Vitamin A Deficiency - Night Blindness Blues
- Function: Vision (retinal cycle), immune health, and differentiation of epithelial cells. Stored in stellate (Ito) cells of the liver.
- Causes: Malnutrition, fat malabsorption (e.g., celiac disease, cystic fibrosis), or liver disease.
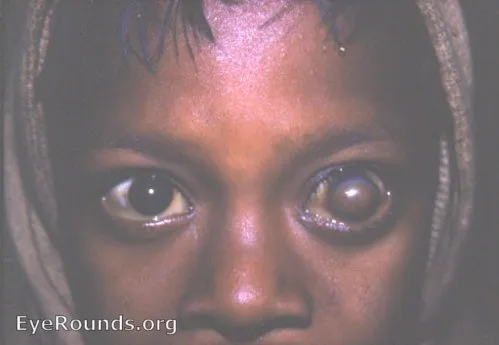
- Ocular Signs (Xerophthalmia):
- Nyctalopia (night blindness) is the earliest symptom.
- Bitot's spots: White, foamy plaques of keratin on the conjunctiva.
- Keratomalacia: Corneal softening, ulceration, leading to irreversible blindness.
- Other Effects: Follicular hyperkeratosis, impaired immunity (↑ risk of measles morbidity).
⭐ Deficiency leads to squamous metaplasia of epithelial linings (e.g., respiratory, urinary tracts), replacing normal mucus-secreting epithelium with keratinized squamous cells.
Vitamin D Deficiency - Brittle Bones Breakdown
- Pathophysiology: Insufficient UV light or dietary intake → ↓ calcitriol (1,25-dihydroxyvitamin D) → impaired intestinal absorption of Ca²⁺ & PO₄³⁻.
- Syndromes:
- Rickets (Children): Defective mineralization of cartilaginous growth plates.
- Bowed legs (genu varum), rachitic rosary (costochondral hypertrophy), craniotabes.
- Osteomalacia (Adults): Defective mineralization of existing bone.
- Diffuse bone pain, muscle weakness, ↑ fracture risk.
- Rickets (Children): Defective mineralization of cartilaginous growth plates.
- Labs: ↓ Ca²⁺, ↓ PO₄³⁻, ↑ PTH (secondary hyperparathyroidism), ↑ alkaline phosphatase.
⭐ On X-ray, osteomalacia classically presents with Looser zones (pseudofractures)-radiolucent bands perpendicular to the cortex, especially in the scapula, pelvis, or femoral neck.

Vitamin E Deficiency - Nerve & RBC Wreck
- Function: Potent lipid-soluble antioxidant. Protects RBC and neuronal cell membranes from free radical-induced oxidative damage.
- Causes: Rare. Primarily from fat malabsorption syndromes (cystic fibrosis, cholestasis) or abetalipoproteinemia.
- Clinical Presentation:
- Hemolytic anemia: Increased RBC fragility leads to acanthocytosis (spur cells) and a shortened RBC lifespan.
- Neurologic Dysfunction: Due to demyelination of posterior columns and spinocerebellar tracts.
- Ataxia
- Peripheral neuropathy
- Loss of proprioception and vibration sense
- Retinopathy: Pigmentary changes that can mimic retinitis pigmentosa.
⭐ Neurologic symptoms can closely mimic Friedreich ataxia. Differentiate by the absence of hypertrophic cardiomyopathy and skeletal deformities (e.g., scoliosis) in Vitamin E deficiency.
Vitamin K Deficiency - The Bleeding Problem
- Function: Essential cofactor for γ-glutamyl carboxylase, which activates clotting factors II, VII, IX, X and anticoagulant proteins C & S.
- Etiology: Malabsorption (Crohn's, cystic fibrosis), broad-spectrum antibiotics (↓ gut flora), and newborns (sterile gut, poor placental transfer).
- Labs & Clinical: ↑ PT is the earliest indicator (Factor VII's short half-life), later followed by ↑ aPTT. Normal bleeding time. Presents with easy bruising, mucosal bleeding, melena, and hematuria.
⭐ Warfarin acts as a Vitamin K antagonist by inhibiting the enzyme Vitamin K epoxide reductase, preventing the regeneration of active Vitamin K.
High‑Yield Points - ⚡ Biggest Takeaways
- Vitamin A deficiency presents with night blindness, xerophthalmia (dry eyes), and corneal Bitot spots.
- Vitamin D deficiency causes rickets in children and osteomalacia in adults, leading to defective bone mineralization.
- Vitamin E deficiency can cause hemolytic anemia and neurologic dysfunction (e.g., spinocerebellar ataxia).
- Vitamin K deficiency impairs clotting factor synthesis, causing a prolonged PT/INR and bleeding risk.
- Deficiencies are common in fat malabsorption syndromes like cystic fibrosis and cholestasis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

