STEMI Diagnosis - Spotting the Enemy
- ECG within 10 minutes of first medical contact is critical.
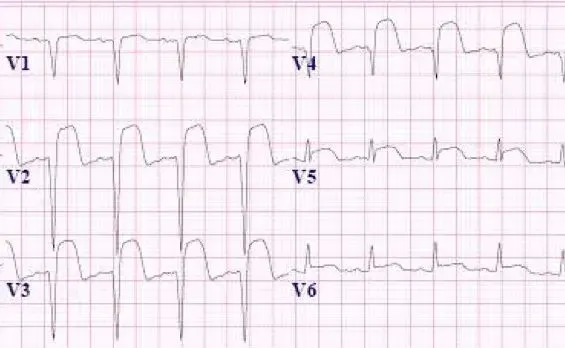
- Diagnostic Criteria: ST-segment elevation in ≥2 contiguous leads.
- ≥1 mm in most leads.
- V2-V3: ≥2 mm (men ≥40), ≥2.5 mm (men <40), ≥1.5 mm (women).
- New or presumed new LBBB with ischemic symptoms is a STEMI equivalent.
- Cardiac Biomarkers: ↑ Troponin I or T (highly sensitive/specific).
⭐ Posterior Wall MI: Often missed! Look for ST depression in V1-V3 (reciprocal changes). Confirm with ST elevation in posterior leads (V7-V9).
Acute Management - First Response
- Immediate Actions: 12-lead ECG within 10 min, establish IV access, cardiac monitoring, O₂ if SpO2 <90%.
- Initial Medical Therapy:
- Aspirin 325 mg (chewed) & P2Y12 inhibitor (e.g., ticagrelor).
- Nitroglycerin (sublingual/IV). ⚠️ Caution in RV MI, hypotension, or severe aortic stenosis.
- Morphine for refractory chest pain.
- Anticoagulation (unfractionated heparin or LMWH).
⭐ The cornerstone of STEMI care is timely reperfusion. The target for primary PCI is a door-to-balloon time of < 90 minutes.
Reperfusion Therapy - Opening the Gates
Primary Percutaneous Coronary Intervention (PCI) is the gold standard. The choice between PCI and fibrinolysis is critically time-dependent, aiming to restore coronary blood flow immediately.
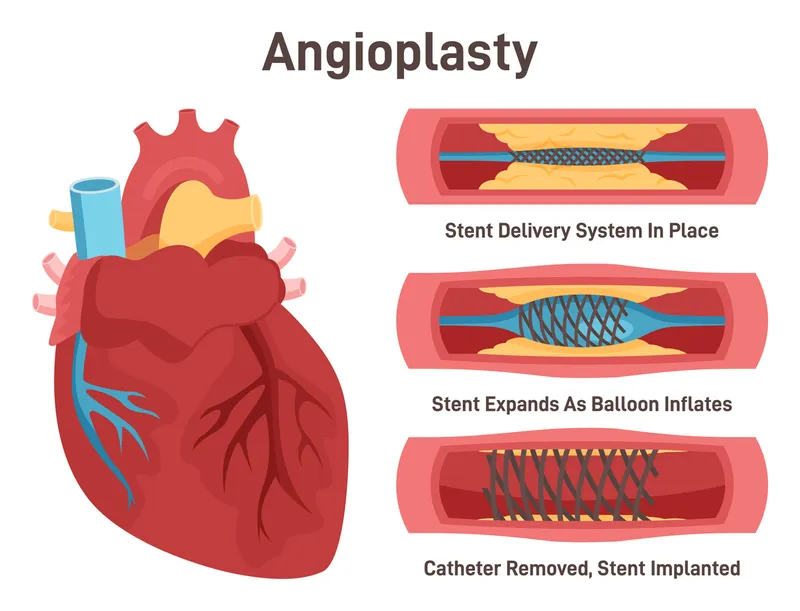
- PCI (Angioplasty with Stent): Preferred strategy.
- Goal: First Medical Contact (FMC) to device time < 90 minutes in a PCI-capable hospital.
- If transfer needed, FMC-to-device < 120 minutes.
- Fibrinolysis (tPA, tenecteplase):
- Use if timely PCI is unavailable.
- Goal: Door-to-needle time < 30 minutes.
- ⚠️ Contraindicated in patients with prior intracranial hemorrhage or active bleeding.
⭐ All patients receiving fibrinolysis should be transferred to a PCI-capable center for routine angiography and potential intervention within 3-24 hours.
Post-MI Care - The Long Road Back
- Goal: Prevent reinfarction, manage complications, and improve long-term survival.
- Secondary Prevention Medications (Post-MI Cocktail):
- Dual Antiplatelet Therapy (DAPT): Aspirin (lifelong) + P2Y12 inhibitor (e.g., clopidogrel) for at least 12 months.
- Beta-Blockers: Continue for ≥3 years; lifelong if HF or LVEF <40%.
- High-Intensity Statins: Atorvastatin 80 mg or Rosuvastatin 40 mg for all.
- ACE Inhibitors / ARBs: Especially with anterior MI, HF, or LVEF <40%.
- Aldosterone Antagonists: (e.g., spironolactone) if LVEF <40% with HF symptoms or diabetes.
- Lifestyle is Key:
- Cardiac rehabilitation, smoking cessation, diet, exercise.
- Complication Watchlist:
- Arrhythmias: ↑VT/VF risk. Consider ICD if LVEF <35% after 40 days.
- Pericarditis: Early vs. late (Dressler's).
- Structural: Aneurysm, mural thrombus, rupture.
⭐ Dressler Syndrome: Autoimmune pericarditis occurring weeks to months post-MI. Presents with fever, pleuritic chest pain, and a friction rub. Treat with NSAIDs/colchicine.
- Classic symptom: Substernal chest pain radiating to the jaw/arm; be aware of atypical presentations (women, diabetics).
- ECG diagnosis: New ST-elevation (≥1 mm) in ≥2 contiguous leads or a new LBBB.
- Immediate reperfusion is critical: PCI within 90 minutes is the gold standard over thrombolysis.
- Use thrombolysis (tPA) only if PCI is unavailable within 120 minutes of first medical contact.
- For right ventricular (RV) infarcts, avoid nitrates/morphine and give IV fluids to maintain preload.
- Aspirin (162-325 mg) should be administered immediately to all patients with suspected ACS.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

