Hypothetico-Deductive Model - The Diagnostic Detective
A conscious, systematic process applying the scientific method to clinical problem-solving. It involves generating and testing diagnostic hypotheses based on patient data.
- Core Loop: Iterative cycle of data collection, hypothesis formation, and refinement.
- Primary Users: Essential for trainees and learners; also used by experts for complex or atypical cases.
- Cognitive Cost: More deliberate and resource-intensive than rapid pattern recognition.
⭐ High-Yield Pitfall: Beware of premature closure. This cognitive bias involves accepting a diagnosis too early, ceasing to gather further data or consider other reasonable alternatives, which can lead to diagnostic errors.
The H-D Workflow - From Clue to Conclusion
- A cyclical process of refining diagnostic possibilities from initial patient encounters to a final conclusion. It integrates new data to continuously update the likelihood of each potential diagnosis.
- Cue Acquisition: Gathering raw data: patient history, physical exam findings, initial lab results.
- Hypothesis Generation: Formulating an initial, broad list of potential causes (differential diagnosis) based on early cues and established illness scripts.
- Data Interpretation & Refinement: Sequentially interpreting new information (e.g., imaging, specialized labs) to support or refute hypotheses. The list of differentials is narrowed until a working diagnosis is established.
⭐ Cognitive Bias Alert: Avoid premature closure-the tendency to stop the diagnostic process once a plausible diagnosis is found, failing to consider other reasonable alternatives.
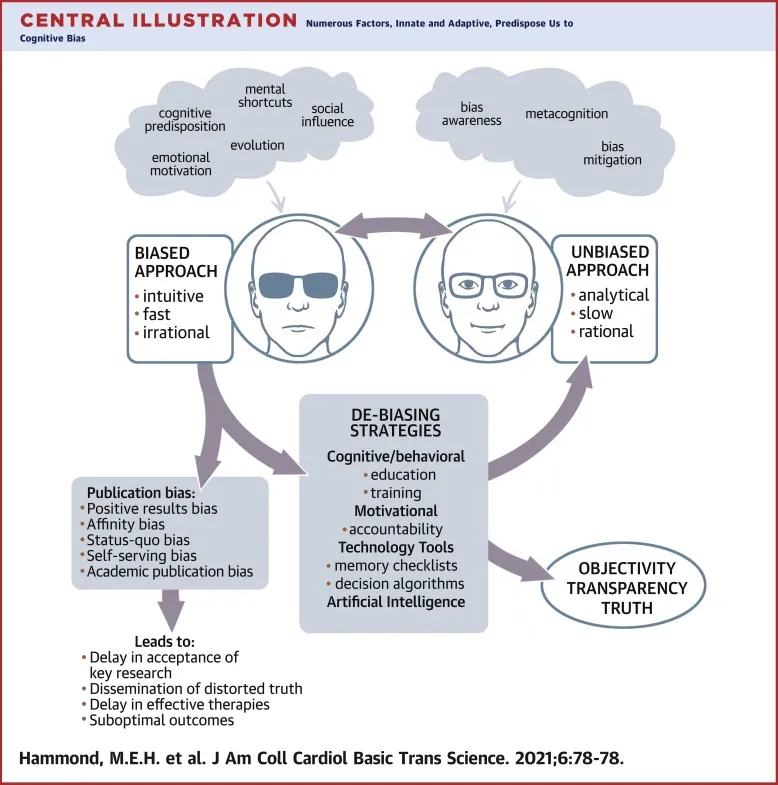
Cognitive Biases - Navigating Mind Traps
Cognitive biases are systematic errors in thinking that affect clinical judgment and decision-making, often leading to diagnostic errors. Awareness is the first step to mitigation.
- Anchoring Bias: Over-reliance on initial information (e.g., a previous diagnosis or the first symptom mentioned).
- Availability Heuristic: Judging likelihood by how easily examples come to mind (e.g., overdiagnosing a rare disease after seeing a recent case).
- Confirmation Bias: Seeking and favoring information that confirms one's initial hypothesis while ignoring contradictory evidence.
- Premature Closure: Accepting a diagnosis too early, failing to consider other reasonable alternatives. This is a common and dangerous bias.
⭐ Studies suggest that cognitive biases contribute to 10-15% of diagnostic errors. Actively considering alternatives ("What else could this be?") is a key debiasing strategy.
High‑Yield Points - ⚡ Biggest Takeaways
- Hypothetico-deductive reasoning is a conscious, systematic process of generating and testing diagnostic hypotheses based on clinical data.
- It involves four key steps: cue acquisition, hypothesis generation, data interpretation, and hypothesis evaluation.
- This analytical approach is crucial for complex or atypical cases and is often used by less experienced clinicians.
- It stands in contrast to pattern recognition (non-analytic reasoning), which is faster but more prone to error in unusual presentations.
- The process is iterative, constantly refining the differential diagnosis as more information becomes available.
- A major pitfall is susceptibility to cognitive biases, especially confirmation bias.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

