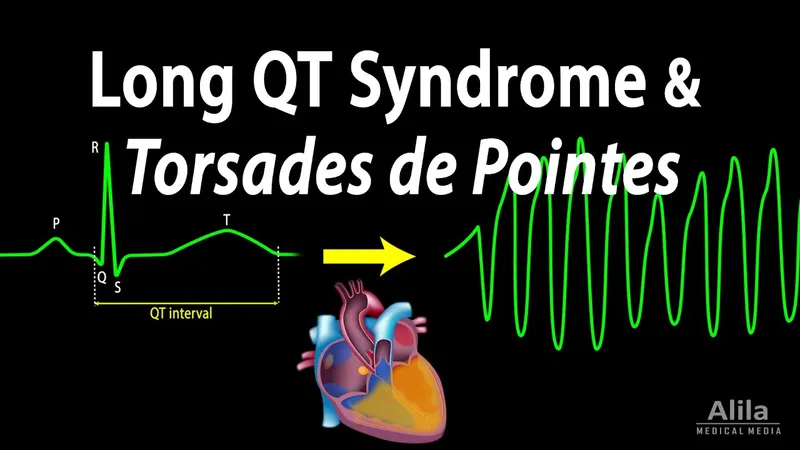
Long QT Syndrome - The Prolonged Pause
- Pathophysiology: Inherited disorder of delayed ventricular repolarization from cardiac ion channel mutations (↓ K⁺ efflux or ↑ Na⁺ influx).
- ECG Hallmark: Rate-corrected QT interval (QTc) prolongation.
- QTc > 450 ms in males
- QTc > 470 ms in females
- Clinical Features: Recurrent syncope, seizures, or sudden cardiac death (SCD), often triggered by exercise, emotion, or auditory stimuli.
- Types:
- Romano-Ward Syndrome: Autosomal dominant, pure cardiac phenotype.
- Jervell and Lange-Nielsen Syndrome: Autosomal recessive, includes congenital sensorineural deafness.
⭐ The hallmark arrhythmia is Torsades de Pointes (TdP), a polymorphic ventricular tachycardia often leading to ventricular fibrillation.
- Management:
- First-line: Beta-blockers (e.g., nadolol, propranolol).
- High-Risk: Implantable Cardioverter-Defibrillator (ICD).
- AVOID: QT-prolonging drugs (e.g., macrolides, fluoroquinolones, antipsychotics).
Brugada Syndrome - Coved Calamity
- Pathophysiology: Autosomal dominant loss-of-function mutation in sodium channels (most commonly SCN5A gene), leading to ↓ Na⁺ current.
- Epidemiology: More common in males of Southeast Asian descent.
- Presentation: Syncope, seizures, or sudden cardiac death (SCD), often nocturnal.
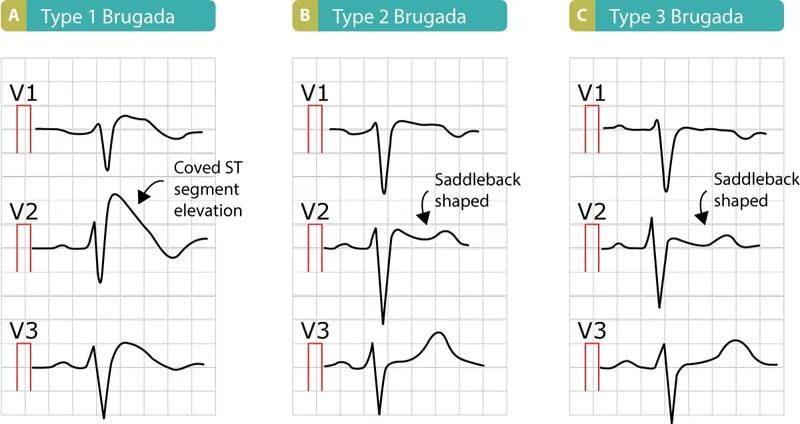
- ECG Findings: Pseudo-RBBB and persistent ST-segment elevation in V1-V2.
- Type 1: Coved ST elevation (≥2 mm) followed by an inverted T-wave.
- Type 2/3: Saddleback ST elevation.
- Triggers: Fever, alcohol, cocaine, and certain medications (e.g., sodium channel blockers, beta-blockers).
- Management: Implantable cardioverter-defibrillator (ICD) is the only proven therapy to prevent SCD.
⭐ Often presents as nocturnal sudden unexplained death syndrome (SUNDS), especially in young Asian males.
ARVC & CPVT - The Stress Syndromes
-
Arrhythmogenic Right Ventricular Cardiomyopathy (ARVC):
- Autosomal dominant; mutations in desmosomal proteins (e.g., PKP2).
- Fibrofatty infiltration of the RV myocardium → ventricular arrhythmias & SCD, especially with exertion.
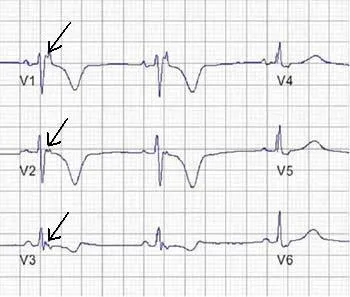
- ECG: T-wave inversions (V1-V3), prolonged S-wave upstroke, and the pathognomonic Epsilon wave.
- Tx: Beta-blockers, ICD placement for high-risk patients.
-
Catecholaminergic Polymorphic VT (CPVT):
- Genetic disorder of intracellular calcium handling (RyR2, CASQ2 mutations).
- Adrenergic stress (exercise, emotion) → massive Ca²⁺ release → delayed afterdepolarizations.
- Presents with syncope or SCD in childhood/adolescence.
- Tx: High-dose beta-blockers (nadolol), flecainide; ICD.
⭐ CPVT is classically associated with bidirectional ventricular tachycardia during exercise stress testing.
- Brugada syndrome shows a coved ST-elevation in leads V1-V3, often triggered by fever.
- Long QT Syndrome (LQTS) presents with Torsades de Pointes (TdP); avoid QT-prolonging drugs.
- Arrhythmogenic Right Ventricular Cardiomyopathy (ARVC) involves fibrofatty replacement of the RV myocardium and may show an epsilon wave.
- Catecholaminergic Polymorphic VT (CPVT) causes bidirectional VT with exercise or emotion.
- These are primarily ion channelopathies that increase risk of sudden cardiac death (SCD).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

