia is a key cause of refractory TdP, often co-occurring with hypokalemia.
- QT prolongation from drugs (Class IA/III antiarrhythmics, macrolides, antipsychotics) is a major TdP risk.
- Digoxin toxicity classically causes "scooped" ST segments and atrial tachycardia with AV block.
- Remember QT interval effects: hypocalcemia prolongs, while hypercalcemia shortens.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

