TCA Cycle - The Cell's Powerhouse
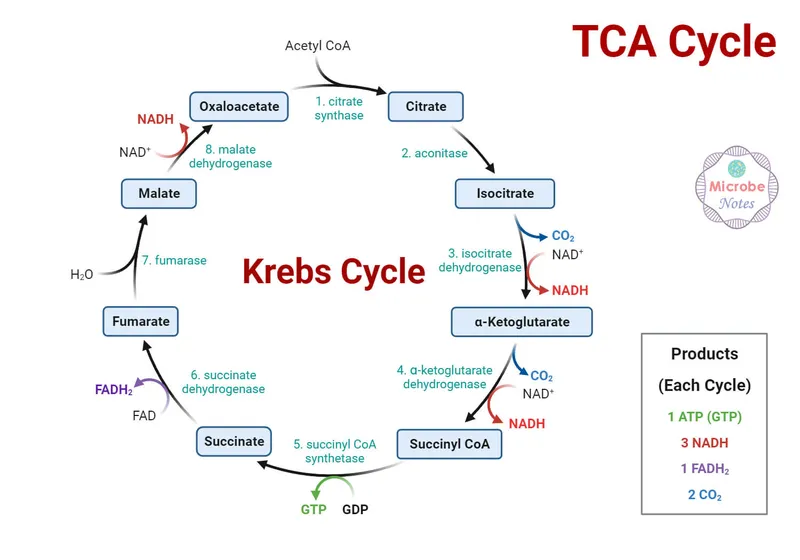
- Location: Mitochondrial matrix.
- Function: Oxidizes Acetyl-CoA, generating 3 NADH, 1 FADH₂, 1 GTP, and $2CO_2$ per cycle.
- Key regulated enzymes:
- Citrate Synthase (inhibited by ATP, citrate)
- Isocitrate Dehydrogenase (Rate-limiting): activated by ADP; inhibited by ATP, NADH
- α-Ketoglutarate Dehydrogenase: activated by Ca²⁺; inhibited by succinyl-CoA, NADH
⭐ Amphibolic pathway: provides precursors for other pathways like gluconeogenesis (malate) and heme synthesis (succinyl-CoA).
📌 Mnemonic: Citrate Is Kreb's Starting Substrate For Making Oxaloacetate.
TCA Cycle Steps - An Enzymatic Merry‑Go‑Round
- Location: Mitochondrial matrix.
- Process: A sequence of 8 enzymatic reactions that oxidizes acetyl-CoA.
- Initiation: Acetyl-CoA (2C) + Oxaloacetate (4C) → Citrate (6C).
- 📌 Mnemonic (Substrates): Citrate Is Krebs' Starting Substrate For Making Oxaloacetate.
⭐ The TCA cycle itself produces very little ATP directly (one GTP/ATP per cycle). Its primary role is to generate a large number of high-energy electrons in the form of NADH and FADH₂, which then fuel the major ATP production via the electron transport chain.
TCA Regulation - Speed Bumps & Green Lights
Regulated by cellular energy status. High energy (↑ATP, ↑NADH) slows the cycle; low energy (↑ADP, ↑NAD⁺) speeds it up.
- Citrate Synthase (Irreversible)
- Inhibitors (Speed Bumps): ATP, NADH, Citrate, Succinyl-CoA.
- Isocitrate Dehydrogenase (Rate-Limiting Step)
- Activators (Green Lights): ADP, Ca²⁺.
- Inhibitors: ATP, NADH.
- α-Ketoglutarate Dehydrogenase (Irreversible)
- Activators: Ca²⁺.
- Inhibitors: NADH, Succinyl-CoA.
⭐ In active muscle, ↑Ca²⁺ not only triggers contraction but also stimulates Isocitrate Dehydrogenase and α-Ketoglutarate Dehydrogenase, boosting ATP production to meet demand.
Yield & Links - TCA's Grand Central Station
- Net Yield (per Acetyl-CoA):
- 3 NADH
- 1 FADH₂
- 1 GTP (ATP equivalent)
- 2 CO₂
- Total Energy: Approx. 10 ATP per turn via oxidative phosphorylation.
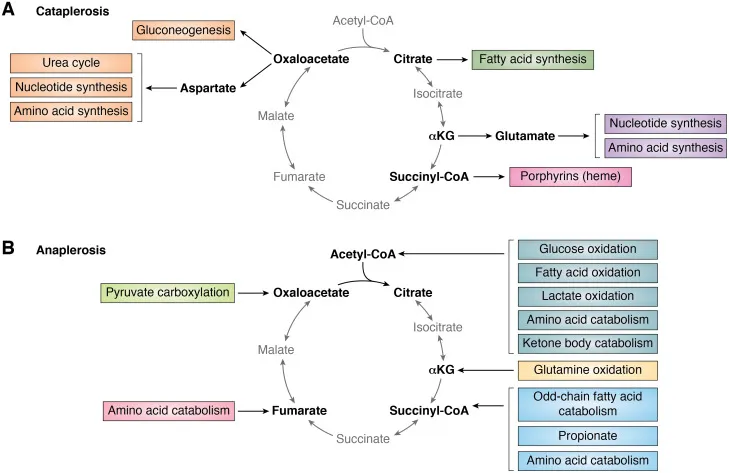
- Metabolic Crossroads: TCA intermediates are hubs for biosynthesis.
- Citrate → Fatty Acid Synthesis
- α-Ketoglutarate → Amino Acid Synthesis (e.g., Glutamate)
- Succinyl-CoA → Heme Synthesis
- Malate → Gluconeogenesis
⭐ The TCA cycle is amphibolic (both catabolic and anabolic). Anaplerotic ("filling up") reactions, like pyruvate carboxylase converting pyruvate to oxaloacetate, are vital to replenish intermediates siphoned off for biosynthesis.
- The TCA cycle occurs in the mitochondrial matrix, generating 3 NADH, 1 FADH₂, and 1 GTP per Acetyl-CoA.
- Key irreversible enzymes are Citrate Synthase, Isocitrate Dehydrogenase, and α-Ketoglutarate Dehydrogenase.
- Isocitrate dehydrogenase is the primary rate-limiting enzyme.
- The cycle is activated by indicators of low energy (ADP, Ca²⁺) and inhibited by indicators of high energy (ATP, NADH).
- It's an amphibolic pathway, supplying precursors for gluconeogenesis and heme synthesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

