Intro to CDRs - Predict, Don't Guess
- Standardized, evidence-based tools that quantify probabilities to guide patient management.
- Goal: Improve accuracy, reduce unnecessary testing, and standardize care.
- Types of CDRs:
- Diagnostic: Rule-in or rule-out a condition (e.g., Wells' Criteria for DVT/PE).
- Prognostic: Estimate probability of future outcomes (e.g., CHADS₂-VASc for stroke risk).
- Therapeutic: Guide treatment choices (e.g., CURB-65 for pneumonia).
⭐ A CDR is only as good as its validation. It must be externally validated in a population different from the one it was derived in before widespread clinical use.
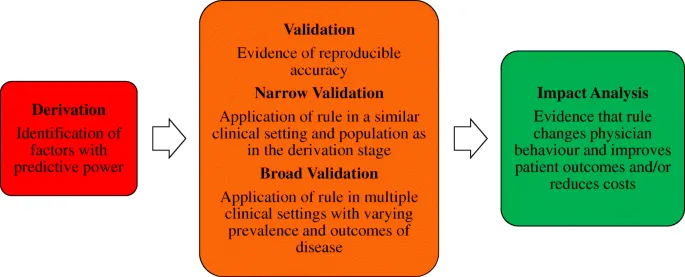
📌 DVI: Derivation → Validation → Impact analysis.
CDR Validation - Making a Good Rule
- 1. Derivation:
- An initial study identifies key predictors from a single patient group.
- Statistical methods (e.g., logistic regression) are used to create the rule.
- 2. Validation:
- The rule's performance is tested in a new set of patients.
- Internal: Same setting, different patients. Checks reproducibility.
- External: Different setting/population. Assesses generalizability. This is the most critical step.
- 3. Impact Analysis:
- Evaluates if the rule improves patient outcomes, reduces costs, or changes clinical behavior.
⭐ A CDR is only ready for clinical use after robust external validation demonstrates its accuracy and utility in diverse populations.
High-Yield CDRs - Rules of the Game
- Wells' Criteria (PE/DVT): Stratifies risk to guide diagnostic testing (D-dimer vs. CTPA).
- PE Score >4: PE likely → Consider CTPA.
- PE Score ≤4: PE unlikely → D-dimer first.
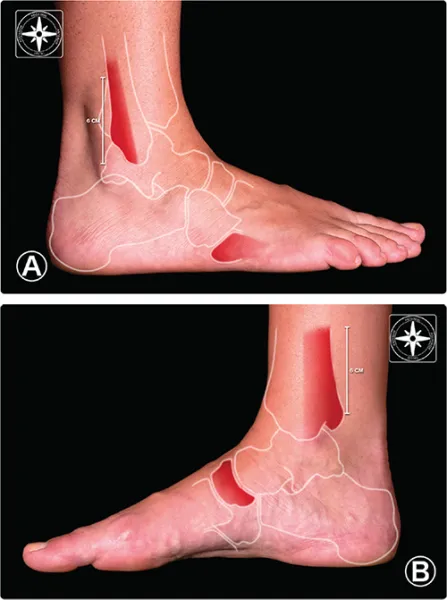
- Ottawa Ankle Rules: Determines need for ankle/foot X-ray after injury.
- X-ray if: Pain in malleolar zone AND (
- Bone tenderness at posterior edge/tip of lateral/medial malleolus OR
- Inability to bear weight 4 steps immediately and in ED).
- X-ray if: Pain in malleolar zone AND (
- NEXUS Criteria: Clears C-spine clinically. Requires ALL 5 to be negative:
- No posterior midline cervical tenderness
- No evidence of intoxication
- Normal level of alertness
- No focal neurologic deficit
- No painful distracting injuries
- Centor Criteria (Strep Pharyngitis): Estimates probability of Group A Strep.
- Score ≥3 suggests rapid strep testing/culture.
⭐ In low-risk PE patients (Wells' score <2), the PERC rule (Pulmonary Embolism Rule-out Criteria) can obviate the need for D-dimer testing, with a miss rate of <2%.
Benefits & Pitfalls - A Double-Edged Sword
-
Benefits:
- Standardizes care, reducing practice variation.
- Improves diagnostic accuracy and efficiency.
- ↓ Unnecessary testing, costs, and patient harm.
- Provides objective, evidence-based guidance for decisions.
- Excellent tool for clinician education.
-
Pitfalls:
- Oversimplification of complex clinical scenarios.
- May discourage critical thinking ("cookbook medicine").
- Risk of misapplication or calculation errors.
- Can become outdated with new evidence.
⭐ High-Yield: A rule's accuracy may drop significantly if applied to populations outside its original validation cohort (e.g., different age, ethnicity, comorbidities).
High‑Yield Points - ⚡ Biggest Takeaways
- Clinical Decision Rules (CDRs) are tools using clinical findings to standardize patient care and improve diagnostic accuracy.
- They aid in risk stratification, helping decide which patients need further testing (e.g., Wells' Criteria for PE/DVT).
- CDRs are meant to supplement, not replace, a clinician's judgment, which remains essential.
- Their validity is limited to the specific populations in which they were studied and validated.
- Key examples include Ottawa Ankle Rules, NEXUS C-spine criteria, and CURB-65 for pneumonia severity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

