Cardioversion vs. Defibrillation - Shocking The System
A timed, lower-energy shock to "reset" an unstable, perfusing tachyarrhythmia versus a high-energy, untimed shock to "reboot" a pulseless, life-threatening one.
| Feature | Cardioversion | Defibrillation |
|---|---|---|
| Timing | Synchronized with QRS (R-wave) | Unsynchronized (anytime) |
| Rhythm | Unstable AFib/AFlutter, SVT, VT with a pulse | Pulseless VT, Ventricular Fibrillation (VF) |
| Energy | Lower, escalating doses (e.g., 50-200J) | Higher, max dose (e.g., 200-360J) |
⭐ Synchronization is Key: Cardioversion delivers a shock synchronized with the R-wave to avoid the vulnerable T-wave period. An unsynchronized shock on the T-wave (R-on-T phenomenon) can induce lethal ventricular fibrillation.
The Procedure - Paddles & Placement
- Paddle Size:
- Adults: 8-12 cm diameter.
- Pediatrics: 4.5 cm for infants (<10 kg), 8-12 cm for children (>10 kg).
- Conductive Medium:
- Essential to reduce transthoracic impedance and prevent skin burns.
- Use pre-made pads or apply conductive gel.
- Placement Options:
- Anterolateral (Standard):
- Sternal paddle: Right of the upper sternum, below the clavicle.
- Apex paddle: 5th-6th intercostal space, left mid-axillary line.
- Anteroposterior (AP).
- Anterolateral (Standard):
⭐ AP Placement: Often preferred for cardioverting atrial fibrillation/flutter and is necessary for patients with an implanted pacemaker or ICD to avoid delivering energy through the device.
Synchronized Cardioversion - Timing is Everything
- Principle: A low-energy shock timed precisely to the QRS complex's R-wave.
- Goal: Resets the heart's electrical activity, allowing the SA node to regain control.
- Mechanism: The "sync" mode avoids the vulnerable T-wave period, preventing the dangerous R-on-T phenomenon which can trigger Ventricular Fibrillation.
- Indications: Unstable tachyarrhythmias with a pulse (e.g., A-fib, A-flutter, VT with pulse).
- Energy: Lower than defibrillation; start at 50-100 J (biphasic).
⭐ If the patient becomes pulseless, abandon cardioversion and proceed immediately to high-energy defibrillation and CPR.
Defibrillation - The Un-Syncable Shock
- Principle: An unsynchronized, high-energy electrical shock used for pulseless life-threatening arrhythmias.
- Indications:
- Ventricular Fibrillation (VF)
- Pulseless Ventricular Tachycardia (pVT)
- Mechanism: Depolarizes the entire myocardium simultaneously, terminating the chaotic rhythm and allowing the sinus node to regain control.
- Energy: Biphasic (120-200 J); Monophasic (360 J).
⭐ The most critical factor for survival in VF/pVT is minimizing the time to defibrillation. Minimize interruptions in chest compressions before and after the shock.
Risks & Reminders - Handle With Care
- Thromboembolism: High risk in AF/Aflutter >48h. Mandates 3-4 weeks of anticoagulation before and after, OR a pre-procedure TEE to exclude thrombus.
- Complications: Includes skin burns (use gel/pads correctly), transient myocardial stunning, and post-shock arrhythmias like bradycardia.
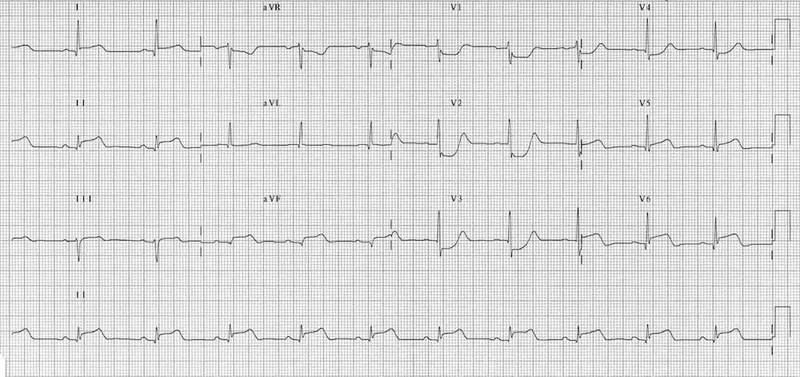
⭐ Post-cardioversion ST-segment elevation can be a benign, transient finding-not always acute MI.
High‑Yield Points - ⚡ Biggest Takeaways
- Synchronized cardioversion treats unstable tachyarrhythmias with a pulse (e.g., Afib, VT with pulse), avoiding the vulnerable T-wave period.
- Unsynchronized defibrillation is for pulseless VT and VF only, delivering a high-energy, non-timed shock.
- PEA and asystole are non-shockable rhythms; treat with high-quality CPR and epinephrine.
- Defibrillation uses higher energy (e.g., 120-200J biphasic) than cardioversion (e.g., 50-100J for SVT/Afib).
- Administer sedation/analgesia before cardioverting a conscious patient.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

