Differential Diagnosis - The Possibilities Game
- Goal: Generate a list of potential diagnoses, then refine based on clinical data.
- Frameworks: Build a broad initial list.
- 📌 VINDICATE: Vascular, Inflammatory/Infectious, Neoplastic, Degenerative, Iatrogenic/Intoxication, Congenital, Autoimmune, Traumatic, Endocrine/Metabolic.
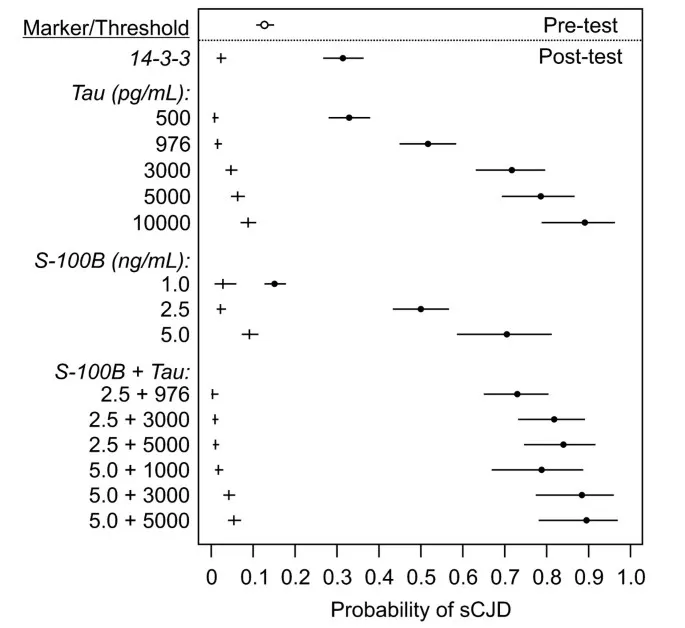
- Probability Ranking: Dynamically re-order the differential list.
- Start with pre-test probability (prevalence).
- Incorporate findings (H&P, tests) to calculate post-test probability.
- Uses Bayes' Theorem: $P(A|B) = \frac{P(B|A)P(A)}{P(B)}$
⭐ High positive likelihood ratios (LR+) dramatically increase post-test probability, often confirming a diagnosis. An LR+ > 10 is considered strong evidence.
Building Differentials - Casting the Net
- The initial phase of diagnostic reasoning involves generating a comprehensive list of potential diagnoses. This "casting a wide net" approach helps prevent premature closure on a single, often incorrect, diagnosis.
- A structured approach is crucial. Organize potential causes by system (e.g., cardiovascular, respiratory) or by a pathological mnemonic.
- 📌 VINDICATE is a powerful tool for building a broad differential:
- Vascular (ischemia, hemorrhage)
- Inflammatory / Infectious
- Neoplastic (primary vs. metastatic)
- Degenerative / Deficiency
- Iatrogenic / Intoxication
- Congenital
- Autoimmune / Allergic
- Traumatic
- Endocrine / Metabolic
- 📌 VINDICATE is a powerful tool for building a broad differential:
⭐ When building a differential for any presenting complaint, always include the most common conditions and the most life-threatening conditions, even if they seem less likely. This dual approach balances probability with patient safety.
Probability Ranking - Playing the Odds
Ranking differentials involves moving from a broad list to a prioritized one using probabilistic reasoning. This is a dynamic process, constantly updated with new data.
- Pre-Test Probability: The baseline chance of a disease before new information. Based on demographics, risk factors, and chief complaint. A 25-year-old with chest pain has a low pre-test probability for coronary artery disease.
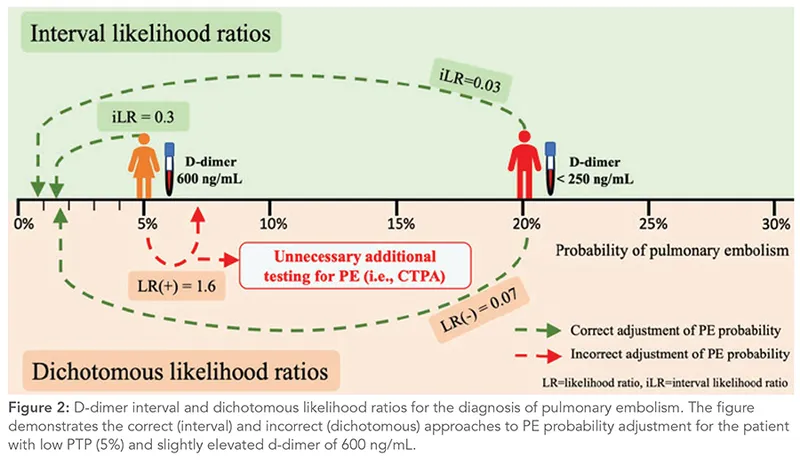
- Likelihood Ratios (LRs): The power of a finding (from history, exam, or tests) to change our suspicion.
- LR+ >10 strongly suggests the disease.
- LR- <0.1 strongly argues against it.
- Post-Test Probability: The updated probability after considering the findings. Calculated as: $Pre-test , odds \times LR = Post-test , odds$.
⭐ On exams, if a classic "textbook" presentation is described, the pre-test probability for that specific disease is artificially high for the question's purpose.
Cognitive Biases - Avoiding Mind Traps
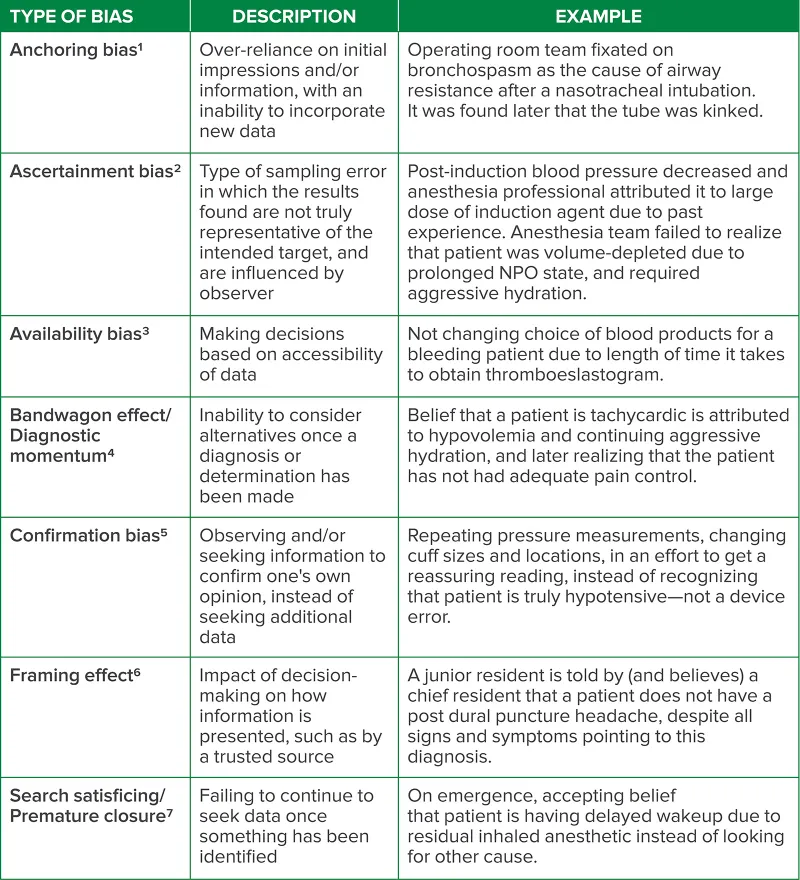
- Anchoring Bias: Over-relying on initial information (e.g., the first symptom).
- Availability Heuristic: Overestimating diagnoses that are recent or memorable.
- Confirmation Bias: Seeking evidence that supports your initial impression.
⭐ Premature closure, a top cause of diagnostic error, is anchoring bias in action-stopping the process too soon.
📌 Guard against by asking: "What else could this be?"
High‑Yield Points - ⚡ Biggest Takeaways
- Prevalence is paramount; common diseases are the most likely culprits in a differential.
- Patient demographics (age, sex) and key risk factors are critical for refining probabilities.
- An atypical presentation of a common disease is more probable than a classic presentation of a rare disease.
- Always prioritize ruling out life-threatening "can't-miss" diagnoses, regardless of their initial probability.
- The best-fit diagnosis explains the entire clinical picture with the fewest assumptions (Occam's razor).
- Continuously update probabilities as new data from labs and imaging becomes available.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

