Iron (Fe) - The Rusty Workhorse
-
Core Functions: Component of heme (hemoglobin, myoglobin) & cytochromes (electron transport chain). Essential for oxygen transport and cellular respiration.
-
Metabolism & Regulation
- Absorption: Occurs in the duodenum as Fe²⁺. DMT1 is the primary transporter.
- Transport: Transferrin binds Fe³⁺ in the blood.
- Storage: Ferritin stores iron intracellularly. Hemosiderin is an insoluble storage form, visible in overload.
⭐ High-Yield: Hepcidin, a hormone synthesized by the liver, is the master regulator of iron homeostasis. It degrades ferroportin, blocking iron release from enterocytes and macrophages, thus ↓ serum iron. Inflammation (↑ IL-6) stimulates hepcidin.

- Deficiency: Microcytic, hypochromic anemia. Symptoms: fatigue, koilonychia (spoon nails), pica. Labs: ↓ ferritin, ↑ TIBC, ↓ serum Fe.
- Overload (Hemochromatosis): Cirrhosis, "bronze diabetes," cardiomyopathy. Labs: ↑ ferritin, ↓ TIBC, ↑ serum Fe, ↑ transferrin saturation > 45%.
Zinc (Zn) - The Cellular Guardian
-
Function: Essential cofactor for >100 enzymes, including metalloproteinases, carbonic anhydrase, and lactate dehydrogenase. Crucial for forming transcription factors (zinc fingers) and for immune function (T-cell differentiation).
-
Deficiency: Leads to delayed wound healing, hypogonadism, decreased adult hair, dysgeusia (impaired taste), anosmia, and immune suppression.
- Acrodermatitis enteropathica: Classic triad of dermatitis (perioral, acral), alopecia, and diarrhea.
⭐ Delayed wound healing and a pustular, crusted rash around the mouth and on the extremities should immediately raise suspicion for zinc deficiency.
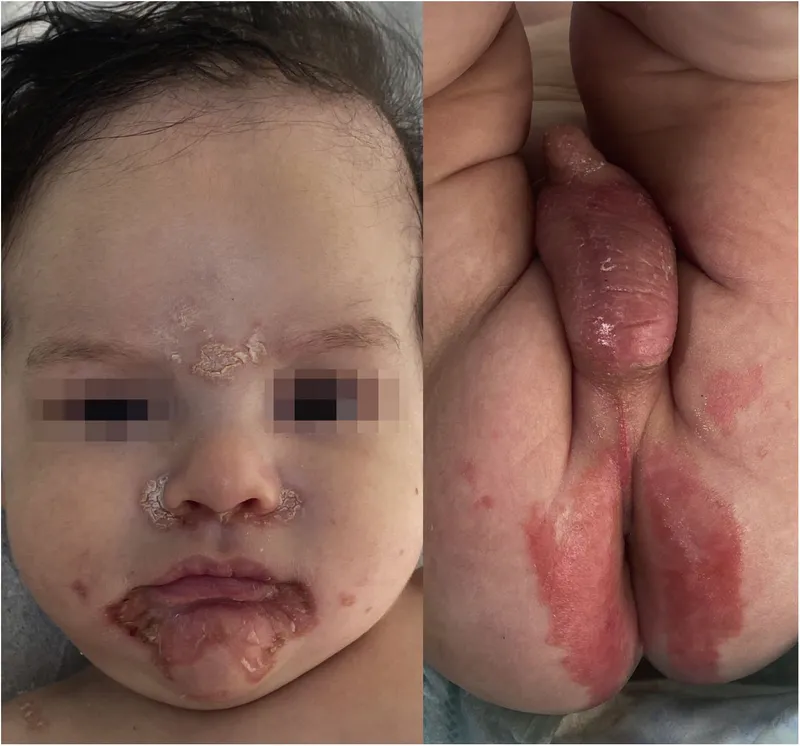
📌 Mnemonic: Remember "ZINC" for deficiency findings: Zits (rash), Immune dysfunction, No taste/smell, Crazy hair loss (alopecia).
Copper (Cu) - The Conductor Mineral
- Function: Cofactor for critical enzymes.
- Lysyl oxidase: Collagen & elastin cross-linking.
- Cytochrome c oxidase: Mitochondrial energy production (Complex IV).
- Dopamine β-hydroxylase: Catecholamine synthesis.
- Ceruloplasmin: Binds Cu; ferroxidase activity (Fe²⁺ → Fe³⁺) for iron transport.
- Deficiency: Microcytic anemia, neutropenia, brittle/kinky hair, hypotonia, osteoporosis.
⭐ Wilson's disease is treated with copper chelators (penicillamine, trientine) and oral zinc, which interferes with copper absorption.
Se & I - Thyroid & Antioxidant Duo
-
Selenium (Se): Cofactor for glutathione peroxidase (antioxidant defense) and iodothyronine deiodinase (converts T4 to active T3).
- Deficiency: Keshan disease (cardiomyopathy), muscle pain, impaired immunity.
- Toxicity: Selenosis (garlic breath, hair loss, neuropathy).
-
Iodine (I): Essential component for thyroid hormone (T4 & T3) synthesis.
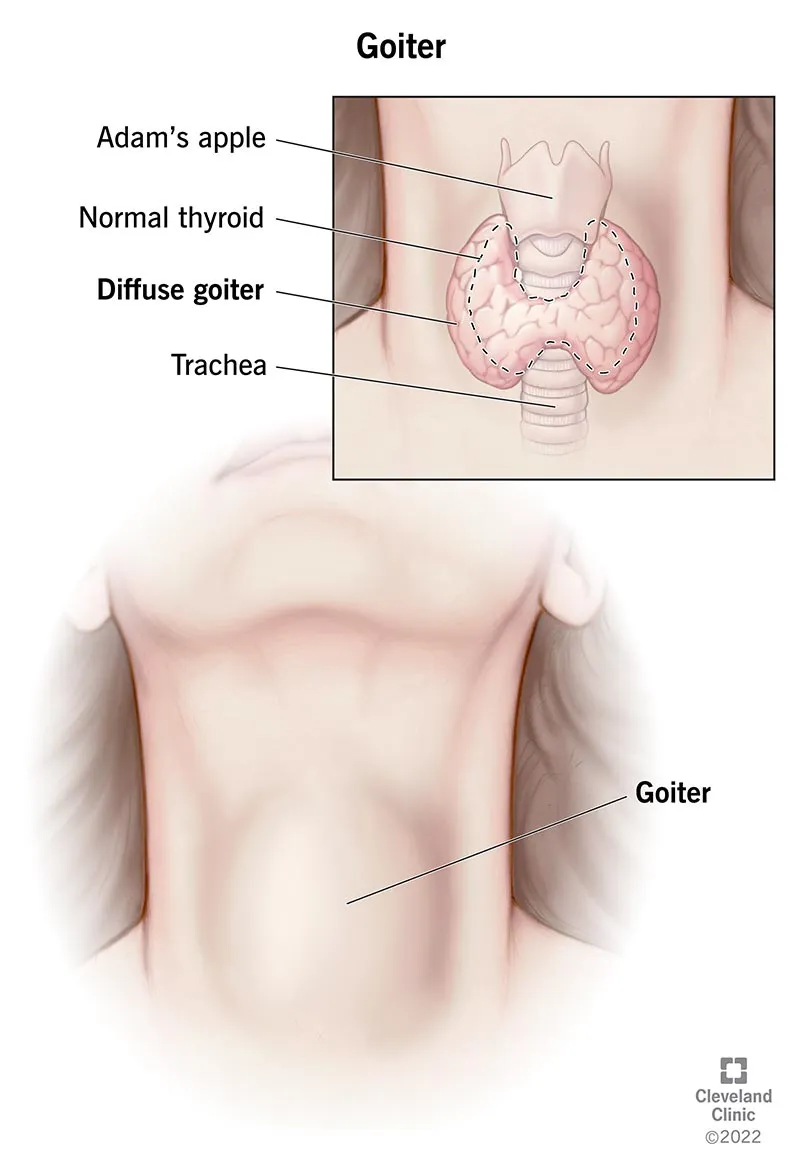
- Deficiency: Goiter, hypothyroidism. Severe congenital deficiency causes cretinism.
- Toxicity: Can induce hypo- or hyperthyroidism (Wolff-Chaikoff & Jod-Basedow effects).
⭐ Selenium deficiency can exacerbate iodine deficiency disorders by impairing T4→T3 conversion.
High‑Yield Points - ⚡ Biggest Takeaways
- Iron deficiency causes microcytic, hypochromic anemia; look for Plummer-Vinson syndrome (dysphagia, webs).
- Zinc deficiency presents with acrodermatitis enteropathica, impaired wound healing, and anosmia.
- Copper deficiency can lead to sideroblastic anemia and mimics vitamin B12 deficiency neurologically.
- Menkes disease is characterized by brittle, kinky hair due to impaired copper absorption.
- Selenium deficiency is associated with Keshan disease (cardiomyopathy).
- Iodine deficiency is a leading cause of preventable goiter and hypothyroidism.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

