Atypical ACS - Not The Classic Crush
- Elderly (>75y) & Renal Dysfunction (CKD): Classic anginal chest pain is often absent. A high index of suspicion is key.
- Common Atypical Symptoms:
- Dyspnea (most common)
- Syncope, weakness, fatigue
- Delirium/acute confusion
- Epigastric pain, nausea/vomiting
- Diagnostic Challenges:
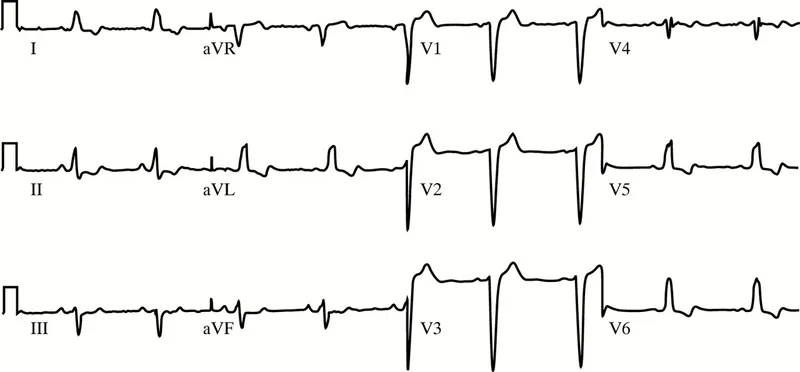
- ECG: Often non-specific. Pre-existing LBBB, LVH, or pacing can obscure STEMI findings.
- Troponins:
- Chronically elevated in CKD due to ↓ clearance.
- Diagnosis requires a dynamic change: a rise/fall of >20% from baseline is significant.
⭐ In patients with advanced CKD, a baseline troponin should be established. A subsequent rise of >20% within hours strongly suggests acute MI, even if the absolute value is high at baseline.
Diagnostic Quirks - Reading The Signals
-
Elderly Patients (>75y): Atypical is Typical
- Symptoms: Dyspnea on exertion is the most common anginal equivalent. Also watch for syncope, weakness, confusion, or epigastric pain. Classic chest pain is often absent.
- ECG: Frequently confounded by pre-existing LBBB, LVH, or pacemaker rhythms, reducing ST-segment specificity.
-
Chronic Kidney Disease (CKD) Patients:
- Biomarkers: Baseline troponin (cTnT & cTnI) is often chronically elevated due to decreased renal clearance.
- Diagnosis hinges on dynamic change: a significant rise and/or fall in serial troponin levels is required.
⭐ In CKD, a >20% change in serial high-sensitivity troponin (hs-cTn) within hours is a key indicator for acute MI, valued over a single absolute number.
Treatment Tweaks - Handle With Care
-
Elderly (>75y): Atypical presentation (e.g., syncope, delirium) is common. Reduced metabolic clearance increases bleeding risk.
- Lower threshold to reduce or withhold P2Y12 inhibitors or anticoagulants.
- Fibrinolysis: Dose reduction for tenecteplase; increased intracranial hemorrhage risk.
-
Renal Dysfunction (CKD): Drug accumulation is a major concern. Always calculate CrCl.
- Anticoagulants: Dose adjustments are critical. Avoid certain agents.
- Contrast: Risk of contrast-induced nephropathy (CIN). Hydrate well; use low-osmolar contrast.
⭐ High-Yield: In patients >75 years receiving fibrinolytics for STEMI, the risk of intracranial hemorrhage significantly increases. Half-dose tenecteplase may be considered.

- Elderly patients often present with atypical symptoms like syncope, weakness, or delirium, delaying ACS diagnosis.
- Silent MIs are significantly more common in the elderly and in patients with diabetes.
- Baseline ECG abnormalities (e.g., LBBB, LVH) can obscure STEMI diagnosis in older adults.
- Renal dysfunction is a major bleeding risk factor; requires careful dose adjustment of anticoagulants (e.g., LMWH, bivalirudin).
- Contrast-induced nephropathy (CIN) is a key risk during angiography in patients with CKD; pre-procedure hydration is critical.
- Avoid NSAIDs in all ACS patients, but especially those with renal issues, due to ↑ thrombotic risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

