Iron Deficiency - The Rusty Engine
- Etiology: Chronic blood loss (GI bleed, menses), malnutrition/absorption issues, or increased demand (pregnancy).
- Clinical: Fatigue, pallor, glossitis, cheilosis. Pica (craving non-food items), koilonychia (spoon nails).
- Labs: ↓ Ferritin (first indicator), ↓ serum Fe, ↑ TIBC, ↓ transferrin saturation (<15%). Anemia is microcytic, hypochromic (↓ MCV, ↓ MCH).
⭐ Plummer-Vinson Syndrome: A classic triad of dysphagia (due to esophageal webs), glossitis, and iron deficiency anemia. 📌 Mnemonic: WEBS (Webs, Esophageal, Beefy-red tongue, Swallowing difficulty).
Iodine & Selenium - Thyroid's Tandem
-
Iodine: Integral component of thyroid hormones (thyroxine/T4 & triiodothyronine/T3).
- Deficiency: ↓ T3/T4 → ↑ TSH → goiter.
- Severe deficiency: Cretinism (infants), myxedema (adults).
- Sources: Iodized salt, seafood, dairy.
-
Selenium: Essential cofactor for 5'-deiodinase, the enzyme that converts T4 → T3 (active form).
- Also a key part of antioxidant glutathione peroxidase.
- Deficiency: Impairs T3 production, can exacerbate iodine deficiency.
- Associated with Keshan disease (cardiomyopathy).
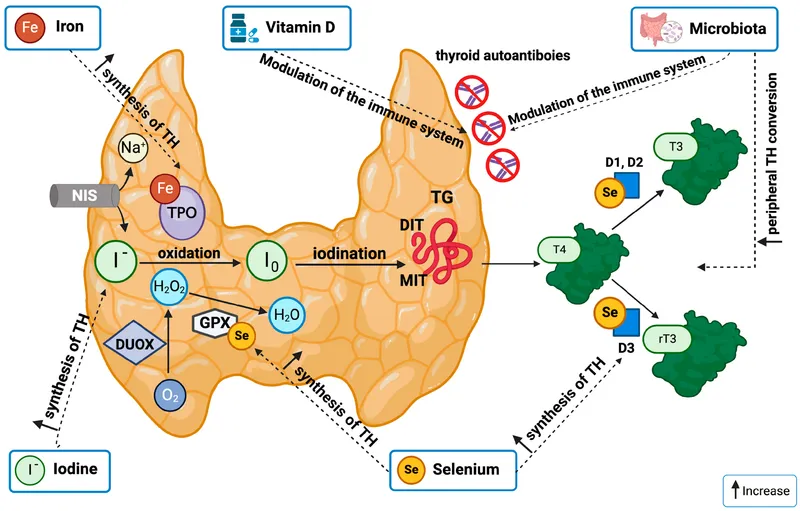
⭐ High-Yield: Selenium deficiency can worsen the effects of concurrent iodine deficiency, leading to more severe hypothyroidism and goiter, as T4 to T3 conversion is impaired.
Copper & Zinc - The Co-factor Crew
-
Copper (Cu): Cofactor for lysyl oxidase (collagen cross-linking), cytochrome c oxidase (electron transport), & dopamine β-hydroxylase.
- Deficiency: Microcytic anemia, neutropenia, ataxia (myelopathy mimicking B12 def.), brittle/depigmented hair.
- Menkes Disease: X-linked recessive (ATP7A gene) → ↓Cu absorption → “kinky hair,” hypotonia, growth failure.
-
Zinc (Zn): Cofactor for >100 enzymes (e.g., carbonic anhydrase) & zinc-finger transcription factors.
- Deficiency: Impaired wound healing, hypogonadism, dysgeusia, anosmia, alopecia.
⭐ Acrodermatitis enteropathica, an inherited Zn malabsorption, presents with a classic triad: periorificial/acral dermatitis, alopecia, & diarrhea.
Other Key Players - The Supporting Cast
- Zinc: Deficiency → Acrodermatitis enteropathica (perioral/acral rash), alopecia, dysgeusia, anosmia, poor wound healing, hypogonadism.
- Copper: Component of lysyl oxidase & cytochrome c oxidase. Deficiency → brittle/kinky hair, microcytic anemia, osteoporosis, neutropenia.
- Selenium: Component of glutathione peroxidase. Deficiency → Keshan disease (cardiomyopathy), myopathy.
- Chromium: Potentiates insulin. Deficiency → impaired glucose tolerance, peripheral neuropathy.
⭐ Menkes disease (X-linked recessive ATP7A defect) causes copper deficiency. Classic findings: brittle, “kinky” hair, growth retardation, and hypotonia.
High‑Yield Points - ⚡ Biggest Takeaways
- Iron deficiency, the most common nutritional disorder, causes microcytic anemia, koilonychia, and pica.
- Iodine deficiency leads to goiter and hypothyroidism; congenital deficiency causes cretinism.
- Copper deficiency (e.g., Menkes disease) presents with brittle, kinky hair, and microcytic anemia.
- Zinc deficiency is marked by acrodermatitis enteropathica, poor wound healing, and anosmia.
- Selenium deficiency is strongly associated with Keshan disease, a severe cardiomyopathy.
- Chromium deficiency can result in impaired glucose tolerance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

