NSTEMI Pathophysiology - The Unstable Plaque
-
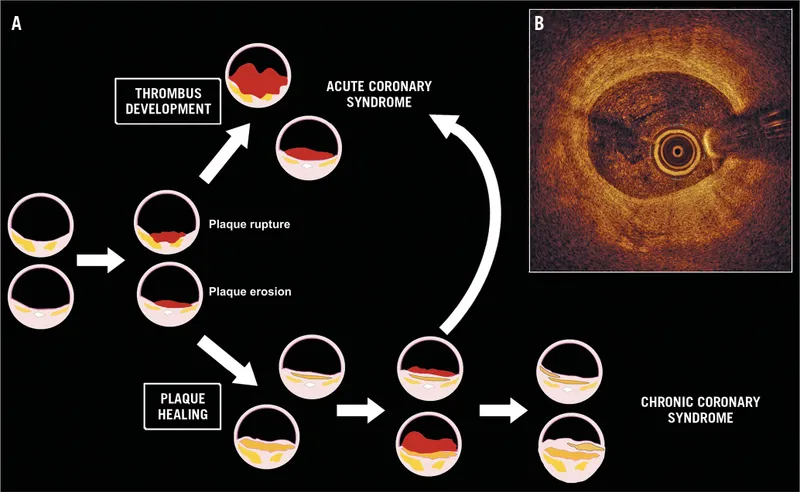
Core Mechanism: Rupture of an atherosclerotic plaque triggers platelet aggregation and thrombus formation.
- The key distinction is a partially occlusive thrombus, which limits but doesn't eliminate blood flow.
- This leads to subendocardial ischemia and necrosis, hence the elevated cardiac biomarkers (Troponins).
-
Spectrum of ACS:
- Unstable Angina: Ischemia without necrosis (negative biomarkers).
- STEMI: A fully occlusive thrombus causing transmural ischemia.
⭐ Plaque rupture most commonly occurs at the shoulder region of the fibrous cap, an area weakened by inflammatory cells.
NSTEMI Diagnosis - The Clinical Picture
- Clinical Presentation: Substernal chest pain >20 min, often with dyspnea, diaphoresis, or nausea. Atypical symptoms (fatigue, epigastric pain) common in women, diabetics, and the elderly.
- ECG Findings: Key ischemic changes include ST-segment depression (≥0.5 mm) or dynamic T-wave inversions (≥1 mm). A normal ECG does not rule out NSTEMI.
- Cardiac Biomarkers: High-sensitivity cardiac troponin (hs-cTn) is the gold standard.
- Serial measurements (e.g., at 0 and 1-3 hours) are crucial.
- Look for a characteristic rise and/or fall pattern.
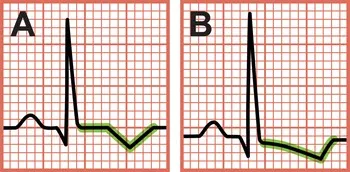
⭐ A normal initial ECG occurs in up to 20% of NSTEMI cases; repeat ECGs are essential if clinical suspicion remains high.
Risk Stratification - Scoring the Danger
Guides timing of intervention (invasive vs. conservative).
-
TIMI Score: Predicts 30-day risk of death, MI, or revascularization.
- Age ≥65
- Markers (positive cardiac)
- EKG (ST deviation ≥0.5 mm)
- Risk factors for CAD (≥3: HTN, HLD, DM, smoking, family hx)
- Ischemia (≥2 anginal events in 24h)
- CAD (known, stenosis ≥50%)
- Aspirin use in past 7 days
- 📌 Mnemonic: AMERICA
-
GRACE Score: More complex, but more accurate for in-hospital & long-term mortality.
⭐ The GRACE score is superior to the TIMI score in predicting mortality, especially in higher-risk patients.
NSTEMI Management - The Action Plan
- Initial Medical Therapy:
- DAPT: Aspirin + P2Y12 inhibitor (e.g., Ticagrelor).
- Anticoagulation: Unfractionated or LMW Heparin.
- Beta-blockers: Metoprolol (cardioselective).
- Statin: High-intensity (e.g., Atorvastatin 80 mg).
- Nitrates for angina relief.
⭐ In patients with NSTEMI and cardiogenic shock or refractory angina, emergent (<2h) coronary angiography is recommended.
High-Yield Points - ⚡ Biggest Takeaways
- NSTEMI is an ACS with positive cardiac biomarkers (troponin) but no ST-segment elevation on EKG.
- It is differentiated from Unstable Angina by the presence of elevated troponins, indicating myocardial necrosis.
- Initial management includes dual antiplatelet therapy (DAPT)-Aspirin plus a P2Y12 inhibitor-and anticoagulation.
- Risk stratification with TIMI or GRACE scores is crucial to guide therapy toward an early invasive strategy.
- Beta-blockers reduce myocardial oxygen demand; nitrates provide symptom relief.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

